Sleeping is the only time your spinal muscles, ligaments, discs, and joints get to completely relax and rejuvenate.
A good choice of mattress will go a long way in supporting this type of deep, healing sleep.
When choosing a mattress, it is advisable to select one that is not too firm or overly soft, provides customized support for your spine, and suits your personal preferences for comfort.
Specifically, there is medical research to indicate that a medium-firm mattress works well for most people, whether they have back pain or not.1Caggiari G, Talesa GR, Toro G, Jannelli E, Monteleone G, Puddu L. What type of mattress should be chosen to avoid back pain and improve sleep quality? Review of the literature. J Orthop Traumatol. 2021;22(1):51. Published 2021 Dec 8. doi:10.1186/s10195-021-00616-5
This article also reviews findings in the medical literature on the impact of a mattress that provides customized support for spinal alignment, as well as personalized comfort.2Radwan A, Fess P, James D, et al. Effect of different mattress designs on promoting sleep quality, pain reduction, and spinal alignment in adults with or without back pain; systematic review of controlled trials. Sleep Health. 2015;1(4):257-267. doi:10.1016/j.sleh.2015.08.001,3Normand MC, Descarreaux M, Poulin C, et al. Biomechanical effects of a lumbar support in a mattress. J Can Chiropr Assoc. 2005;49(2):96-101. Available from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1840018/
Guideline #1: A medium-firm mattress is generally recommended
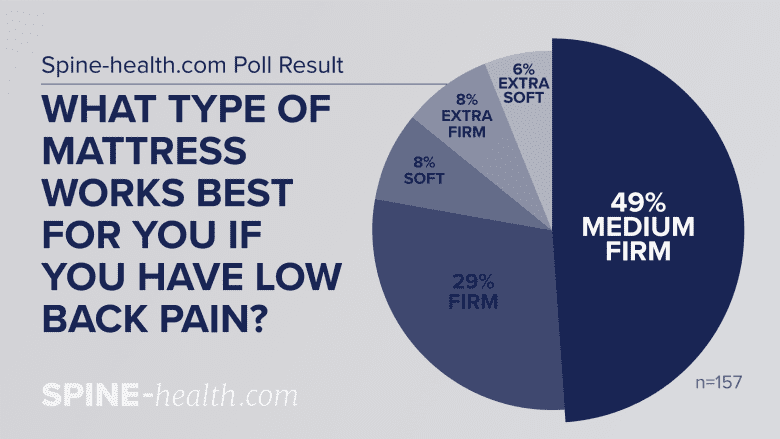
Poll results for what type of mattress works best for you if you have low back pain.
There is a limited amount of definitive medical research informing the best type of mattress firmness, but several studies indicate that a medium-firm mattress is preferable over a soft or firm one.
One well-referenced study published in The Lancet evaluated the effect of mattress firmness on 313 patients with chronic, nonspecific low back pain. The volunteers had reported pain while lying in bed and upon rising.4Kovacs FM, Abraira V, Pena A, Martin-Rodriguez JG, Sanchez-Vera M, Ferrer E, et al. Effect of firmness of mattress on chronic non-specific low-back pain: randomized, double-blind, controlled, multicentre trial. Lancet 2003;15:1599–1604. doi:10.1016/S0140-6736(03)14792-7
The participants were assigned either firm or medium-firm spring mattresses and were followed for 90 days.4Kovacs FM, Abraira V, Pena A, Martin-Rodriguez JG, Sanchez-Vera M, Ferrer E, et al. Effect of firmness of mattress on chronic non-specific low-back pain: randomized, double-blind, controlled, multicentre trial. Lancet 2003;15:1599–1604. doi:10.1016/S0140-6736(03)14792-7
Three primary variables were assessed4Kovacs FM, Abraira V, Pena A, Martin-Rodriguez JG, Sanchez-Vera M, Ferrer E, et al. Effect of firmness of mattress on chronic non-specific low-back pain: randomized, double-blind, controlled, multicentre trial. Lancet 2003;15:1599–1604. doi:10.1016/S0140-6736(03)14792-7:
- Pain intensity while lying in bed
- Pain intensity upon rising in the morning
- Disability level (during everyday activities)
The results showed the medium-firm mattresses were more effective than firm mattresses across all three measures.4Kovacs FM, Abraira V, Pena A, Martin-Rodriguez JG, Sanchez-Vera M, Ferrer E, et al. Effect of firmness of mattress on chronic non-specific low-back pain: randomized, double-blind, controlled, multicentre trial. Lancet 2003;15:1599–1604. doi:10.1016/S0140-6736(03)14792-7
