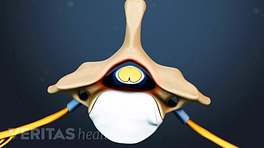
Surgical treatment of spinal stenosis is indicated if non-operative care fails or if there is neurologic loss or deficit, especially if the neurologic loss is progressive. Examples of typical neurologic loss or deficit include symptoms of numbness, weakness, loss of coordination or tingling in the arm or leg.
In This Article:
- Full Range of Surgical Options for Spinal Stenosis
- Lumbar (Low Back) Stenosis Surgery
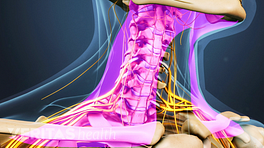
Cervical (Neck) Stenosis Surgery
The most common surgical procedures to alleviate symptoms for cervical spinal stenosis include the following:
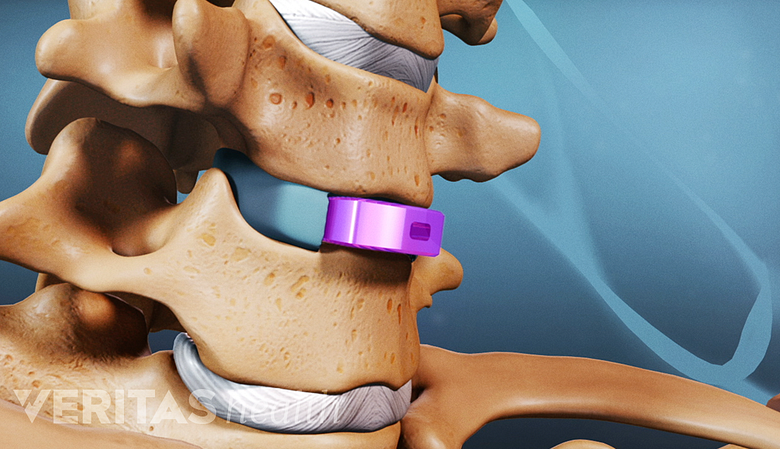
Anterior Disc Replacement
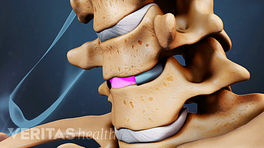
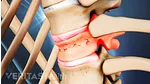
Cervical artificial disc surgery treats central canal and/or foraminal stenosis.
A cervical artificial disc surgery may be an option if stenosis is in the central canal and/or foramen and the facet joints (joints behind the disc are normal).
See Cervical Artificial Disc Replacement Surgery
This procedure can be done as a day surgery procedure or with a one-day hospital stay with return to regular activity within the week and generally a 90% success rate. Long term follow up with level I evidence-based medical studies show better outcomes with fewer revision surgery compared to cervical fusion (ACDF) for most, but not all, stenosis cases.
See Considerations for Cervical Disc Replacement Surgery
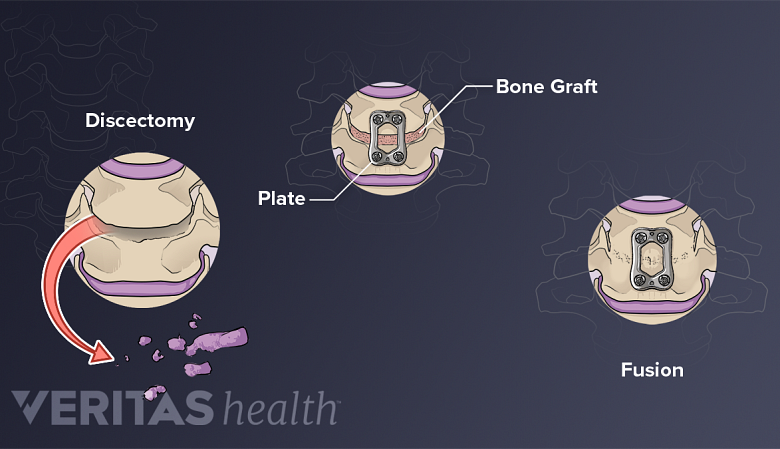
Anterior Cervical Discectomy and Fusion (ACDF)
ACDF is the preferred approach for severe arthritis involving facet joints.
