Cervical degenerative disc disease is a common cause of neck pain and radiating arm pain. It develops when one or more of the cushioning discs in the cervical spine starts to break down due to wear and tear.
There may be a genetic component that predisposes some people to more rapid wear. Injury may also accelerate and sometimes cause the development of the degenerative changes.
In This Article:
How Cervical Discs Can Degenerate
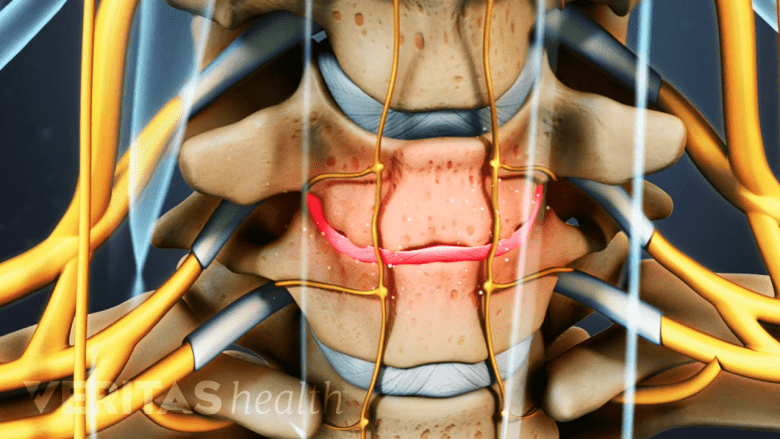
As the disc loses hydration, it becomes prone to cracking and tearing.
Normally, there are six gel-like cervical discs (one between each of the cervical spine’s vertebrae) that absorb shock and prevent vertebral bones from rubbing against each other while the neck moves.
Each disc is comprised of a tough but flexible outer layer of woven cartilage strands, called the annulus fibrosus. Sealed inside the annulus fibrosus is a soft interior filled with a mucoprotein gel called the nucleus pulposus. The nucleus gives the disc its shock absorption property.
Watch Cervical Disc Anatomy Animation
In children, the discs are about 85% water. The discs begin to naturally lose hydration during the aging process. Some estimates have the disc’s water content typically falling to 70% by age 70,1Czervionke L. Degenerative disc disease. In: Czervionke L, Fenton D. Imaging Painful Spinal Disorders, 1st ed. Philadelphia, PA: Elsevier Saunders; 2011; Chapter 17. but in some people the disc can lose hydration much more quickly.
As the disc loses hydration, it offers less cushioning and becomes more prone to cracks and tears. The disc is not able to truly repair itself because it does not have a direct blood supply (instead getting nutrients and metabolites via diffusion with adjacent vertebrae through the cartilaginous endplates). As such, a tear in the disc either will not heal or will develop weaker scar tissue that has potential to break again.
The Course of Cervical Degenerative Disc Disease
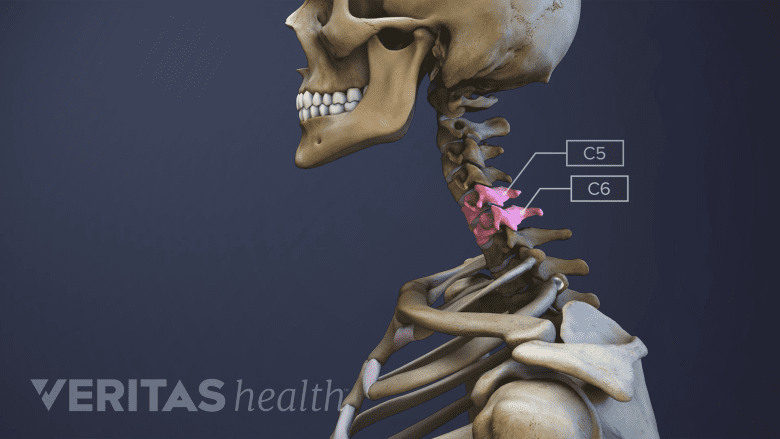
Cervical disc degeneration is commonly seen in the C5-C6 motion segment.
Cervical degenerative disc disease is not technically a disease, but rather a description of the degenerative process that discs located in the cervical spine go through. Essentially all people who live long enough will develop degenerated discs.
Studies show that a plurality of adults have no symptoms related to degenerative disc disease, even though a high percentage of these adults still shows signs of disc degeneration on an MRI somewhere on the spine. One study found that about half of people start showing some signs of disc degeneration on an MRI by their early 20s.2De Bruin F, ter Horst S, van den Berg R, et al. Signal intensity loss of the intervertebral disc in the cervical spine of young patients on fluid sensitive. Skeletal Radiol. 2016; 45: 375-381. Another study found that about 75% of people under age 50 have disc degeneration while more than 90% of people over age 50 have it.3Teraguchi M, Yoshimura N, Hashizume H, et al. Prevalence and distribution of intervertebral disc degeneration over the entire spine in a population-based cohort: the Wakayama Spine Study. Osteoarthr Cartil. 2014;22(1):104-10.
When degenerative disc disease develops in the cervical spine, it can occur in any of the cervical discs but is slightly more likely to occur at the C5-C6 level.3Teraguchi M, Yoshimura N, Hashizume H, et al. Prevalence and distribution of intervertebral disc degeneration over the entire spine in a population-based cohort: the Wakayama Spine Study. Osteoarthr Cartil. 2014;22(1):104-10.
Watch Spinal Motion Segment: C5-C6 Video
In cases where cervical degenerative disc disease does cause pain, it can happen in various ways. In some instances, the disc itself can become painful. People are more likely to experience this type of discogenic pain in their 30s, 40s, or 50s.
When symptoms from cervical degenerative disc disease become chronic, the pain and/or symptoms are likely related to conditions associated with disc degeneration, such as a herniated disc, osteoarthritis, or spinal stenosis. Depending on the cause, the pain may be temporary, or may become chronic. To give an example, pain from a herniated disc is likely to eventually go away on its own, but pain from osteoarthritis may require treatment on a chronic basis.
Risk Factors for Cervical Degenerative Disc Disease
While nearly everyone eventually gets cervical degenerative disc disease with age, there are some factors that can make it more likely to develop sooner and/or become symptomatic. These risk factors could include:
- Genetics. Some studies of twins indicate genetics play a bigger role than lifestyle in determining when cervical degenerative disc disease develops and if it becomes painful.
- Obesity. Weight has been linked to risk for developing degenerative disc disease.
Smoking. This habit can hinder nutrients from reaching the discs and cause them to lose hydration more quickly.
In addition, an injury to the spine, such as a herniated disc in the neck, can sometimes start or accelerate cervical degenerative disc disease.
- 1 Czervionke L. Degenerative disc disease. In: Czervionke L, Fenton D. Imaging Painful Spinal Disorders, 1st ed. Philadelphia, PA: Elsevier Saunders; 2011; Chapter 17.
- 2 De Bruin F, ter Horst S, van den Berg R, et al. Signal intensity loss of the intervertebral disc in the cervical spine of young patients on fluid sensitive. Skeletal Radiol. 2016; 45: 375-381.
- 3 Teraguchi M, Yoshimura N, Hashizume H, et al. Prevalence and distribution of intervertebral disc degeneration over the entire spine in a population-based cohort: the Wakayama Spine Study. Osteoarthr Cartil. 2014;22(1):104-10.