In This Article:
- Choosing the Best Mattress for Lower Back Pain
- How to Evaluate a Mattress
In another well-referenced study, 59 volunteers rated their sleep quality, back pain, and back stiffness during a 4-week period of sleeping on their own beds, and did the same for 4 weeks while sleeping on a new medium-firm mattress.5Jacobson BH, Wallace T, Gemmell H. Subjective rating of perceived back pain, stiffness and sleep quality following introduction of medium-firm bedding systems. J Chiropr Med. 2006;5(4):128-134. doi:10.1016/S0899-3467(07)60145-1
Prior to the study, the participants did not have any specific back diagnoses or treatment, but reported back discomfort and stiffness.5Jacobson BH, Wallace T, Gemmell H. Subjective rating of perceived back pain, stiffness and sleep quality following introduction of medium-firm bedding systems. J Chiropr Med. 2006;5(4):128-134. doi:10.1016/S0899-3467(07)60145-1
The study results showed an immediate improvement in all scores of back pain, stiffness, and disability, with further improvements developing by the final week of the trial period with the medium-firm mattress.5Jacobson BH, Wallace T, Gemmell H. Subjective rating of perceived back pain, stiffness and sleep quality following introduction of medium-firm bedding systems. J Chiropr Med. 2006;5(4):128-134. doi:10.1016/S0899-3467(07)60145-1
Of note, in this study, all the participants’ original beds were more than 5 years old, with an average of 9 years,5Jacobson BH, Wallace T, Gemmell H. Subjective rating of perceived back pain, stiffness and sleep quality following introduction of medium-firm bedding systems. J Chiropr Med. 2006;5(4):128-134. doi:10.1016/S0899-3467(07)60145-1 so it is possible that getting a new mattress in and of itself is beneficial.
Guideline #2: Support your natural spinal alignment while sleeping
In this context, spinal alignment refers to maintaining the natural curves along the spine while sleeping.
To maintain optimal spinal alignment, your mattress should provide sturdy support for your lower back and pelvis, preventing it from sinking into the bed.1Caggiari G, Talesa GR, Toro G, Jannelli E, Monteleone G, Puddu L. What type of mattress should be chosen to avoid back pain and improve sleep quality? Review of the literature. J Orthop Traumatol. 2021;22(1):51. Published 2021 Dec 8. doi:10.1186/s10195-021-00616-5,2Radwan A, Fess P, James D, et al. Effect of different mattress designs on promoting sleep quality, pain reduction, and spinal alignment in adults with or without back pain; systematic review of controlled trials. Sleep Health. 2015;1(4):257-267. doi:10.1016/j.sleh.2015.08.001
Personalized support for spinal alignment can be achieved through several means, such as using pillows to support one’s sleeping position, a mattress topper, mattress selection/types, and/or a mattress that provides customized support for different body zones. Mattress companies use terms like zonal support or zoned support for these specialized mattresses.3Normand MC, Descarreaux M, Poulin C, et al. Biomechanical effects of a lumbar support in a mattress. J Can Chiropr Assoc. 2005;49(2):96-101. Available from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1840018/
Mattress technology has progressed significantly, and the area of more customized spinal support has grown. Mattresses made with variable zones for support are designed to achieve optimal spinal alignment compared to traditional soft or firm mattresses.
