When a cervical disc starts losing hydration and stiffening, there are several ways in which neck pain and associated symptoms can develop. Here are the common ones.
In This Article:
- Cervical Degenerative Disc Disease
- Cervical Degenerative Disc Disease Symptoms and Diagnosis
- How Cervical Degenerative Disc Disease Causes Pain and Other Symptoms
- Cervical Degenerative Disc Disease Treatment Options
- Cervical Degenerative Disc Disease Video
Pain from a Degenerating Disc
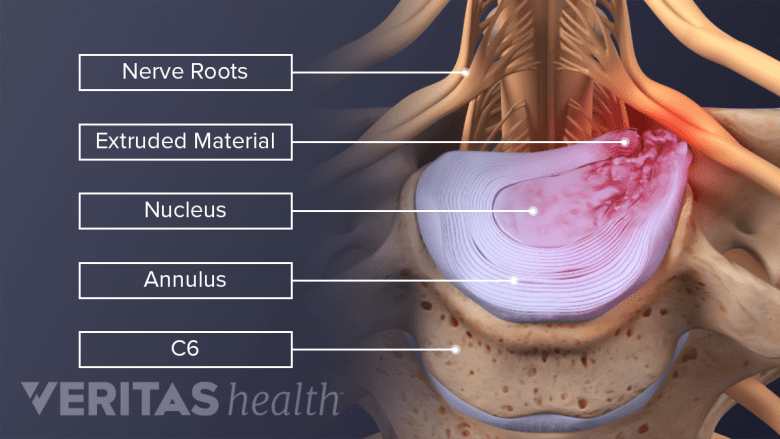
Inflammatory proteins leak out from the disc and irritate a nearby nerve root.
Most people who have a disc tear do not experience pain from it. The exact reason is unknown, but most experts suspect it has something to do with how the disc’s innervation and pain sensory can vary from person to person. For example, some people might have nerves that naturally go deeper into the disc, while some people might simply have a higher threshold for sensing pain.
When a degenerating disc causes neck pain, it is likely from one or both of the following:
Discogenic pain
This pain occurs in the disc itself and can range from mild to severe. The disc’s gel-like interior, called the nucleus pulposus, contains proteins that can cause painful inflammation if they come in contact with nerves located in the outer layer of the disc.
In a healthy adult cervical disc, nerves only go into the outer third of the disc’s protective outer layer, called the annulus fibrosus. However, if the disc’s outer layer gets a tear, then nerves can start to grow deeper into the disc in an attempt to heal itself. The soft inner portion of the disc can leak into the outer rings and come into contact with the small nerves, which can become painful. Some studies have even shown nerves growing all the way into the center of the nucleus pulposus in a painful disc that had gone through significant degeneration.
Micro-motion instability
When the disc’s tough outer layer wears down and no longer provides adequate shock absorption and stability, the vertebrae above and below the disc may move more than usual and surrounding muscles can go into painful spasms in an attempt to limit that abnormal movement.
Pain from a degenerating disc can range anywhere from a dull ache to something so intense that it limits movement and activities. In most cases, the pain will subside within a few weeks or months as chemical inflammation of the disc material starts to subside, and/or the disc stabilizes into it new stable position.
Other Conditions Associated with a Degenerating Disc

Radicular pain is a common symptom of conditions affecting the cervical spine.
Cervical degenerative disc disease is often present with other spinal conditions, either developing at the same time or in some cases one causes the other. Some common examples include:
-
Herniated Cervical Disc. A degenerating disc can have its nucleus wedge into tears in the annulus fibrosus. If the nucleus pulposus eventually passes through the annulus fibrosus, then the disc is considered herniated.
Conversely, a traumatic injury, such as a fall, or other issues could cause a herniated disc that eventually speeds up the disc’s degeneration and leads to cervical degenerative disc disease.
- Cervical osteoarthritis. As the disc degenerates and the disc space within the vertebral column starts to collapse, the facet joints may abnormally move or sublux and cause wear of the cartilage, as well as develop bone spurs in the neck.
- Cervical spinal stenosis. This condition occurs when there is a narrowing of the spinal canal (where the spinal cord runs through) or foramina (where the spinal nerve runs through), due to bone spurs, as described in the arthritis scenario above.
As an example, disc degeneration could eventually lead to osteoarthritis, which could eventually lead to spinal stenosis. For some patients, they are born with a congenital form of cervical stenosis and do not need to have disc degeneration to develop symptoms.
Cervical radiculopathy—symptoms of pain, tingling, numbness, and/or weakness radiating down the shoulder into the arm and hand—can result when one or more of the neck’s spinal roots becomes pinched or irritated. For example, a herniated disc or bone spur in the neck could pinch a nerve root in the C6-C7 segment that might cause weakness in the triceps and forearms, wrist drop, and altered sensation in the middle fingers or fingertips.
See What Is Cervical Radiculopathy?
If the spinal cord at the neck level becomes compressed by spinal stenosis, such as from bone spurs or a disc bulge, then myelopathy can develop. Possible symptoms of pain, tingling, numbness, and/or weakness could be felt at that level in the neck and anywhere below. For example, a person could have tingling or weakness in the legs, balance problems, or even difficulty with bowel and bladder control.
It is important to get a medical evaluation if there are symptoms of myelopathy, as the condition may progress and without treatment it is possible to eventually develop paralysis of multiple limbs and body functions.

