For some people, whiplash symptoms can be so minor that they go away within a couple days. For others, the symptoms can become varied and chronic, ranging from severe pain to cognitive and emotional problems.
Whiplash symptoms might manifest immediately following the acceleration-deceleration accident, or they can take a few hours or days to appear. Oftentimes the exact underlying cause remains unknown for some whiplash symptoms despite today’s best diagnostic techniques. Due to the potentially high number and varied complexity of whiplash symptoms, they are sometimes collectively referred to as whiplash-associated disorders.
In This Article:
- What Is Whiplash?
- Whiplash Symptoms and Associated Disorders
- Diagnosing Whiplash
- Whiplash Treatments and Recovery
- Whiplash Video
Common Whiplash Symptoms
Some of the most common symptoms of whiplash include:
Neck pain

Neck pain, neck stiffness, and reduced range of motion are common symptoms of a whiplash injury.
The pain could range anywhere from mild to severe. It might be located in one spot or general area, or it could also radiate down the shoulder into the arm and/or hand. Typically, neck pain from whiplash is caused by ligament sprains or muscle strains, but it can also be caused by injuries to discs, nerves, joints, and/or bones.
Neck stiffness or reduced range of motion
Reduced neck mobility could be from pain, tightening of a muscle, or a mechanical problem, such as with a joint.
See How to Treat Stiff Neck After Direct Trauma
Headache
Injury to the neck joints and muscles during whiplash can result in headaches.
A neck muscle tightening, or a nerve or joint of the cervical spine becoming irritated could cause headaches.
See What Is Causing My Neck Pain and Headache?
Neck instability
This whiplash symptom commonly results from stretched or torn soft tissues, such as ligaments. Although, it could also be caused by a fracture.
Shoulder and/or upper back pain
If the neck’s soft tissues, such as muscles or ligaments, are torn or strained during whiplash, then sometimes that pain can also be referred to other soft tissues in the upper back and shoulders.
See Could That Shoulder Pain Really Stem From the Neck?
Radiating tingling, weakness, or numbness
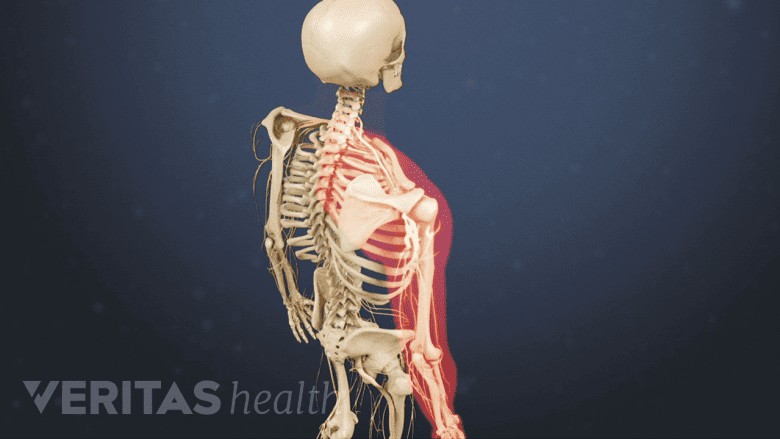
Whiplash can cause localized neck pain and radiating pain in the surrounding areas.
Sometimes whiplash can cause one of the neck’s spinal nerve roots to become compressed or inflamed, which can lead to cervical radiculopathy symptoms of tingling, weakness, and/or numbness radiating down the shoulder, arm, hand, and/or fingers. Typically, cervical radiculopathy is only felt on one side of the body, but in rare cases it can be felt on both sides if more than one nerve root is affected.
See Understanding Hand Pain and Numbness
Anywhere from just one whiplash symptom all the way up to numerous symptoms can present at once. Symptoms can also come and go at various times.
Other Whiplash Symptoms and Associated Disorders
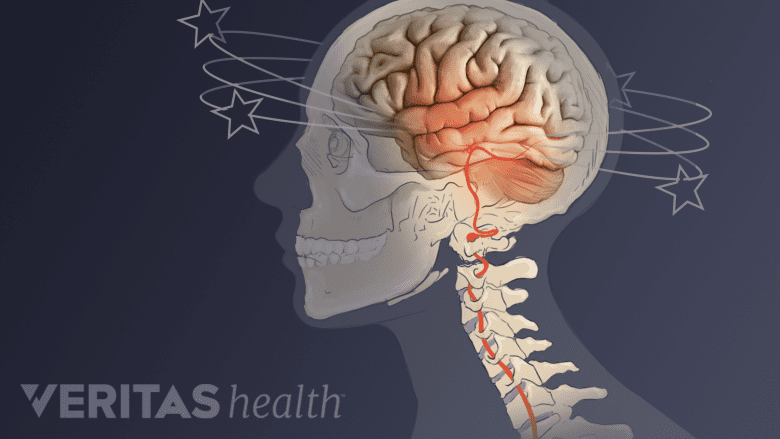
Whiplash-related dizziness can stem from neck instability or mild traumatic brain injury.
Other whiplash-associated disorders can include:
- Dizziness. Whiplash-related dizziness could be from neck instability or even a concussion (mild traumatic brain injury).
- Vision problems. Blurry vision or other visual deficits could result from any number of causes, including concussion or damage to a nerve. A vision problem could also contribute to dizziness.
- Emotional changes. A person might become more irritable, anxious, or even depressed. It can be hard to know if these changes are due to a concussion, post-traumatic stress syndrome, pain from the neck injury, or stress from the accident’s aftermath which could include litigation, financial worries, and/or the involvement of loved ones who were also injured.
- Ringing in ears. Also called tinnitus, this ringing or buzzing in one or both ears can range from intermittent and minor to constant and highly distracting. Any number of problems from whiplash could lead to tinnitus, such as an injury to the part of the brain that controls hearing, nerve or vascular damage, jaw injury, or even stress.
- Trouble getting good sleep. A person might find it difficult to fall asleep or stay asleep. These problems with sleeping well and waking refreshed could be due to various whiplash-related factors, such as pain, stress, or concussion.
- Fatigue. Lack of energy could be related to difficulty sleeping, depression, stress, pain, concussion, or various other causes.
- Memory and/or concentration problems. It’s possible for someone to develop cognitive symptoms after a whiplash injury. These troubles could involve difficulty with memory or thinking. Sometimes these symptoms start shortly after the injury, or they might not show up until hours or days later. Cognitive problems could be from a brain injury, or perhaps they could be related to various types of stress.
- Challenges with chewing, swallowing, or speaking. Sometimes trauma to muscles around the jaw can cause chewing or yawning to be painful.
- Difficulty swallowing. Injury to the larynx or esophagus could make swallowing painful or more difficult.
Sometimes whiplash symptoms persist or get worse with time, and finding their root causes often proves elusive.

