Spinal fusion to treat scoliosis is an extensive surgery that is undertaken only after careful consideration of the patient’s options. Typically, surgery may be considered if the following is present
- Scoliosis curve is at least 45 degrees by skeletal maturity. Any sideways spinal curve at least 45 degrees by the time a person has reached skeletal maturity is likely to continue to progress into adulthood. This progression could be about 1 to 2 degrees per year and over time may result in a severe deformity that is more difficult to treat.
- Scoliosis curve is at least 40 degrees despite bracing. If bracing has not stopped the curve’s progress in a growing adolescent, it could make sense to have the surgery before letting the curve reach 45 degrees. Possible benefits include a better correction (smaller curvature means a straighter correction can be made) and less time in a brace.
If neither of the above conditions is met, ongoing observation and bracing is usually recommended.
In This Article:
- Spinal Fusion for Idiopathic Scoliosis
- Scoliosis Surgery: Potential Risks and Complications
How a Spinal Fusion Works
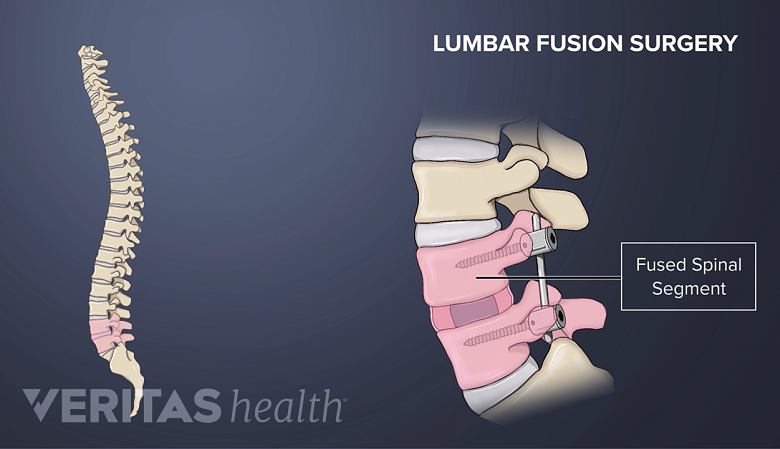
Rods and screws are commonly used in scoliosis surgery to correct and stabilize the spine.
There are several variations to spinal fusion surgery for scoliosis, but most use modern instrumentation systems in which hooks and screws are applied to the spine to anchor long rods. The surgeon then:
- Uses the rods to carefully reposition the spine at the segments affected by scoliosis, correcting the abnormal rotation and reducing the lateral (sideways) curvature; and
- Grafts bone to the vertebral segments that are to be fused. These bone grafts typically come from a donor or bone bank (allograft) or part of the patient’s own bone such as from the patient’s hip (autograft). In recent years, there have also been some bone grafts using synthetic bone substitutes; however, long term results and potential risks are not yet fully known.
See Bone Graft for Spine Fusion
The rods are essentially used as a splint to hold the spine in place while the bones continue to fuse after surgery is completed. The initial fusion process usually takes about 3 to 6 months, and the fusion will usually continue to take hold for up to 12 months.
See Scoliosis Surgery Recovery: 3 Months Post-Operation and Beyond
Once the fusion has set up, the spine’s shape and position are held in place by its long, newly-fused bone (not the rods). The rods are generally not removed since this would be a large and unnecessary surgery. Occasionally, a rod can irritate the soft tissue around the spine, in which case the rod can be removed without affecting the fused spine’s stability.
Two Approaches to Scoliosis Surgery
To perform a spinal fusion for scoliosis, the surgeon usually will approach the spine through the person’s back (posterior) or front (anterior). Specific surgery is recommended based on the type and location of the curve or curves.
1. Posterior Surgical Approach
With the posterior approach, the surgeon will make an incision in the patient’s back that traces over the scoliosis curve(s).
See Posterior Lumbar Interbody Fusion (PLIF) Surgery
Over the past couple decades, the posterior approach has increased in popularity. Previously, the anterior approach was needed for especially rigid curves or to preserve more levels of mobility in the lower spine, but today’s posterior procedures can now accomplish many of the same goals due to enhancements in pedicle screw instrumentation.
Watch: Posterior Lumbar Interbody Fusion (PLIF) Video
By having the ability to place screws in the vertebrae’s centrally-located pedicles—bony segments that connect a vertebral body to its vertebral arch—today’s surgeons can achieve a strong 3-column vertebral fixation to correct rigid curves without also having to approach the spine from the front.
