Doctors often come across misconceptions and superstitious beliefs about the causes of back pain and back problems. While several theories are passed down from well-meaning grandmothers, others come from content found on the internet. Learning the truth behind the myths from a trusted source is important for treating back problems in a medically accurate way and preventing further damage to the tissues.
In This Article:
- The Myths and Reality of Back Pain and Back Problems
- Myths about Causes of Back Pain and Back Problems
Myth: Lower Back Pain Is a Telltale Sign of Pregnancy

Lower back pain is one of the symptoms of pregnancy, typically observed in later stages.
Truth: Research indicates that anatomical and hormonal changes can cause back pain to occur in the later stages of pregnancy, during the second or third trimester, and only a small fraction of women develop back pain during the very early stages.1Sabino J, Grauer JN. Pregnancy and low back pain. Curr Rev Musculoskelet Med. 2008;1(2):137-141. doi:10.1007/s12178-008-9021-8
The possibility may be considered when back pain is accompanied by other revealing symptoms and signs, such as a missed menstrual period, morning sickness, fatigue, headache, and/or body soreness.
Myth: Gas Causes Back Pain

Back pain is usually unrelated to abdominal bloating and gas.
Truth: Abdominal bloating and intestinal gas can cause mild to severe discomfort in the upper body. An increased feeling of bloating and gas can result in tightness in the chest, occasionally accompanied by sharp pain. Back pain is usually not related to abdominal bloating and intestinal gas unless the pain from the abdomen is referred to the back, which is rare.
Back pain may result from gas bubbles within the spine and/or the cerebrospinal fluid, which is the fluid that covers and protects the spinal cord.2Abbassian A, Minaee B, Nikbakht Nasrabadi A, Rostamian A, Shirzad M. Gas as a cause of spinal pains: a possible new syndrome. Iran J Public Health. 2013;42(1):110-112. This gas differs from the intestinal gas and is not related to the symptoms caused by it. The spinal gas bubbles may move slightly depending on the posture and cause focal areas of pressure on the spinal tissues, resulting in upper or lower back pain.2Abbassian A, Minaee B, Nikbakht Nasrabadi A, Rostamian A, Shirzad M. Gas as a cause of spinal pains: a possible new syndrome. Iran J Public Health. 2013;42(1):110-112.
Myth: Sitting Causes Back Pain
Adopting a posture that provides adequate support while sitting decreases the risk of developing low back pain.
Truth: Sitting is an active process and engages the muscles and joints in the spine, hips, and pelvis. When an ergonomically supported posture is adopted while sitting, the stress on these tissues and joints is minimal and does not cause pain.
To minimize these stresses, the following postural adaptations are recommended3Pavilack, L., Alstedter, N. & Wisniewski, E. Pain-free posture handbook : 40 dynamic easy exercises to look and feel your best. Berkeley, CA: Althea Press; 2016.:
- Sitting straight with the shoulders rolled back and shoulder blades down.
- Keeping both legs hip-distance apart with feet flat on the floor.
- Ensuring that the spine follows its natural curve; placing a small pillow or rolled-up towel to support the lower back.
Even while adopting a supported posture, it is advisable to take frequent breaks, every hour, by getting up, walking around, and/or doing simple stretches.
Following these steps allows the upper and lower back to remain supported at all times and ensures the proper blood flow and nutrition supply to the spinal tissues. When sitting for long hours for work, using active workstations, such as sit-to-stand desks or stability balls allow the body to stay dynamic while seated, can reduce the risk of developing back pain.4Doroff CE, Langford EL, Ryan GA, Snarr RL. Effects of Active Sitting on Reading and Typing Task Productivity. Int J Exerc Sci. 2019;12(5):1216-1224. Published 2019 Nov 1.
Unsupported sitting postures, which include prolonged hunching or slouching, can cause the abdominal muscles to become strained and painful. Over time, their blood supply is reduced, slowly developing stiffness and weakness in the trunk and lower back.5Wong KC, Lee RY, Yeung SS. The association between back pain and trunk posture of workers in a special school for the severe handicaps. BMC Musculoskelet Disord. 2009;10:43. Published 2009 Apr 29. doi:10.1186/1471-2474-10-43 Prolonged sitting in an unsupported posture may also increase loads on the lower spinal discs, causing herniation and back pain with or without sciatica.6Alamin TF, Agarwal V, Zagel A, Qeli A. The effect of standing vs. variants of the seated position on lumbar intersegmental angulation and spacing: a radiographic study of 20 asymptomatic subjects. J Spine Surg. 2018;4(3):509–515. doi:10.21037/jss.2018.08.03,7Kwon Y, Kim JW, Heo JH, Jeon HM, Choi EB, Eom GM. The effect of sitting posture on the loads at cervico-thoracic and lumbosacral joints. Technol Health Care. 2018;26(S1):409–418. doi:10.3233/THC-174717
Myth: Constipation Does Not Cause Back Pain

Constipation may lead to discomfort or referred pain in the lower back region.
