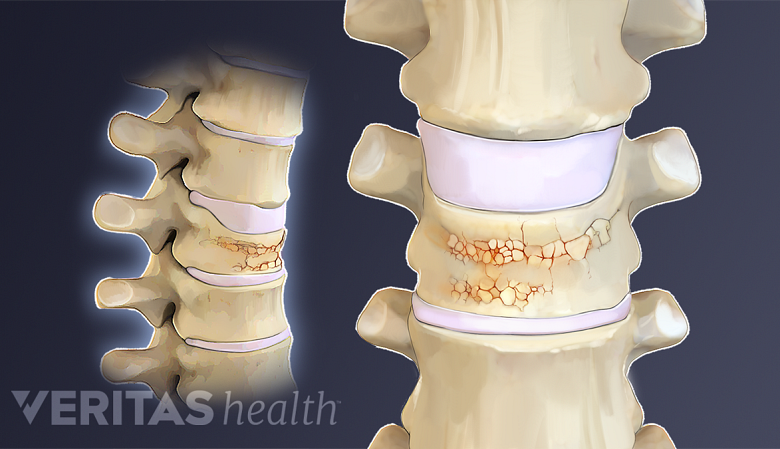
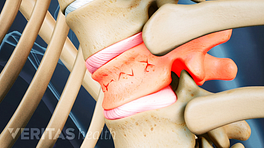
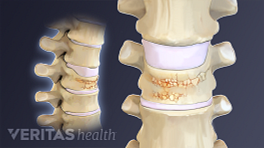
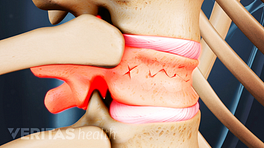
Maintaining strong bones as you age can reduce the risk for osteoporosis and related complications, such as painful vertebral compression fractures in the spine. Try these 11 tips to improve your bone health and protect your body.
Participate in weight-bearing exercise
Regularly performing weight-bearing activities is a great way to build and maintain bone mass.
-
Go for a walk or jog.
The pace and frequency of your walks or jogs are up to you. Your doctor or certified personal trainer can help you decide what is appropriate. Typically, 20 to 30 minutes, 3 to 4 times a week is recommended. -
Climb stairs, do bench steps or jumping exercises.
These activities can be a step up in intensity from walking or jogging. They are great for strengthening your bones and getting a vigorous aerobic workout. -
Do resistance or strength training.
A session of lifting, pushing, and pulling weights (or resistance bands) 2 to 3 times per week is good for your bones and promotes overall health.
For people who already have or at risk of developing osteoporosis, check with your health care provider to learn which exercises are best for you.
Make lifestyle changes
Two lifestyle changes that can make a big difference in bone health include:
-
Quit smoking.
Smoking may be a significant risk factor for bone loss. Not only that, smokers are shown to display poorer balance than non-smokers, raising the chances of falling and breaking a bone. 1 Wong PKK, Christie JJ, Wark JD. The effects of smoking on bone health. Clinical Science. 2007;113(5):233-241. -
Avoid excessive alcohol use.
Heavy alcohol consumption interferes with the body’s ability to absorb and regulate calcium, vitamin D, and hormones. It may also increase your risk of bone density loss and bone fracture. 2 Jang H-D, Hong J-Y, Han K, et al. Relationship between bone mineral density and alcohol intake: A nationwide health survey analysis of postmenopausal women. Plos One. 2017;12(6).
Consume plenty of calcium
Calcium helps to keep your bones strong and prevent osteoporosis. It is recommended that adults get 1000 to 1200 mg of calcium daily. 3 Calcium. US National Institutes of Health, Office of Dietary Supplements. https://ods.od.nih.gov/factsheets/Calcium-HealthProfessional/. Updated October 16, 2019. Accessed December 16, 2019.
-
Have fortified oatmeal for breakfast.
One pack of unsweetened instant oatmeal has over 100 mg of calcium 4 FoodData Central. US Department of Agriculture Website. https://fdc.nal.usda.gov. Accessed December 16, 2019. , about 10% of the daily recommended amount. Get the kind that has added nutrients but no added sugar. Combine whole milk, almond milk, or yogurt with your oatmeal for extra calcium. -
Try canned seafood.
Canned sardines, shrimp, and salmon are all packed with calcium and high in protein. Salmon is a great source of omega-3 fatty acids, too. -
Eat more nuts, beans, and leafy greens.
Almonds, walnuts, and pistachios are all rich sources of calcium. Put a few handfuls in a small plastic bag and keep it nearby to snack on. Traditional baked beans and white beans also have a bunch of calcium. Eat them on their own, or add them to a low-sodium soup. Leafy greens also offer a lot of calcium. Collard greens, kale, and bok choy are all good options. -
Consider a calcium supplement.
If your diet alone doesn’t help you to reach the daily recommended amount of calcium, talk to a doctor or pharmacist about adding over-the-counter calcium supplements to your daily routine.
Increase your vitamin D intake
Vitamin D helps your body hold onto bone-strengthening nutrients. Without enough vitamin D, your bones may weaken, increasing the risk of fracture.
-
Eat cereal fortified with vitamin D, eggs, and fatty fish (such as salmon).
These food options are all ways to get the recommended amount of vitamin D, which is 600 international units (IU) per day (or 800 IU for people age 70 or older). 5 Vitamin D. US National Institutes of Health, Office of Dietary Supplements. https://ods.od.nih.gov/factsheets/VitaminD-HealthProfessional/. Updated August 7, 2019. Accessed December 16, 2019. -
Get at least 5 to 10 minutes of daily sun exposure.
Spending a little time in the sunlight helps your body to absorb vitamin D naturally.
Consider putting some or all of these tips into practice. They may help you to maintain bone health and protect your body against osteoporosis.
Learn more:
- 1 Wong PKK, Christie JJ, Wark JD. The effects of smoking on bone health. Clinical Science. 2007;113(5):233-241.
- 2 Jang H-D, Hong J-Y, Han K, et al. Relationship between bone mineral density and alcohol intake: A nationwide health survey analysis of postmenopausal women. Plos One. 2017;12(6).
- 3 Calcium. US National Institutes of Health, Office of Dietary Supplements. https://ods.od.nih.gov/factsheets/Calcium-HealthProfessional/. Updated October 16, 2019. Accessed December 16, 2019.
- 4 FoodData Central. US Department of Agriculture Website. https://fdc.nal.usda.gov. Accessed December 16, 2019.
- 5 Vitamin D. US National Institutes of Health, Office of Dietary Supplements. https://ods.od.nih.gov/factsheets/VitaminD-HealthProfessional/. Updated August 7, 2019. Accessed December 16, 2019.