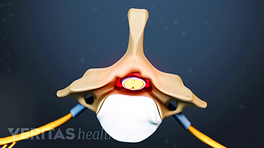
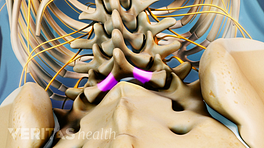
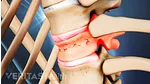
When spinal stenosis results in worsening neurological deficits, such as numbness or weakness, surgery may be considered if nonsurgical treatments have not been effective. The goal of spinal stenosis surgery is to decompress the spinal nerve and/or spinal cord to allow the nerves to start healing and functioning better.
There are several surgical options for spinal stenosis.
In This Article:
Laminectomy
A laminectomy surgery involves the removal of 2 laminae and the spinous process (bony protrusion at the back of the vertebra) that connects them. The vertebral arch normally helps protect the back of the spinal cord. By removing part of the vertebral arch during a laminectomy, the goal is to decompress the spinal cord and nerve roots that were being pinched or inflamed by spinal stenosis. In severe stenosis, parts of one or more enlarged facet joints may also be removed as part of a laminectomy.
Laminectomy is the most common surgery for spinal stenosis. While it is sometimes accompanied by a fusion of adjacent vertebrae to maintain stability, that is not always necessary.
See Lumbar Laminectomy Surgery for Spinal Stenosis (Open Decompression)
Foraminotomy
A foraminotomy surgery removes a small part of the intervertebral foramen (bony opening where the spinal nerve exits the spinal canal). In addition to removing part of the foramen and associated bone spurs, partial removal of the disc and/or other soft tissues that were compressing the spinal nerve in or near the foramen may also be removed.
A foraminotomy is less invasive than a laminectomy, but it is not an option when spinal stenosis is more extensive or widespread.
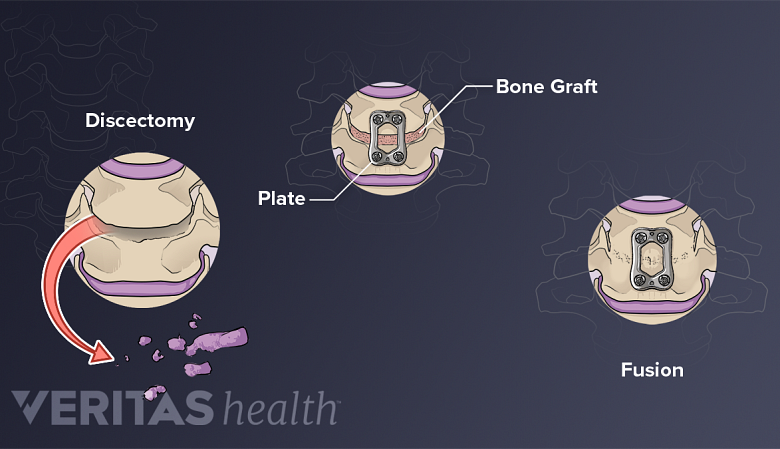
Discectomy and Fusion
If a disc degenerates to the point where the space starts to collapse, the disc may be removed and the vertebrae fused together.
Sometimes disc degeneration plays a key role in narrowing the intervertebral foramen and causing spinal stenosis. In such cases, the collapsing disc space may need to be restored by removing the degenerated disc and fusing the adjacent vertebrae.
There are various surgical methods to accomplish discectomy and fusion. In the neck, the most common method is anterior cervical discectomy and fusion (ACDF)..
Watch Anterior Cervical Discectomy and Fusion (ACDF) Video
In cases when spinal stenosis is extensive or affects multiple levels of the spine, it is likely that a fusion is done in conjunction with other procedures, such as a laminectomy or foraminotomy.
Other Surgical Options for Spinal Stenosis
Some less common surgical techniques for spinal stenosis may include:
Microendoscopic decompression
One surgical option for decompressive surgery is to do the surgery through a tube, known as microendoscopic surgery. The goal of this approach is to minimize the trauma to the soft tissue and allow for earlier recovery. The tradeoff is that this spinal stenosis surgery is harder to do and visualization is limited compared to an open laminectomy. It is a technique that a few surgeons favor, but for spinal stenosis it has not gained widespread usage.