Placing pedicle screws in the lumbar vertebrae have long been possible, but placing them in the smaller thoracic vertebrae (which also are closer to the spinal cord) has only become commonplace in the past decade as more surgeons have gained this expertise.
2. Anterior Surgical Approach
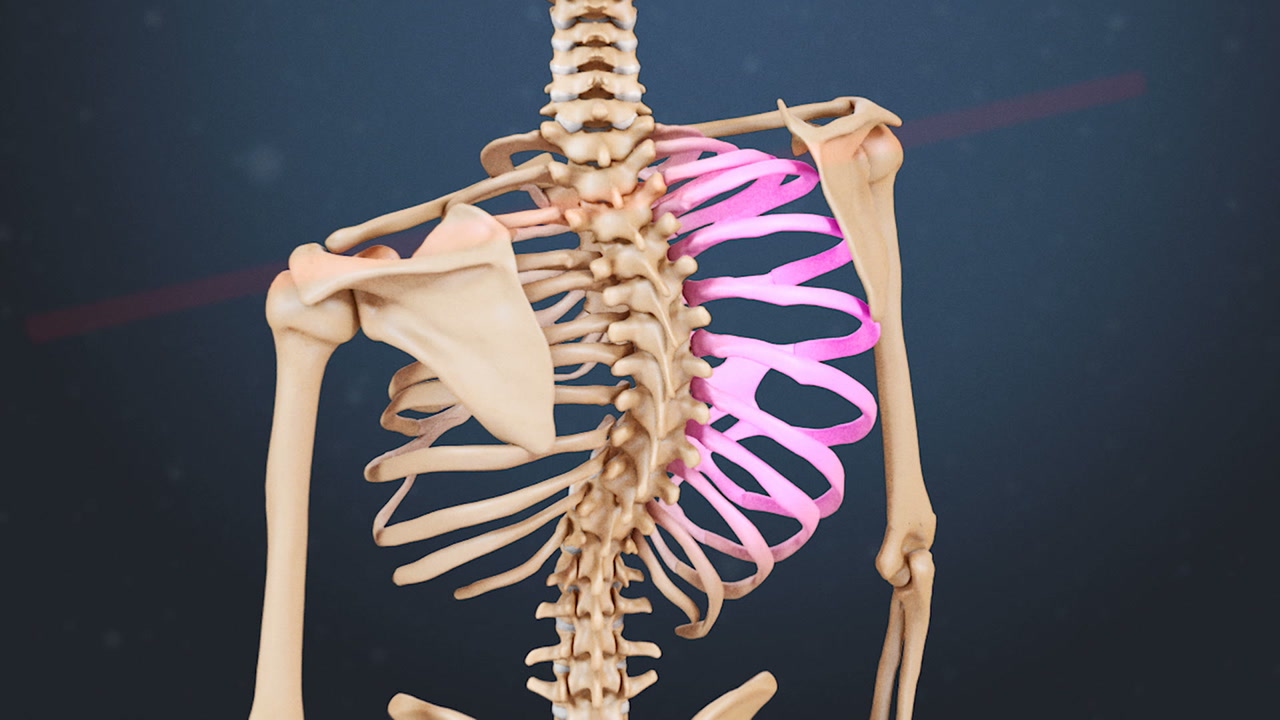
With the anterior approach to scoliosis surgery, the surgeon will go through the patient’s front to access the spine. This approach requires an open incision in the side of the chest and, compared to the posterior approach, has some extra challenges to reach the spine:
- A rib must be removed (usually on the left side)
- The diaphragm is released from the chest wall and spine
- A lung must be deflated to access the spine (and restored afterward)
See Anterior Lumbar Interbody Fusion (ALIF) Surgery
Once the spine is reached, the surgeon will proceed with instrumentation, repositioning the spine, and bone grafting for the fusion.
Watch: ALIF (Anterior Lumbar Interbody Fusion) Video
In the past, a severe deformity or extreme spinal rigidity was commonly treated with a combination of anterior and posterior approaches. However, anterior approach is rarely needed today. With modern instrumentation, most of these procedures can now be done posteriorly without any need for cutting into the chest and deflating a lung.
See Spine Fusion Instrumentation
It should also be noted that a lateral surgical approach, such as XLIF, can be used for short angular thoracolumbar idiopathic scoliosis.