Nerve pain may be incapacitating, and the intricate fibers of the nervous tissue can cause an array of symptoms, including pain, stiffness, weakness, and abnormal sensations (paresthesia).
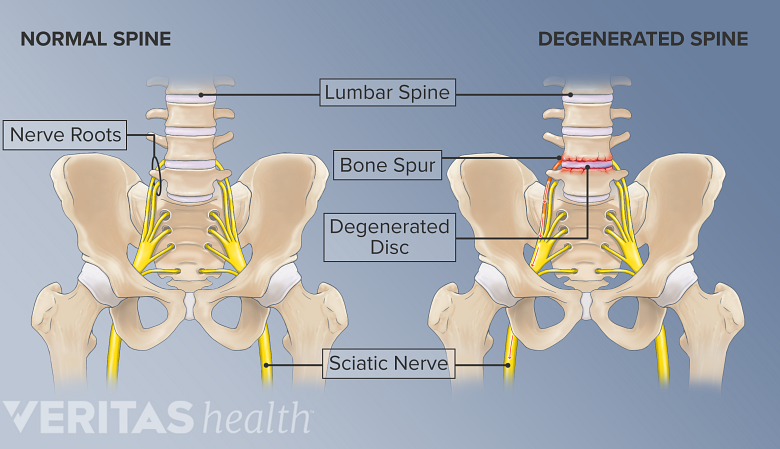
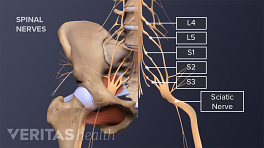
Radiculopathy originating from the sciatic nerve may be felt in clearly outlined (and often overlapping) areas of the thigh and leg, which are responsible for the distinctive symptom patterns associated with sciatica and tend to also help physicians identify the level of the spinal segment(s) that are involved in causing the symptoms. 1 Felten DL, O’Banion MK, Maida MS. Peripheral nervous system. In: Netter’s Atlas of Neuroscience. Elsevier; 2016:153-231.
In This Article:
- Understanding Sciatica Symptoms: Pins and Needles, Numbness, Icy, and Burning
- The Essentials of Sciatic Nerve Pain Patterns
- Challenges in Diagnosing the Cause of Sciatica
- Sciatica Causes and Symptoms Video
Recognizing the 2 Main Symptom-Causing Components of the Sciatic Nerve
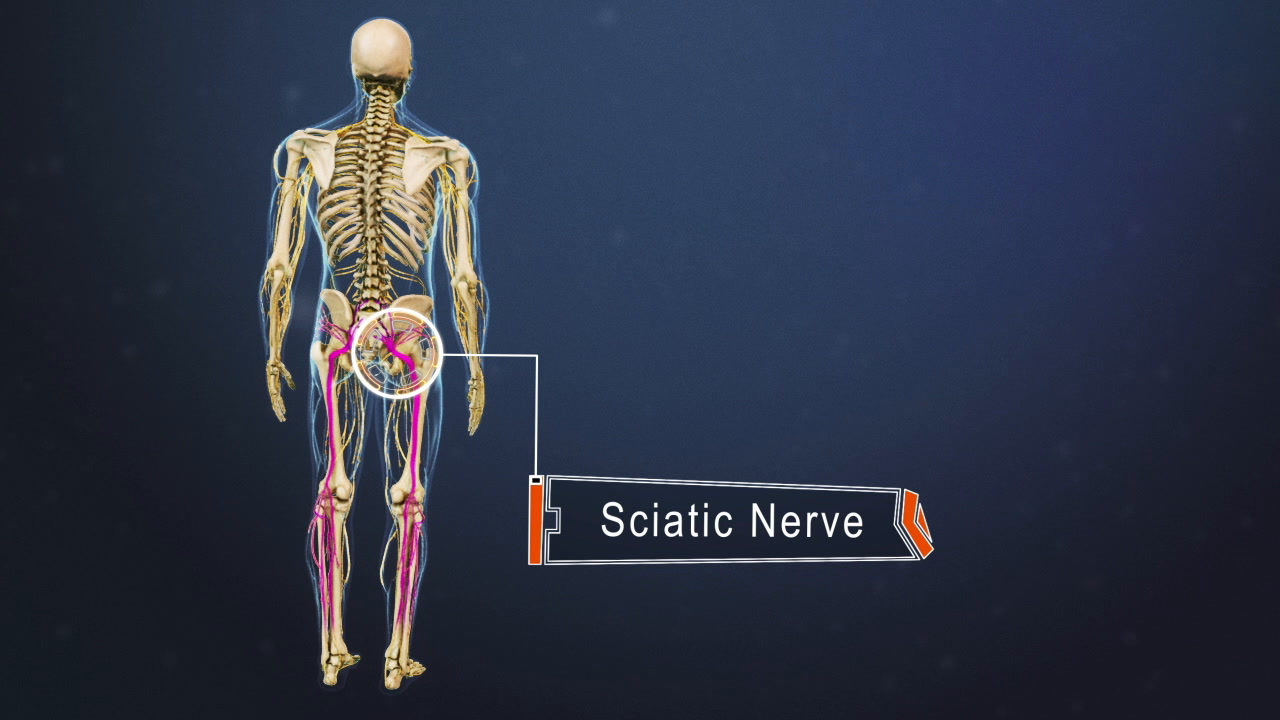
The structure and composition of the sciatic nerve is made of smaller elements that help conduct sensory and motor impulses to the lower part of the body below the hip. An impairment to these delicate neural tissues can result in varying degrees of symptoms and signs.