Truth: While constipation does not directly affect the lower back tissues, this condition can cause specific disruptions in the body, which may cause or increase back pain.8Arai YC, Shiro Y, Funak Y, et al. The Association Between Constipation or Stool Consistency and Pain Severity in Patients With Chronic Pain. Anesth Pain Med. 2018;8(4):e69275. Published 2018 Aug 11.
- Constipation may alter the balance of the gut microbiome (microbes in the intestine), which may result in increased pain perception and anxiety.8Arai YC, Shiro Y, Funak Y, et al. The Association Between Constipation or Stool Consistency and Pain Severity in Patients With Chronic Pain. Anesth Pain Med. 2018;8(4):e69275. Published 2018 Aug 11.
- Constipation is associated with insufficient physical activity and excessive sedentary behavior, which can cause chronic lower back pain.8Arai YC, Shiro Y, Funak Y, et al. The Association Between Constipation or Stool Consistency and Pain Severity in Patients With Chronic Pain. Anesth Pain Med. 2018;8(4):e69275. Published 2018 Aug 11.
Women are 2 to 3 times more likely to get constipation compared to men.9Tantawy SA, Kamel DM, Abdelbasset WK, Elgohary HM. Effects of a proposed physical activity and diet control to manage constipation in middle-aged obese women. Diabetes Metab Syndr Obes. 2017;10:513-519. Published 2017 Dec 14. doi:10.2147/DMSO.S140250
Myth: Stress Does Not Affect Back Pain
Truth: Stress is an emotional experience that can cause behavioral and psychological alterations in the body – elevating the perception of lower back pain. Depression and anxiety are thought to be the most common stress-related conditions associated with lower back pain.10Ellegaard H, Pedersen BD. Stress is dominant in patients with depression and chronic low back pain. A qualitative study of psychotherapeutic interventions for patients with non-specific low back pain of 3-12 months' duration. BMC Musculoskelet Disord. 2012;13:166. Published 2012 Sep 6. doi:10.1186/1471-2474-13-166
Research suggests that certain life stressors such as lack of social support and demanding jobs are associated with musculoskeletal back pain.11Alturkistani LH, Hendi OM, Bajaber AS, et al. Prevalence of Lower Back Pain and its Relation to Stress Among Medical Students in Taif University, Saudi Arabia. Int J Prev Med. 2020;11:35. Published 2020 Mar 16. doi:10.4103/ijpvm.IJPVM_264_19 For treating back pain associated with stress, individual psychological management is recommended as the primary treatment, followed by medical treatment for the back problem.10Ellegaard H, Pedersen BD. Stress is dominant in patients with depression and chronic low back pain. A qualitative study of psychotherapeutic interventions for patients with non-specific low back pain of 3-12 months' duration. BMC Musculoskelet Disord. 2012;13:166. Published 2012 Sep 6. doi:10.1186/1471-2474-13-166
Myth: Back Pain Is Not Related to Kidney Problems
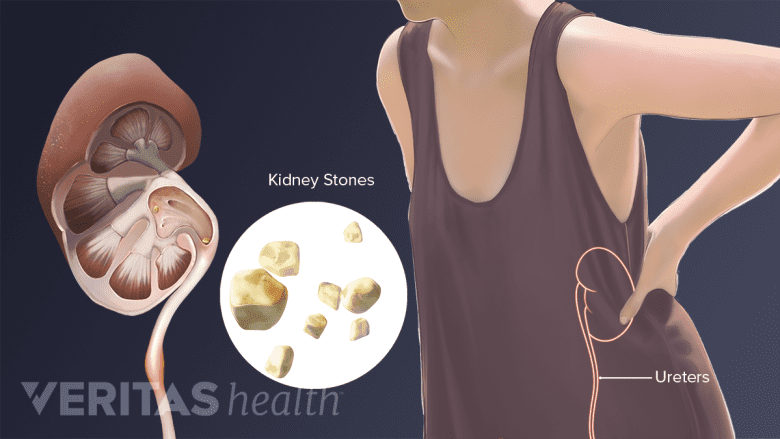
Kidney stones may cause moderate to severe back pain.
Truth: Certain problems related to the kidney(s) can cause back pain that is severe enough for an emergency room visit. The two most common kidney problems that can cause moderate to severe back pain are kidney stones and a kidney infection.12Nagayama M, Yanagawa Y, Aihara K, et al. Analysis of non-traumatic truncal back pain in patients who visited an emergency room. Acute Med Surg. 2014;1(2):94-100. Published 2014 Jan 28. doi:10.1002/ams2.16 The symptoms can occur on the left and/or right side of the lower back depending on the affected kidney and may be felt as a dull ache or a sharp, stabbing pain.
