Axial low back pain can vary widely. It can be a sharp or dull pain, it can be felt constantly or intermittently, and the pain can range from mild to severe.
In This Article:
- Understanding Low Back Pain (Lumbago)
- Diagnosing the Cause of Lower Back Pain
- Axial Back Pain: Most Common Low Back Pain
- Low Back Pain with Referred Pain
- Lumbar Radiculopathy
- Video: What is Lumbago?
Characteristics of Axial Back Pain
The most common type of axial back pain is "mechanical” and is characterized as:
- Low back pain that gets worse with certain activities (e.g. certain sports)
- Low back pain that gets worse with certain positions (e.g. sitting for long periods)
- Low back pain that is relieved by rest
Axial pain represents the most common type of low back pain, and it is usually non-specific – meaning that the anatomical structure responsible for the pain need not be identified because symptoms are usually self-limited and resolve with time.
Area of Pain Distribution
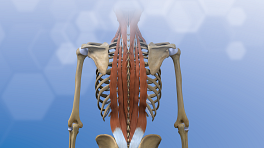
Axial pain is confined to the lower back region.
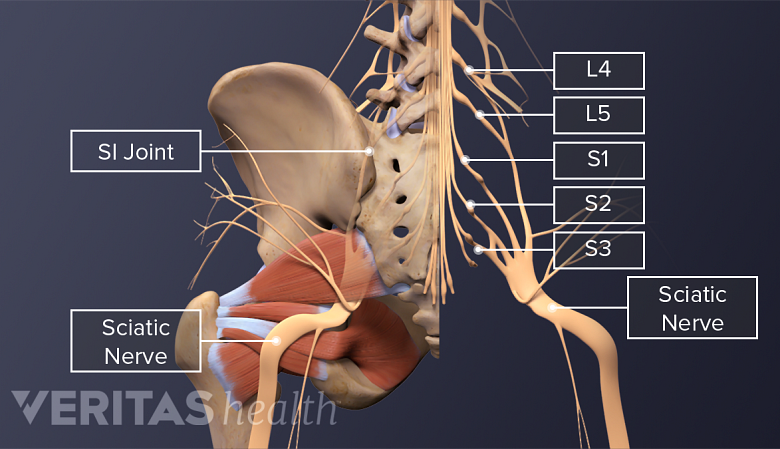
Axial pain is confined to the low back area. Unlike other low back problems, this type of pain does not travel into the buttock, legs and feet, or other areas of the body.
Diagnosis of Axial Back Pain
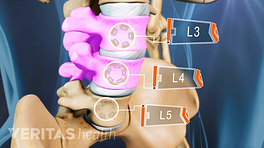
The complex anatomical structures in the back can make it difficult to pinpoint the exact source of pain.
The exact diagnosis as to which structure is causing the low back pain rarely has significance to treatment. Only in chronic and severe cases is further evaluation and diagnosis helpful.
See Special Considerations for a Neck or Back Pain Diagnosis
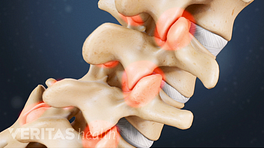
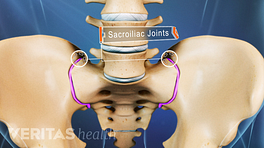
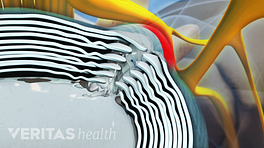
With axial pain, the presence of an anatomical lesion that can be seen on an MRI scan, such as a herniated disc, may have nothing to do with the low back pain episode. This common finding is part of what makes diagnosis difficult. A variety of structures in the low back can cause axial or mechanical lower back pain, such as a degenerated disc, facet joint problems, and damage to soft tissues – muscles, ligaments, and tendons - and it is often difficult to identify which anatomical structure(s) is the underlying cause of the patient’s pain.
As a general rule of thumb, if the back pain is bad enough that it wakes one up from deep sleep, one should consult a physician to rule out possible serious conditions, such as an infection, tumor or fracture.
See How Back Pain Affects Sleep
Treatment of Axial Low Back Pain
Once the possibility of a serious underlying medical condition as the cause of a patient’s low back pain is ruled out, treatment options are non-surgical and may include one or a combination of the following:
- A short period of rest (e.g. one or two days)
- Physical therapy and active exercise and stretching
- Ice and/or heat application for activity related pain relief
- Appropriate medications for pain relief
The natural history of axial low back pain is that with time the symptoms get better, and about 90% of patients with axial low back pain recover within six weeks. If axial low back pain persists for more than six to eight weeks, then additional testing and/or injections may be useful in diagnosing and treating the source of the low back pain.
For patients with severe, chronic low back pain that impedes their ability to function in everyday activities, degenerative disc disease or other problems may be identified as the source of the pain and fusion, disc replacement surgery, or other surgical options may be considered.
It should be emphasized that laminectomy and discectomy surgery is rarely recommended for axial low back pain and is unpredictable as to its successful outcome. These types of back surgery are reserved for pain secondary to compression of the spinal nerve roots or sac.
The surgical and non-surgical treatment of chronic axial back pain (e.g. lasts more than six weeks), is somewhat controversial and beyond the scope of this article. More can be read about ongoing axial back pain in the degenerative disc disease and chronic pain sections of this site.