1. Sciatic nerve roots
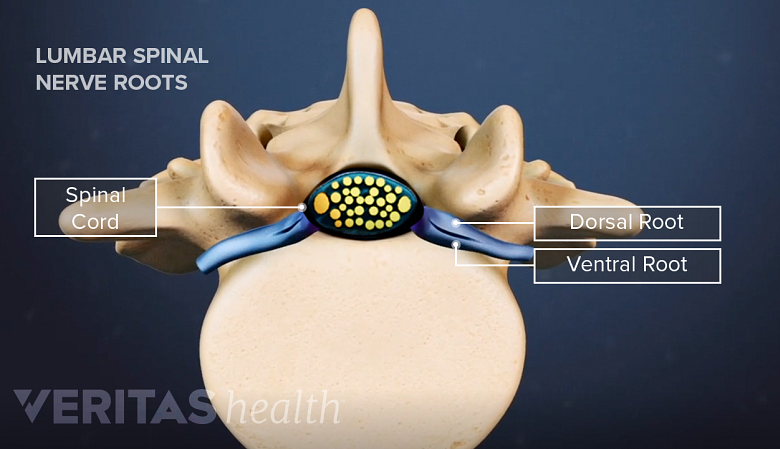
The dorsal and ventral roots branch off from the spinal cord and merge together to form a single spinal nerve.
At the level of each spinal segment, two individual “roots” (bundles of nerve fibers) branch off the spinal cord and merge right before it enters the intervertebral foramen as a single nerve root. These individual roots are:
- Dorsal root: A small group of nerve fibers derived from the back (posterior end) of the spinal cord.
- Ventral root: A comparatively larger group of nerve fibers derived from the front (anterior end) of the spinal cord.
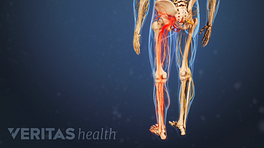
The dorsal and ventral roots of the sciatic nerve are responsible for symptoms along the buttocks, thigh, leg, and foot.
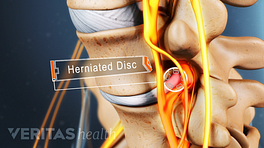
The nerve root lies within and courses through the intervertebral foramen at each vertebral segment. The nerve root is short, at times measuring just 1 mm in length 2 Bogduk N. Clinical and Radiological Anatomy of the Lumbar Spine E-Book. Elsevier Health Sciences; 2012. as it lies within this foramen. If this tiny segment of nerve root is affected while it courses through the foramen in the lower spine, sciatica may occur.