This surgery has been considered the standard of care for stenosis for decades. It is generally very successful for proper indications and good surgical technique. The indications are similar to disc replacement, but typically ACDF will be preferred if the arthritis is more severe with involvement of the facet joints, multiple levels, or deformity, or if the surgeon has more experience with ACDF. More surgeons have extensive experience with an ACDF than with an anterior disc replacement.
See ACDF: Anterior Cervical Discectomy and Fusion
An ACDF can be done as a day surgery procedure, but may be done in the hospital with one-day stay. The return to activity is rapid, usually within weeks.
See ACDF Surgery Postoperative Care
Posterior Foraminotomy
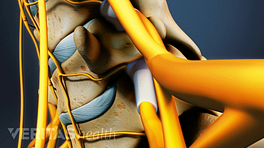
This approach may be indicated when stenosis is due to a herniated disc or bone spur that is located in the area where the nerve root leaves the spinal canal, to the side of the spinal cord.The symptoms include unilateral or one-sided pain, numbness, tingling, or weakness.
A posterior can be done as a day surgery procedure, through a small tube, and generally has a greater than 90% success rate.
See Outpatient Posterior Cervical Foraminotomy and Discectomy
Posterior Laminoplasty
This is a more extensive surgery and is usually reserved for multilevel stenosis and spinal cord compression with dysfunction (cervical myelopathy). There are several indications and contra-indications for this procedure. This type of surgery is done in the hospital setting one or more nights in the hospital. With the correct indications and skilled surgical technique, the results are very good.
See Spinal Cord Compression and Dysfunction from Cervical Stenosis
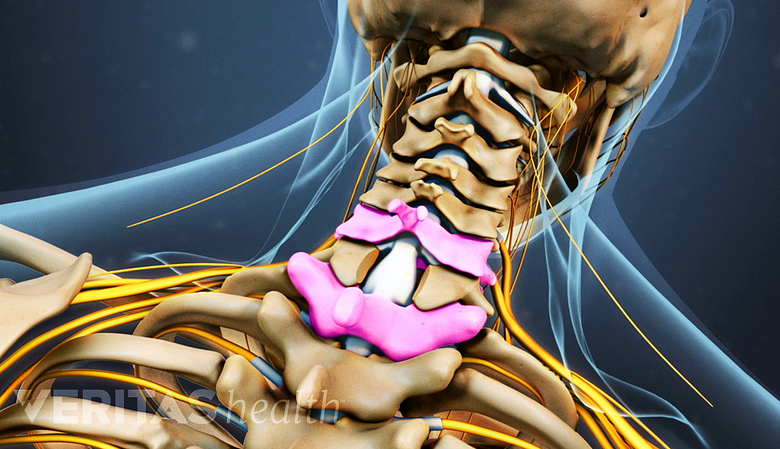
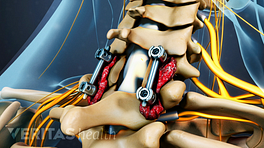
Posterior Laminectomy and fusion
Posterior laminectomy involves removing a portion of the vertebral bone to alleviate nerve compression.
This surgery is done for severe stenosis, deformity, trauma, or tumors at multiple levels. It can be combined with anterior (through the front of the neck) procedures. A posterior cervical surgery is more extensive than an anterior procedure (e.g. an ACDF), so the recovery time is longer.
Posterior Laminectomy
While this surgery is possible, there is no indication for a cervical laminectomy done as a standalone procedure and it can lead to recurrent stenosis, instability, and deformity. An ACDF or posterior laminectomy with a fusion are the usual approaches.
All types of surgery for cervical spinal stenosis have unique advantages and potential risks, and deciding on the type of surgery usually involves a combination of the patient's anatomy and medical condition, the patient's preferences, and the surgeon's experience and preferences.