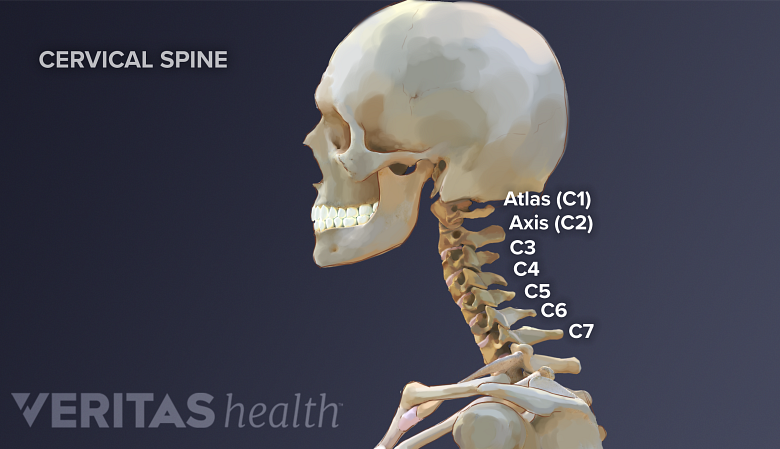
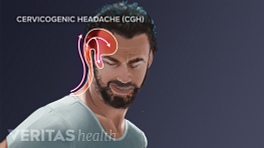
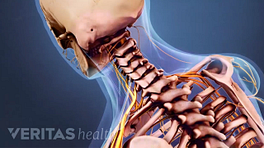
The causes for cervicogenic headache (CGH) are based on the involvement of several anatomical structures in the upper cervical region that are sensitive to pain. The nerves that supply these structures are capable of referring pain from the neck to different parts of the head including the forehead, eye, temple, and ear.
In This Article:
Common Sources of Pain in CGH
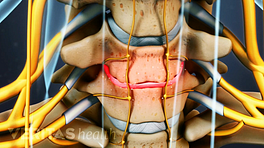
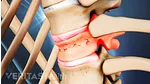
Facet joints of vertebrae C1-C3 are most commonly involved in CGH pain.
One or more of the following anatomical structures in the cervical spine can be primary sources of pain in CGH:
- Facet joints. There are 2 small facet joints at the back of each spinal level, allowing restricted movements between adjacent vertebrae, such as between C2 and C3. The facet joints in the cervical spine are prone to injury due to the weight-bearing function they perform while supporting the head. The upper cervical facet joints relating to vertebrae C1-C3 are most commonly involved in CGH pain, 1 Alix ME, Bates DK. A proposed etiology of cervicogenic headache: the neurophysiologic basis and anatomic relationship between the dura mater and the rectus posterior capitis minor muscle. J Manipulative Physiol Ther. 1999;22(8):534-9. although the facet joints of lower vertebrae may also be involved. At least 70% of CGH cases are reported to occur due to traumatic injuries to the cervical facet joints between vertebrae C2 and C3 2 Bogduk N, Govind J. Cervicogenic headache: an assessment of the evidence on clinical diagnosis, invasive tests, and treatment. Lancet Neurol. 2009; 8:959–968.
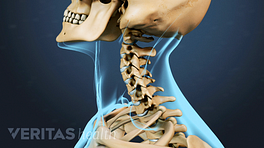
- The atlanto-occipital joint. This joint is where the lower part of the occipital bone (base of the skull) connects with the first cervical vertebra, called the atlas. This region facilitates the passing of the spinal cord out of the skull and down into the cervical spine.
- Intervertebral discs. The cervical intervertebral discs act as shock absorbers between vertebral bones, help facilitate neck movements, and maintain spacing for nerves and joints to function.
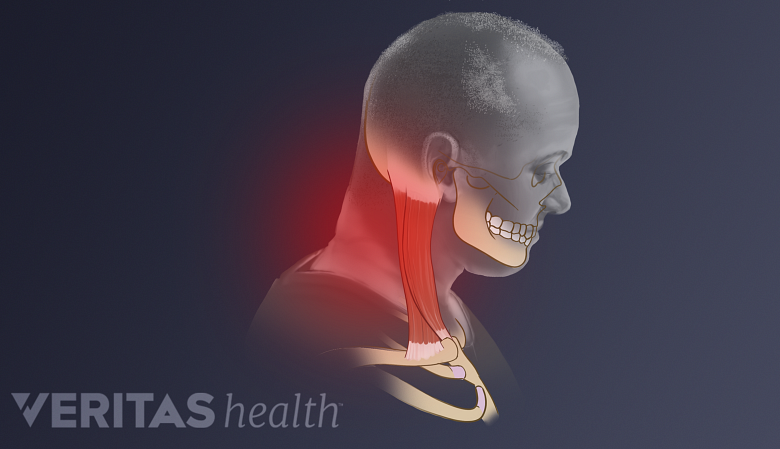
- Neck muscles. Overuse or disuse of certain neck muscles can result in muscle fatigue or weakness leading to CGH. These problems can occur in the muscles of the neck or in the shoulder blade muscles that originate from the neck.