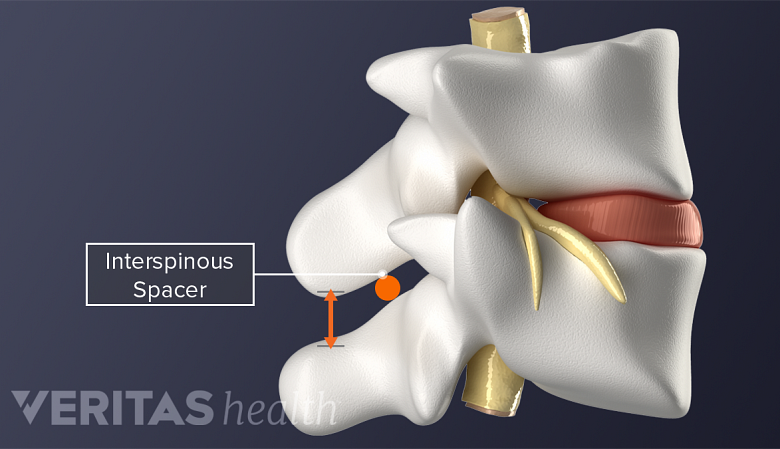
Interspinous process spacers
Placing interspinal spacers between the processes of two vertebrae can be a minimally invasive alternative surgical option for maintaining space in the spinal canal.
Various devices are available that can be implanted between adjacent spinous processes (the bony protrusions at the back of the vertebrae) to increase space within the spinal canal. These devices can be implanted in a minimally invasive way under local anesthesia rather than general anesthesia. More research is needed to determine whether or not interspinous process spacers offer benefits over more traditional surgical options for some cases of spinal stenosis. 1 Li M, Yang H, Wang G. Interspinous process devices for the treatment of neurogenic intermittent claudication: a systematic review of randomized controlled trials. Neurosurg Rev. 2017; 40(4):529-536. doi: 10.1007/s10143-016-0722-y. , 2 Zhao XW, Ma JX, Ma XL, et al. Interspinous process devices (IPD) alone versus decompression surgery for lumbar spinal stenosis (LSS): A systematic review and meta-analysis of randomized controlled trials.
Corpectomy
Rarely performed, a corpectomy involves the complete removal of a vertebral body and the adjacent discs above and below. This surgery is more likely to be performed if spinal stenosis is present at multiple vertebral levels and/or the spinal degeneration is more extensive or involves a fracture.
Other surgical options for spinal stenosis may be available, and new techniques are always being researched.
Spinal Stenosis Surgery Risks
For appropriately selected candidates who have not benefited from nonsurgical treatments, spinal stenosis surgery is a relatively safe and effective treatment. In cases when imaging and/or electrodiagnostic testing do not correspond with the patient’s signs and symptoms, surgery is unlikely to provide benefit and not worth the risk.
As with any surgery, there are potential risks for serious complications, such as:
- Infection
- Excessive bleeding
- Allergic reaction
- Nerve or spinal cord damage
- Failure to relieve pain, worsening pain, or need for a follow-up surgery
The surgeon’s skill, extent of the stenosis, and overall health of the patient are all factors that can affect the likelihood of a good surgical outcome. Before deciding on surgery, it is important that the risks, benefits, and alternatives to the procedure are carefully explained. It is also important for the patient to have all of his or her questions satisfactorily answered.
- 1 Li M, Yang H, Wang G. Interspinous process devices for the treatment of neurogenic intermittent claudication: a systematic review of randomized controlled trials. Neurosurg Rev. 2017; 40(4):529-536. doi: 10.1007/s10143-016-0722-y.
- 2 Zhao XW, Ma JX, Ma XL, et al. Interspinous process devices (IPD) alone versus decompression surgery for lumbar spinal stenosis (LSS): A systematic review and meta-analysis of randomized controlled trials.