Osteoporosis on its own does not cause pain or obvious symptoms. Complications arise when loss of bone strength makes the spine less able to withstand everyday stresses, such as from a minor fall or even lifting a bag of groceries from the trunk of a car.
In This Article:
Compression Fractures from Osteoporosis
Weak vertebral bodies collapse due to repetitive spine pressure, resulting in a compression fracture.
Regular minor stresses can cause small fractures to develop throughout the spine. A fracture may be the first outward sign of osteoporosis.
The wide, flat portion of the vertebra (called the vertebral body) is the part of the spine most susceptible to fracture from low bone strength. When vertebral bodies are too weak to support the daily pressure placed on the spine (such as when walking), it may collapse, called a compression fracture. Advanced osteoporosis can lead to multiple compression fractures throughout the spine.
Common Complications of Osteoporosis
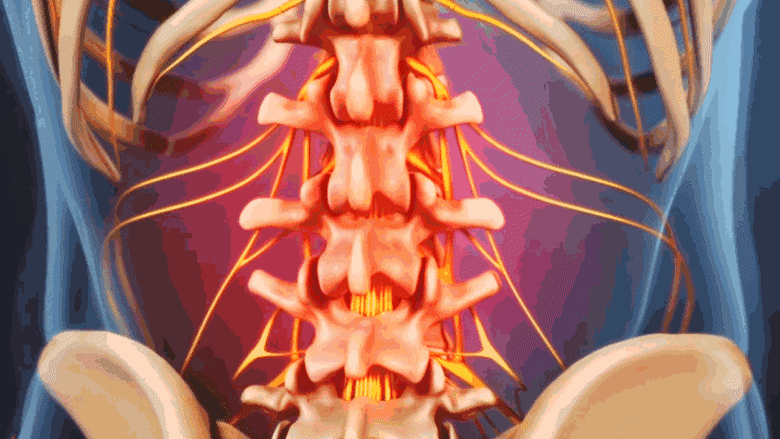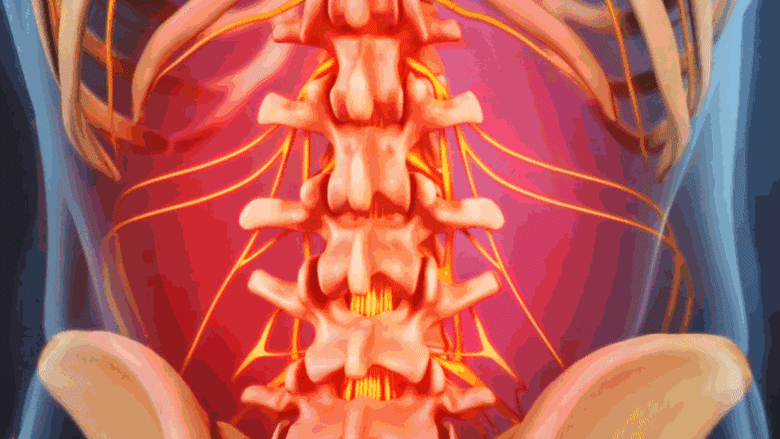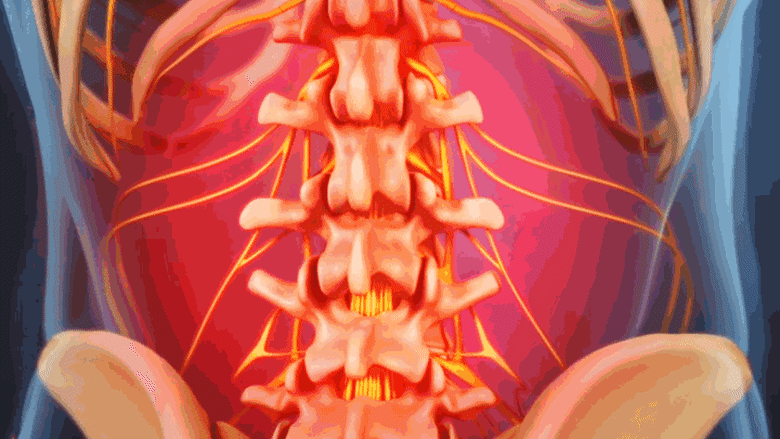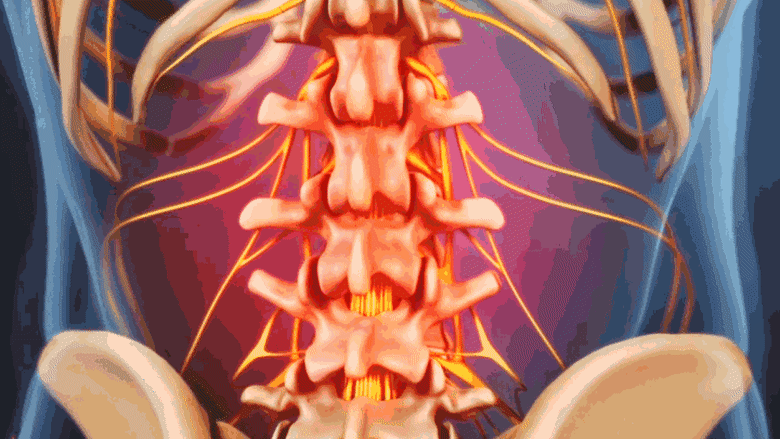
Spinal fractures from osteoporosis cause focal pain at the site of the fracture.
Spinal fractures from osteoporosis can lead to a range of complications, such as:
- Back pain at the level of the fracture. Back pain may start gradually or suddenly, and may be severe. Nerve root pain from osteoporosis is less common.1Cannada LK, Hill BW. Osteoporotic Hip and Spine Fractures: A Current Review. Geriatr Orthop Surg Rehabil. 2014;5(4):207–212. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4252159/. Published Sept 5, 2014. Accessed April 2019.
- A hunch in the upper back where vertebrae have fractured and partially collapsed in several places, causing the curve of the spine to change.
- Loss of height due to multiple fractures in the vertebral bodies.
- Loss of mobility and instability during daily activity due to weakening of the bones.
- Respiratory and cardiovascular complications when multiple fractures shorten the torso and compress the abdomen
- Loss of self-esteem, loss of independence, mood changes
- Rarely, neurologic injury
See Vertebral Fracture Symptoms
Many fractures occur with no symptoms, or symptoms may not be felt immediately.
Symptoms of a compression fracture may develop suddenly. For example, person may fall and experience a sudden onset of back pain that gets worse while sitting or standing (placing weight on the spine). Pain from a fracture tends to feel better when lying down (taking weight off the spine).
When Is Spinal Osteoporosis Serious?
In its early stages, osteoporosis does not cause complications with any obvious symptoms such as back pain or instability. If osteoporosis is diagnosed at this stage, through routine screening and diagnostic studies, it is typically not severe and can be managed effectively to delay or avoid fractures.
See Diagnostic Processes for Neck and Back Pain
In some cases, osteoporosis may only be diagnosed once a fracture has occurred. If a person has been diagnosed with osteoporosis and has one or more fractures in the spine or hip, it may be considered severe. Severe spinal osteoporosis can cause significant back or neck pain and disability.
- 1 Cannada LK, Hill BW. Osteoporotic Hip and Spine Fractures: A Current Review. Geriatr Orthop Surg Rehabil. 2014;5(4):207–212. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4252159/. Published Sept 5, 2014. Accessed April 2019.