Watch Sciatic Nerve Anatomy Video
While the cause(s) of sciatica is mostly defined as a problem occurring at the level of the spinal nerve root, it is also possible for the dorsal or ventral roots to be affected before they merge to form the spinal nerve root. Research indicates that the dorsal roots are more vulnerable to inflammation, irritation, or compression compared to the ventral roots. 3 Dydyk AM, M Das J. Radicular Back Pain. [Updated 2020 Apr 14]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK546593/
2. Sciatic nerve fibers
The sciatic nerve roots are composed of two types of specialized nerve fibers derived from the dorsal and ventral roots:
- Sensory fibers—help conduct impulses, resulting in sensations that cannot be seen, but felt (such as touch and pain).
- Motor fibers—help execute actions that can be seen or performed (such as walking, lifting the leg, and sitting).
The sensory and motor fibers within the sciatic nerve roots are distinct and can be affected individually or together, resulting in only pain, only motor deficits, or both. 3 Dydyk AM, M Das J. Radicular Back Pain. [Updated 2020 Apr 14]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK546593/
Dermatomes and Sclerotomes in Sciatica-Related Sensory Impairment
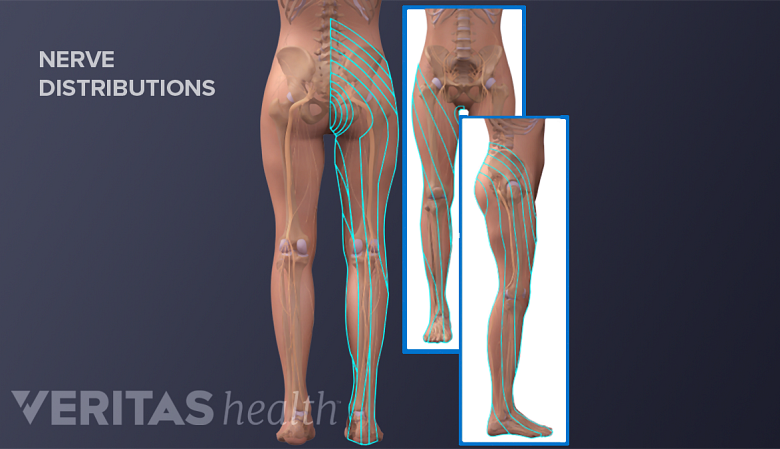
Each spinal nerve root supplies a unique area of skin in the lower back, leg, and foot.
Depending on the type of nerve fibers that are affected, a constellation of sensory sciatica symptoms may be felt in different areas of skin, called dermatomes. 4 Postacchini F. Lumbar Disc Herniation. Springer Science & Business Media; 1998. Sensory symptoms are more common in sciatica.
When the sensory component of a sciatic nerve root is affected, radicular pain and sensory deficits may be experienced in the related dermatome.
The dermatomes of the sciatic nerve roots typically have the following characteristics:
- They are shaped like long, vertical, and continuous bands extending from the lower back into the leg and foot 5 Davis D, Maini K, Vasudevan A. Sciatica. [Updated 2020 Apr 27]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK507908/
- They may overlap each other 4 Postacchini F. Lumbar Disc Herniation. Springer Science & Business Media; 1998.
- The nerve supply to a specific dermatome may vary among individuals, resulting in different dermatomal patterns
- They may be related to other areas called sclerotomes, which can cause more painful symptoms due to referred pain from the spinal nerve root. 6 Laroche F, Perrot S. Managing Sciatica and Radicular Pain in Primary Care Practice. Springer Science & Business Media; 2013. Sclerotomes are defined as pain emanating areas of bone or fascia supplied by a single nerve root. Nerve distribution varies greatly among individuals 7 Cole AJ, Herring SA, eds. The Low Back Pain Handbook: A Guide for the Practicing Clinician. 2nd ed. Hanley & Belfus; 2003.