For example, a study published in the Journal of the National Sleep Foundation examined how a soft, firm, and custom-made mattress affects spinal alignment for side sleepers.6Leilnahari, K., Fatouraee, N., Khodalotfi, M. et al. Spine alignment in men during lateral sleep position: experimental study and modeling. BioMed Eng OnLine 10, 103 (2011). https://doi.org/10.1186/1475-925X-10-103 In this study, 25 men had markers placed on their spinous processes to track spinal alignment on each of the 3 types of mattresses.6Leilnahari, K., Fatouraee, N., Khodalotfi, M. et al. Spine alignment in men during lateral sleep position: experimental study and modeling. BioMed Eng OnLine 10, 103 (2011). https://doi.org/10.1186/1475-925X-10-103
This study revealed that custom-made mattresses provided the best support for spinal alignment, followed by firm mattresses, and then soft ones.6Leilnahari, K., Fatouraee, N., Khodalotfi, M. et al. Spine alignment in men during lateral sleep position: experimental study and modeling. BioMed Eng OnLine 10, 103 (2011). https://doi.org/10.1186/1475-925X-10-103
Further analysis showed that heavier men with wide shoulders (compared to hips) who sleep on their sides find the most benefit from custom-made mattresses.6Leilnahari, K., Fatouraee, N., Khodalotfi, M. et al. Spine alignment in men during lateral sleep position: experimental study and modeling. BioMed Eng OnLine 10, 103 (2011). https://doi.org/10.1186/1475-925X-10-103
Guideline #3: Sleep comfort is personalized
The comfort provided by a mattress and bedding is one of personal experience and is driven by several factors, such as:
- Minimizing pressure points while sleeping. For a side sleeper, this means minimizing pressure on the shoulder and hip, which in turn reduces nighttime awakenings and tossing and turning due to discomfort. Mattresses made with a pillowtop, and/or use of a mattress topper provide additional cushioning.
- The back pain diagnosis. The best bed and sleeping position should also be guided by the underlying cause(s) of back pain. The bedframe may also play a role, as people with some types of back pain will feel better with an adjustable bed frame that allows them to elevate their upper body on an incline and provides support under their knees.
- Temperature preference. People tend to have a temperature preference while sleeping, and some people “sleep hot” and will want to avoid a mattress or bedding that locks in heat.
- Sleep surface. Sleep comfort can be improved with the use of good pillows, and possibly a cushioned mattress, or a mattress topper, for adding extra softness on top of the mattress without sacrificing support.
- Aiding mobility. Getting in and out of bed is problematic for some people with back pain, and in this case, it becomes important to have sturdy mattress edges that don’t sink too far down. Some people find adjustable bed frames useful, as they can use the remote control to raise themselves up to a sitting position to aid in getting into and out of bed.
Most retailers offer sleep trials, such as a 100-day or even a 365-day trial period with an option to return for free, allowing buyers an option of trial and error to find the best match.
The bottom line is to aim for sleep comfort that fosters continuous sleep through the night and waking up feeling rested and rejuvenated.
- 1 Caggiari G, Talesa GR, Toro G, Jannelli E, Monteleone G, Puddu L. What type of mattress should be chosen to avoid back pain and improve sleep quality? Review of the literature. J Orthop Traumatol. 2021;22(1):51. Published 2021 Dec 8. doi:10.1186/s10195-021-00616-5
- 2 Radwan A, Fess P, James D, et al. Effect of different mattress designs on promoting sleep quality, pain reduction, and spinal alignment in adults with or without back pain; systematic review of controlled trials. Sleep Health. 2015;1(4):257-267. doi:10.1016/j.sleh.2015.08.001
- 3 Normand MC, Descarreaux M, Poulin C, et al. Biomechanical effects of a lumbar support in a mattress. J Can Chiropr Assoc. 2005;49(2):96-101. Available from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1840018/
- 4 Kovacs FM, Abraira V, Pena A, Martin-Rodriguez JG, Sanchez-Vera M, Ferrer E, et al. Effect of firmness of mattress on chronic non-specific low-back pain: randomized, double-blind, controlled, multicentre trial. Lancet 2003;15:1599–1604. doi:10.1016/S0140-6736(03)14792-7
- 5 Jacobson BH, Wallace T, Gemmell H. Subjective rating of perceived back pain, stiffness and sleep quality following introduction of medium-firm bedding systems. J Chiropr Med. 2006;5(4):128-134. doi:10.1016/S0899-3467(07)60145-1
- 6 Leilnahari, K., Fatouraee, N., Khodalotfi, M. et al. Spine alignment in men during lateral sleep position: experimental study and modeling. BioMed Eng OnLine 10, 103 (2011). https://doi.org/10.1186/1475-925X-10-103

