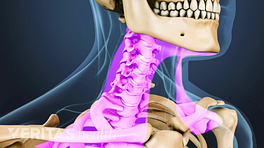
While uncommon, as with all surgery there are a number of risks and potential complications that can occur as a result of a cervical decompression and fusion surgery, including:
- Hemorrhage or formation of a wound hematoma
- Damage to the carotid or vertebral artery resulting in a stroke or excessive bleeding, even death
- Damage to the recurrent laryngeal nerve resulting in hoarseness
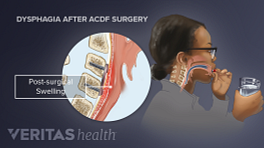
- Damage to the superior laryngeal nerve resulting in swallowing disturbance
- Damage to the esophagus or trachea resulting in infection
- Damage to the dura, resulting in a cerebrospinal fluid leak or pocket of cerebral spinal fluid beneath the incision (pseudomeningocele)
- Mechanical complications of the graft and plate (including graft migration, breakage of the plate, screw pullout, etc.)
- Wound infection
- Development of painful pseudoarthrosis (failure of adequate fusion to occur)
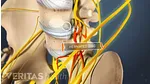
- Damage to the spinal cord or nerve root(s) resulting in pain, weakness, paralysis, loss of sensation, loss of bowel or bladder function, impaired sexual function, etc.
In This Article:
- Anterior Cervical Decompression and Fusion for Cervical Spondylosis with Myelopathy
- Anterior Cervical Decompression and Spine Fusion Procedure
- Potential Risks and Complications of ACDF Surgery
- Anterior Cervical Discectomy and Fusion (ACDF) Video
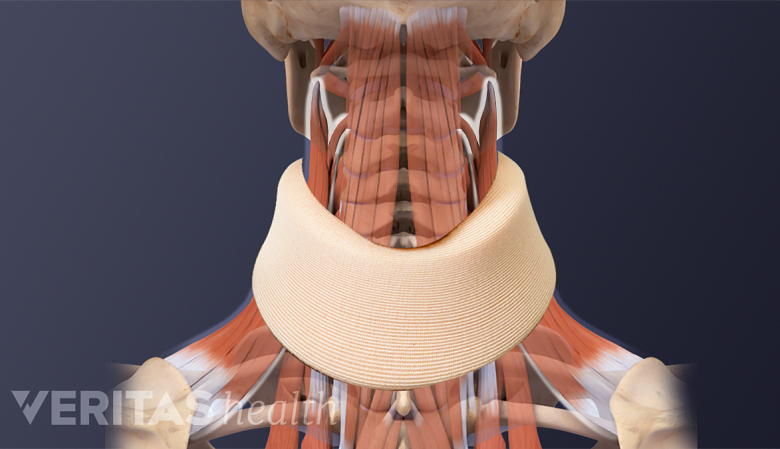
Postoperative Care for Decompression/Fusion Surgery
A neck brace prevents excessive neck movement, aiding in healing and recovery.
Immediately after the surgery, patients will experience some difficulty swallowing or a sore throat due to manipulation of the esophagus. This usually resolves within several days, but symptoms may persist to a troublesome degree.
See ACDF Surgery Postoperative Care
The postoperative pain associated with the procedure is relatively minimal, as most of the exposure is obtained by dissecting tissue, not dividing it. Pain at the graft site (where bone graft is obtained from the hip) is more of a concern if iliac crest graft is utilized (compared to a needle stick to obtain bone marrow aspirate).
See Outpatient Anterior Cervical Discectomy and Fusion (ACDF)
Non-steroidal anti-inflammatory medications (NSAIDs) inhibit bone formation, which is required for the fusion to take hold, and are to be avoided. The same is known for all types of tobacco products. External bone stimulators may be used to theoretically aid fusion formation for selected patients who are at a high risk of poor fusion.
To aid in the postoperative healing process, the spine surgeon may prescribe a cervical collar for a specific period of time to assist in healing and avoid extremes of neck range of motion. The spine surgeon will also provide instructions regarding specific lifting and activity restrictions for the patient in the post-op period.
See 3 Weeks to 3 Months After ACDF Surgery
In most instances, adequate healing (fusion) occurs within a three to six months. The spine surgeon may require sequential x-rays over time to document adequate healing and ensure appropriate alignment at the operative site.
Read more about Potential Risks and Adverse Events Associated with Cervical Spine Surgery