The L5 nerve root, for example, has such sclerotomes in the buttock and on either side of the ankle—causing pain in these regions in addition to the typical sciatica symptoms caused by this nerve root. Sclerotomes are deep sensory areas and also include bone, ligaments, tendons, and joint capsules that are supplied by the nerve root. The sclerotomes are less distinct and less understood than dermatomes but are a considerable source of pain and sensory symptoms in sciatica. Sclerotomal pain is usually a deep and dull ache, while dermatomal pain is sharp and shock-like. 6 Laroche F, Perrot S. Managing Sciatica and Radicular Pain in Primary Care Practice. Springer Science & Business Media; 2013.
The sensory component of a nerve root is responsible for tingling, pins and needles, numbness, pain, and paresthesia. Excruciating spasms of the leg muscles may also occur in some individuals when the motor fibers (described in the next section) are affected. 6 Laroche F, Perrot S. Managing Sciatica and Radicular Pain in Primary Care Practice. Springer Science & Business Media; 2013. These symptoms may be experienced in the entire dermatomal band, just one part of the dermatomal area, and/or the sclerotome supplied by the nerve.
How Leg Weakness and Decreased Function Occur in Sciatica
When the motor component of a sciatic nerve root is affected, a variable degree of weakness and loss of movement may be experienced in the muscle group(s), called a myotome.
The role of myotomes in sciatica-related motor impairment
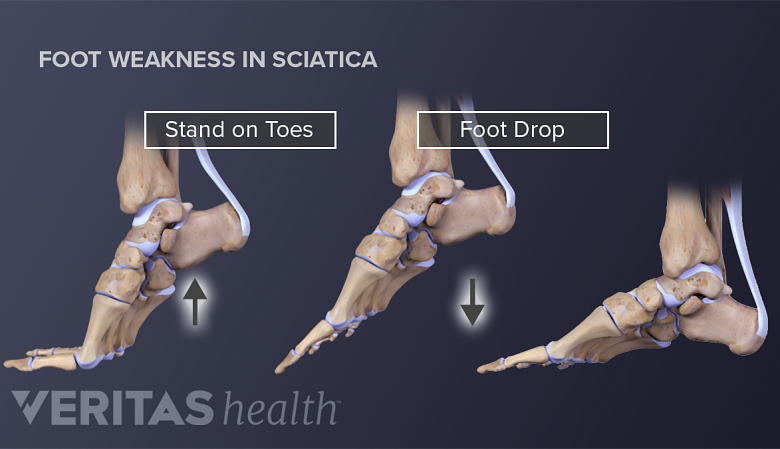
When the motor fibers of a sciatic nerve root are affected, foot drop may occur.
Multiple nerves supply the myotomes in the leg. 3 Dydyk AM, M Das J. Radicular Back Pain. [Updated 2020 Apr 14]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK546593/ When a spinal nerve root is directly compressed by a mechanical force, such as from a severely herniated disc, it may involve several motor fibers. 5 Davis D, Maini K, Vasudevan A. Sciatica. [Updated 2020 Apr 27]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK507908/
When the sciatic myotomes are affected, there is a loss of strength in the affected muscles, resulting in one or more of the following signs 6 Laroche F, Perrot S. Managing Sciatica and Radicular Pain in Primary Care Practice. Springer Science & Business Media; 2013. :
- Difficulty or inability to arise from a chair, indicating iliopsoas or quadriceps muscle weakness in the top and front of the thigh
- Buckling of the knee, indicating quadriceps muscle weakness in the front of the thigh
- Dragging of the toe or foot drop, indicating tibialis anterior muscle weakness in the front of the leg
While uncommon, it is possible to have motor impairment and symptoms of sciatica without any sensory issues.
Subsequent Loss of Stability, Mobility, and Function in the Lower Back and Leg
Over time, spinal degeneration causes instability and loss of function in the lower back and leg.
