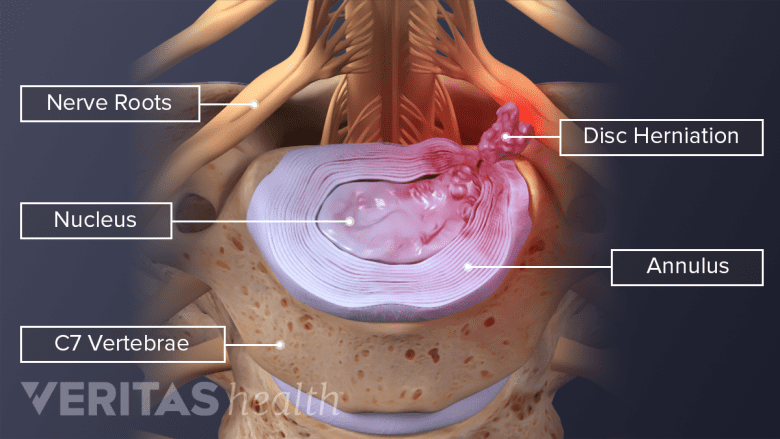
Cervical spinal stenosis occurs when one or more intervertebral foramina (bony openings where the spinal nerves exit the spinal canal) become narrowed within the neck. When too much narrowing leads to spinal nerve compression and/or inflammation, symptoms of pain, tingling, numbness, and/or weakness may radiate from the neck into the arm.
In This Article:
Range of Cervical Foraminal Stenosis Symptoms
Cervical foraminal stenosis causes electric-like sharp pain radiating into arm and hand.
Cervical foraminal stenosis symptoms can vary in intensity from a mild annoyance to severe or debilitating. Symptoms may include one or more of the following:
- Neck pain that can feel dull or sharp and may be accompanied by swelling or stiffness
- Cervical radicular pain that is electric-like and radiates into the arm or hand
- Cervical radiculopathy, which includes neurological deficits such as numbness, reflex problems, and/or weakness in the shoulder, arm, hand, or fingers.
Cervical spinal stenosis does not always cause symptoms. It is possible to have cervical foraminal narrowing that is visible on medical imaging, such as an MRI, without any associated pain or neurological deficits. The underlying factors as to why some people with cervical foraminal stenosis have symptoms and others do not is still being researched.
How Cervical Foraminal Stenosis Causes Symptoms
Cervical foraminal stenosis can cause pain and neurological symptoms by one or more of the following mechanisms.
Direct spinal nerve root compression
Cervical foraminal stenosis causes pain and nerve issues from bone spurs pressing on spinal nerve roots.
Degenerative causes, such as bone spurs (osteophytes) in the neck, cervical degenerative disc disease, and/or thickened ligaments may directly compress the spinal nerve root. The uncovertebral joint (on either side of the vertebra) is a common location for bone spurs to grow and encroach upon the nerve root. Additionally, as the disc loses hydration and flattens out over the time, the decreased disc space can contribute to nerve root compression.
Spinal nerve root inflammation
A cervical herniated disc induces nerve root inflammation, resulting in pain.
Biochemical processes may also contribute to nerve root inflammation and damage.1Slipman CW, Isaac Z, Lenrow, DA, Chou L. Clinical evidence of chemical radiculopathy. Pain Physician. 2002. 5(3):260-5. For example, a disc herniation can leak inflammatory chemicals onto the spinal nerve in the foramen.2Iyer S, Kim HJ. Cervical radiculopathy. Curr Rev Musculoskelet Med. 2016; 9(3):272-80. doi: 10.1007/s12178-016-9349-4.
See Cervical Herniated Disc Symptoms and Treatment Options
Some individuals may have a genetic predisposition to these degenerative changes that can lead to cervical spinal stenosis and pain.
The Course of Cervical Foraminal Stenosis
Narrowing of the intervertebral foramina in the cervical spine typically develops as apart of the aging process in people over age 50.3Spinal Stenosis: Who Gets It? National Institute of Arthritis and Musculoskeletal and Skin Diseases, National Institutes of Health Website. https://www.niams.nih.gov/health-topics/spinal-stenosis. Accessed October 8, 2019.,4Childress MA, Becker BA. Nonoperative management of cervical radiculopathy. Am Fam Physician. 2016; 93(9):746-54. Cervical foraminal stenosis can also occur sooner due to injury or congenital factors (from birth).
While cervical foraminal stenosis tends to progress over time, the symptoms may not necessarily worsen. Most people can manage cervical foraminal stenosis symptoms with nonsurgical treatments, such as physical therapy, medication, rest, cervical traction, and minimally invasive injection therapies.
When weakness, numbness, and/or severe pain continue to worsen despite nonsurgical treatments, surgery may be considered. Surgery is typically recommended for cervical foraminal stenosis when imaging and other diagnostic tests show that symptoms are likely to be relieved by decompressing the nerve root.
When Cervical Foraminal Stenosis Is Serious
Neck pain with arm numbness and weakness requires immediate medical attention.
When a cervical spinal nerve is compressed or inflamed, neurological deficits, such as numbness or weakness may develop in the shoulder, arm, and/or hand. If this nerve compression and the associated neurological deficits go untreated, permanent numbness and/or paralysis can occur.
Any neck pain that is accompanied by arm numbness, weakness, and/or changes in balance, urinary function or coordination needs to be examined by a doctor.
- 1 Slipman CW, Isaac Z, Lenrow, DA, Chou L. Clinical evidence of chemical radiculopathy. Pain Physician. 2002. 5(3):260-5.
- 2 Iyer S, Kim HJ. Cervical radiculopathy. Curr Rev Musculoskelet Med. 2016; 9(3):272-80. doi: 10.1007/s12178-016-9349-4.
- 3 Spinal Stenosis: Who Gets It? National Institute of Arthritis and Musculoskeletal and Skin Diseases, National Institutes of Health Website. https://www.niams.nih.gov/health-topics/spinal-stenosis. Accessed October 8, 2019.
- 4 Childress MA, Becker BA. Nonoperative management of cervical radiculopathy. Am Fam Physician. 2016; 93(9):746-54.