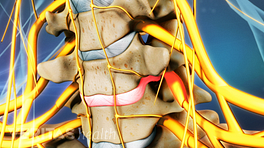
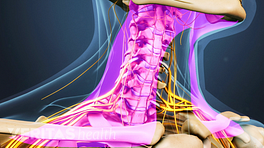
- Cervical nerves. Compression and irritation of cervical spinal nerves can result in CGH. The nerve that innervates the most commonly affected joint (C2-C3) in CGH are medial branches that continue their path to become the third occipital nerve. This nerve continues to course around the back of the head and around the scalp—the path followed by CGH pain.
The anatomical structures within the cervical region are interconnected, so an injury to one is likely to affect the health of others.
Causes of Pain in CGH
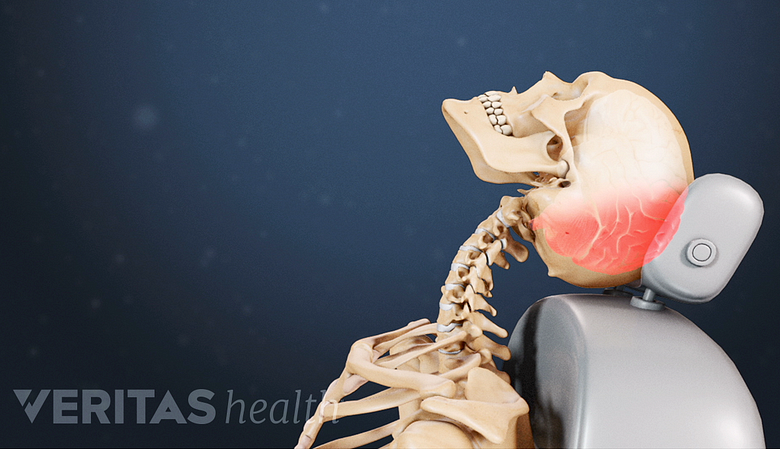
Whiplash injury is the common cause of pain in cervicogenic headaches.
Depending on the structures involved, several causes of CGH can arise in the cervical region. Some of these include:
- Trauma to the facet joints, such as fracture or dislocation due to falling down or playing sports
- Whiplash injury commonly associated with rear-end car accidents
- Rheumatoid arthritis of the facet joints
- Cervical herniated disc, in which the outer layer (annulus fibrosus) tears and the inner jelly-like material (nucleus pulposus) leaks inflammatory proteins
- Normal spinal degeneration due to aging such as cervical degenerative disc disease or osteoarthritis of the facet joints
- Cancer or benign tumors in the cervical region may compress or pinch the cervical spinal nerves causing pain
The most common cause of trauma to the facet joints is whiplash injury, which has been estimated to account for 53% of CGH cases. 2 Bogduk N, Govind J. Cervicogenic headache: an assessment of the evidence on clinical diagnosis, invasive tests, and treatment. Lancet Neurol. 2009; 8:959–968.
Risk Factors for CGH
Forward head tilt over extended periods can strain the muscles of the neck.
Common risk factors associated with CGH are:
- Occupational hazards. Hair stylists, carpenters, drivers, and other occupations may be at a higher risk for CGH due to their head posture while working.
- Strenuous activities. CGH is reported to be the most common type of headache among weight-lifting sportsmen. 3 Page P. Cervicogenic headaches: an evidence-led approach to clinical management. International Journal of Sports Physical Therapy. 2011;6(3):254-266.
- Forward head posture. Holding the head out in a forward position while doing activities such as working on a computer on a continual basis may eventually lead to CGH.
- Female sex. Women are at a higher risk than men to get CGH.
Any posture that puts extra weight on the joints and muscles of the neck can possibly cause CGH over a period of time.
- 1 Alix ME, Bates DK. A proposed etiology of cervicogenic headache: the neurophysiologic basis and anatomic relationship between the dura mater and the rectus posterior capitis minor muscle. J Manipulative Physiol Ther. 1999;22(8):534-9.
- 2 Bogduk N, Govind J. Cervicogenic headache: an assessment of the evidence on clinical diagnosis, invasive tests, and treatment. Lancet Neurol. 2009; 8:959–968.
- 3 Page P. Cervicogenic headaches: an evidence-led approach to clinical management. International Journal of Sports Physical Therapy. 2011;6(3):254-266.