Without appropriate treatment and care, certain underlying causes of sciatica can cause a cascade of neurological and musculoskeletal events, resulting in troubling symptoms and signs in the lower body, leading to weakness and loss of function in the lower back and leg(s). These spinal changes may include:
- Decrease in vertebral stability, leading to abnormal posture 8 Studnicka K, Ampat G. Lumbar Stabilization. [Updated 2021 Nov 29]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK562179/ , 9 Henson B, Kadiyala B, Edens MA. Anatomy, Back, Muscles. [Updated 2021 Aug 10]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK537074/
- Reduction in joint range of motion in the hip and knee, interrupting the biomechanics in the spine and pelvis 10 Bueno-Gracia E, Pérez-Bellmunt A, Estébanez-de-Miguel E, et al. Differential movement of the sciatic nerve and hamstrings during the straight leg raise with ankle dorsiflexion: Implications for diagnosis of neural aspect to hamstring disorders. Musculoskeletal Science and Practice. 2019;43:91-95. , 11 Jandre Reis FJ, Macedo AR. Influence of Hamstring Tightness in Pelvic, Lumbar and Trunk Range of Motion in Low Back Pain and Asymptomatic Volunteers during Forward Bending. Asian Spine J. 2015;9(4):535-540. doi:10.4184/asj.2015.9.4.535
- Increase in spinal degeneration, leading to further deterioration of the affected spinal segment 12 Makino H, Kawaguchi Y, Seki S, Nakano M, Yasuda T, Suzuki K, Ikegawa S, Kimura T. Lumbar disc degeneration progression in young women in their 20's: A prospective ten-year follow up. J Orthop Sci. 2017 Jul;22(4):635-640. doi: 10.1016/j.jos.2017.03.015
- Weakening of muscles in the hip and knee joints, causing reduced mobility in the lower back and leg 11 Jandre Reis FJ, Macedo AR. Influence of Hamstring Tightness in Pelvic, Lumbar and Trunk Range of Motion in Low Back Pain and Asymptomatic Volunteers during Forward Bending. Asian Spine J. 2015;9(4):535-540. doi:10.4184/asj.2015.9.4.535
- Decrease in blood circulation to the spinal muscles, leading to poor healing and restoration of spinal tissues 13 Lee JH, Kim TH. The treatment effect of hamstring stretching and nerve mobilization for patients with radicular lower back pain. J Phys Ther Sci. 2017;29(9):1578-1582. doi:10.1589/jpts.29.1578
- Inflammation of nerves, causing neural tension and stiffness 13 Lee JH, Kim TH. The treatment effect of hamstring stretching and nerve mobilization for patients with radicular lower back pain. J Phys Ther Sci. 2017;29(9):1578-1582. doi:10.1589/jpts.29.1578
- Biochemical changes in the small blood vessels that supply the affected regions (microvascular changes), causing pain 13 Lee JH, Kim TH. The treatment effect of hamstring stretching and nerve mobilization for patients with radicular lower back pain. J Phys Ther Sci. 2017;29(9):1578-1582. doi:10.1589/jpts.29.1578
Over time, muscle weakness may progress or become chronic. When muscles are fatigued for long periods of time, muscular shortening and eventually decrease in muscle mass or atrophy may occur, resulting in joint pain and stiffness. 14 Hildebrandt M, Fankhauser G, Meichtry A, Luomajoki H. Correlation between lumbar dysfunction and fat infiltration in lumbar multifidus muscles in patients with low back pain. BMC Musculoskelet Disord. 2017;18(1):12. Published 2017 Jan 10. doi:10.1186/s12891-016-1376-1
Sciatica or symptoms that mimic sciatica must be evaluated by a medical professional trained in musculoskeletal disorders of the spine, such as a Physical Medicine and Rehabilitation specialist (physiatrist), orthopedic surgeon, neurologist, or neurosurgeon. An accurate diagnosis and prompt treatment can prevent the underlying condition from becoming worse or chronic. Sciatica typically resolves within 4 to 6 weeks, 5 Davis D, Maini K, Vasudevan A. Sciatica. [Updated 2020 Apr 27]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK507908/ but in some cases, depending on the cause, the symptoms may become chronic and last up to 12 months. 15 Fernandez M, Hartvigsen J, Ferreira ML, et al. Advice to Stay Active or Structured Exercise in the Management of Sciatica. Spine. 2015;40(18):1457-1466. doi:10.1097/brs.0000000000001036
See Specialists Who Treat Back Pain
Intractable pain and/or weakness in the lower back and legs with other troubling symptoms, such as loss or bowel and/or bladder control and/or loss of sensation in the inner thigh/groin area may indicate a more serious underlying problem, such as cauda equina syndrome.