A more serious kidney condition, renal cell carcinoma, can cause lower back pain.13Watkins CT, Tao C, Yochum TR. Renal cell carcinoma in a 44-year-old man: an etiology for low back pain. Journal of Manipulative and Physiological Therapeutics. 2009;32(7):597-600.,14Rectenwald R. A case study of back pain and renal cell carcinoma. J Chiropr Med. 2008;7(1):24-27. doi:10.1016/j.jcme.2008.01.001 This condition, also called adenocarcinoma, is cancerous and has the ability to spread to other parts of the body (metastasize). Back pain in renal cell carcinoma may be similar to vertebral spondylolisthesis, causing severe sciatica-like symptoms, such as radiating leg pain. The symptoms usually occur at night.13Watkins CT, Tao C, Yochum TR. Renal cell carcinoma in a 44-year-old man: an etiology for low back pain. Journal of Manipulative and Physiological Therapeutics. 2009;32(7):597-600.
- 1 Sabino J, Grauer JN. Pregnancy and low back pain. Curr Rev Musculoskelet Med. 2008;1(2):137-141. doi:10.1007/s12178-008-9021-8
- 2 Abbassian A, Minaee B, Nikbakht Nasrabadi A, Rostamian A, Shirzad M. Gas as a cause of spinal pains: a possible new syndrome. Iran J Public Health. 2013;42(1):110-112.
- 3 Pavilack, L., Alstedter, N. & Wisniewski, E. Pain-free posture handbook : 40 dynamic easy exercises to look and feel your best. Berkeley, CA: Althea Press; 2016.
- 4 Doroff CE, Langford EL, Ryan GA, Snarr RL. Effects of Active Sitting on Reading and Typing Task Productivity. Int J Exerc Sci. 2019;12(5):1216-1224. Published 2019 Nov 1.
- 5 Wong KC, Lee RY, Yeung SS. The association between back pain and trunk posture of workers in a special school for the severe handicaps. BMC Musculoskelet Disord. 2009;10:43. Published 2009 Apr 29. doi:10.1186/1471-2474-10-43
- 6 Alamin TF, Agarwal V, Zagel A, Qeli A. The effect of standing vs. variants of the seated position on lumbar intersegmental angulation and spacing: a radiographic study of 20 asymptomatic subjects. J Spine Surg. 2018;4(3):509–515. doi:10.21037/jss.2018.08.03
- 7 Kwon Y, Kim JW, Heo JH, Jeon HM, Choi EB, Eom GM. The effect of sitting posture on the loads at cervico-thoracic and lumbosacral joints. Technol Health Care. 2018;26(S1):409–418. doi:10.3233/THC-174717
- 8 Arai YC, Shiro Y, Funak Y, et al. The Association Between Constipation or Stool Consistency and Pain Severity in Patients With Chronic Pain. Anesth Pain Med. 2018;8(4):e69275. Published 2018 Aug 11.
- 9 Tantawy SA, Kamel DM, Abdelbasset WK, Elgohary HM. Effects of a proposed physical activity and diet control to manage constipation in middle-aged obese women. Diabetes Metab Syndr Obes. 2017;10:513-519. Published 2017 Dec 14. doi:10.2147/DMSO.S140250
- 10 Ellegaard H, Pedersen BD. Stress is dominant in patients with depression and chronic low back pain. A qualitative study of psychotherapeutic interventions for patients with non-specific low back pain of 3-12 months' duration. BMC Musculoskelet Disord. 2012;13:166. Published 2012 Sep 6. doi:10.1186/1471-2474-13-166
- 11 Alturkistani LH, Hendi OM, Bajaber AS, et al. Prevalence of Lower Back Pain and its Relation to Stress Among Medical Students in Taif University, Saudi Arabia. Int J Prev Med. 2020;11:35. Published 2020 Mar 16. doi:10.4103/ijpvm.IJPVM_264_19
- 12 Nagayama M, Yanagawa Y, Aihara K, et al. Analysis of non-traumatic truncal back pain in patients who visited an emergency room. Acute Med Surg. 2014;1(2):94-100. Published 2014 Jan 28. doi:10.1002/ams2.16
- 13 Watkins CT, Tao C, Yochum TR. Renal cell carcinoma in a 44-year-old man: an etiology for low back pain. Journal of Manipulative and Physiological Therapeutics. 2009;32(7):597-600.
- 14 Rectenwald R. A case study of back pain and renal cell carcinoma. J Chiropr Med. 2008;7(1):24-27. doi:10.1016/j.jcme.2008.01.001

