Treatment for Scheuermann’s disease depends on the individual’s situation. Several factors determining the best treatment include:
- Severity of the curvature in the back
- Amount of flexibility in the area
- Whether the individual is expected to continue to grow
- Concerns about appearance
- Patient preferences
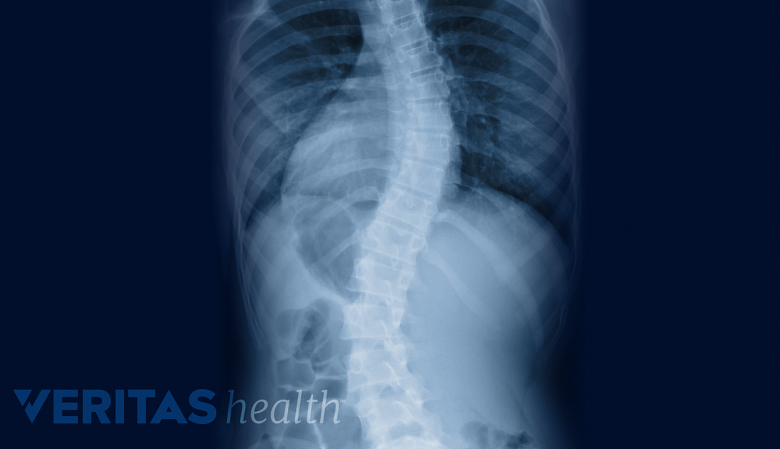
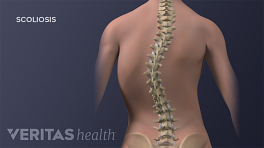
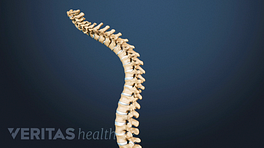
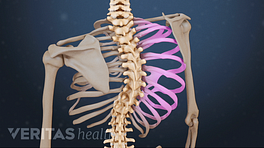
In considering treatments for Scheuermann’s disease, it’s helpful to understand the anatomy of the upper back or thoracic spine. Human spines are designed to curve, but if the curvature reaches 45 degrees or more, it’s considered abnormal. Allowing an abnormal curvature to continue could cause considerable pain and disfigurement over time.
In This Article:
- Scheuermann's Disease of the Thoracic and Lumbar Spine
- Symptoms and Diagnosis of Scheuermann's Disease
- Nonsurgical Treatments for Scheuermann's Disease
- Surgery for Scheuermann's Disease
Observation and Bracing
The doctor periodically takes x-rays to monitor the spine's curvature.
A young person with a slight curvature who is still growing, shows no sign of the curvature worsening, and has mild or no pain may not require intervention. Instead, the individual could be monitored by a doctor and undergo periodic X-rays, or other tests, to track the curvature. If the curvature worsens, more active treatment would be recommended.
A patient with a more advanced curvature—but with more than a year of growth left—would typically receive more intensive treatment. A back brace would usually be prescribed. Braces can stop or reverse the extra curvature during the growing years by making the front of the vertebrae more upright, which may also reduce pain.
To be most effective, braces should be worn almost all the time, at least at first. Depending on the severity and progression of the curvature, patients may be prescribed a brace for one to two years. Braces can be helpful with curvatures of up to 75 degrees. At one time, braces were thought to be ineffective once spine growth was complete, but recent research indicates there is still a good chance of success after growth has ended. 1 Weiss H, Turnbull D, Bohr S. Brace treatment for patients with Scheuermann's disease: A review of the literature and first experiences with a new brace design, Scoliosis. 2009;(4)22.
See Controversy Over Whether Bracing Works
While braces were once considered bulky and uncomfortable—and often rejected by self-conscious teens—the situation has improved considerably and braces have become less obtrusive and more lightweight. Some of these custom-molded braces can be worn undetected under clothes and allow the young person to take part in activities—including many sports.
Many doctors now recommend these kinds of braces, including the kyphologic and thoracolumbosacral (TSLO)-style Boston braces, over the older, larger Milwaukee brace. 2 Yamaguchi KT Jr., Andras L M, Lee C, Skaggs DL. Successful Brace Treatment of Scheuermann’s Kyphosis in Skeletally Mature Patients and Severe Kyphosis. Annals of Orthopedics & Rheumatology. 2014;2(2):1018.
Exercise and Physical Therapy Beneficial
Hamstring stretches promote flexibility and reduce muscle tightness in the low back and legs.
An exercise and physical therapy program, including specific strengthening and hamstring stretching exercises, is often recommended in conjunction with bracing. While exercise won’t correct the deformity, it can be helpful in maintaining flexibility, and alleviating back pain and fatigue.
Low-impact sports, such as low-impact aerobics, swimming, and cycling are preferred. Sports to avoid are those including jumping, high impact, and those likely to cause extra stress or overuse of the back.
Physical therapy can have an educational benefit beyond exercises; it can increase the patient’s awareness of the condition. For the less-common Scheuermann's disease in the lumbar spine, physical therapy will emphasize modifying activity to reduce the chance of developing chronic low back pain in adulthood.
The doctor and/or physical therapist may offer suggestions on ways to live more comfortably with Scheuermann's disease. If pain is bothersome, for instance, taking anti-inflammatory medication (NSAIDs) and use of heating pads may be helpful. Individuals having trouble sleeping may benefit from using extra pillows to help cushion the back.
- 1 Weiss H, Turnbull D, Bohr S. Brace treatment for patients with Scheuermann's disease: A review of the literature and first experiences with a new brace design, Scoliosis. 2009;(4)22.
- 2 Yamaguchi KT Jr., Andras L M, Lee C, Skaggs DL. Successful Brace Treatment of Scheuermann’s Kyphosis in Skeletally Mature Patients and Severe Kyphosis. Annals of Orthopedics & Rheumatology. 2014;2(2):1018.