These medical emergencies must be treated on an urgent basis to preserve leg function and prevent irreversible damage to the nerves.
- 1 Felten DL, O’Banion MK, Maida MS. Peripheral nervous system. In: Netter’s Atlas of Neuroscience. Elsevier; 2016:153-231.
- 2 Bogduk N. Clinical and Radiological Anatomy of the Lumbar Spine E-Book. Elsevier Health Sciences; 2012.
- 3 Dydyk AM, M Das J. Radicular Back Pain. [Updated 2020 Apr 14]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK546593/
- 4 Postacchini F. Lumbar Disc Herniation. Springer Science & Business Media; 1998.
- 5 Davis D, Maini K, Vasudevan A. Sciatica. [Updated 2020 Apr 27]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK507908/
- 6 Laroche F, Perrot S. Managing Sciatica and Radicular Pain in Primary Care Practice. Springer Science & Business Media; 2013.
- 7 Cole AJ, Herring SA, eds. The Low Back Pain Handbook: A Guide for the Practicing Clinician. 2nd ed. Hanley & Belfus; 2003.
- 8 Studnicka K, Ampat G. Lumbar Stabilization. [Updated 2021 Nov 29]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK562179/
- 9 Henson B, Kadiyala B, Edens MA. Anatomy, Back, Muscles. [Updated 2021 Aug 10]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK537074/
- 10 Bueno-Gracia E, Pérez-Bellmunt A, Estébanez-de-Miguel E, et al. Differential movement of the sciatic nerve and hamstrings during the straight leg raise with ankle dorsiflexion: Implications for diagnosis of neural aspect to hamstring disorders. Musculoskeletal Science and Practice. 2019;43:91-95.
- 11 Jandre Reis FJ, Macedo AR. Influence of Hamstring Tightness in Pelvic, Lumbar and Trunk Range of Motion in Low Back Pain and Asymptomatic Volunteers during Forward Bending. Asian Spine J. 2015;9(4):535-540. doi:10.4184/asj.2015.9.4.535
- 12 Makino H, Kawaguchi Y, Seki S, Nakano M, Yasuda T, Suzuki K, Ikegawa S, Kimura T. Lumbar disc degeneration progression in young women in their 20's: A prospective ten-year follow up. J Orthop Sci. 2017 Jul;22(4):635-640. doi: 10.1016/j.jos.2017.03.015
- 13 Lee JH, Kim TH. The treatment effect of hamstring stretching and nerve mobilization for patients with radicular lower back pain. J Phys Ther Sci. 2017;29(9):1578-1582. doi:10.1589/jpts.29.1578
- 14 Hildebrandt M, Fankhauser G, Meichtry A, Luomajoki H. Correlation between lumbar dysfunction and fat infiltration in lumbar multifidus muscles in patients with low back pain. BMC Musculoskelet Disord. 2017;18(1):12. Published 2017 Jan 10. doi:10.1186/s12891-016-1376-1
- 15 Fernandez M, Hartvigsen J, Ferreira ML, et al. Advice to Stay Active or Structured Exercise in the Management of Sciatica. Spine. 2015;40(18):1457-1466. doi:10.1097/brs.0000000000001036