The diagnosis of cervical myelopathy associated with cervical spondylosis depends to a large extent on the patient's history and the physical findings described on page one of this article.

The diagnosis may then be confirmed by radiologic imaging, such as an MRI scan of the cervical spine demonstrating overt spinal cord and nerve root compression.
In This Article:
- Cervical Spondylosis with Myelopathy
- Cervical Spondylosis and Cervical Myelopathy Symptoms
- Diagnosis of Spondylosis with Cervical Myelopathy
- Cervical Myelopathy Treatment
- Cervical Spondylosis with Myelopathy Animation
Additional Diagnostic Studies

Several imaging techniques may aid in diagnosing cervical spine problems.
Additional diagnostic studies often performed help provide further levels of detail and may aid in planning for treatment:
- In certain instances (especially when the details of bone anatomy must be seen clearly), a cervical myelogram and post-myelogram CT scan may aid in determination of the anatomy associated with nerve root and spinal cord compression.
- Advanced cases may show abnormal signal within the spinal cord on MRI imaging and/or atrophy of the spinal cord due to nerve cell loss. In such cases, referred to as "myelomalacia," surgical outcomes may not be as promising.
- Flexion/extension cervical spine films to rule out translational instability of the cervical vertebral bodies, which can influence the choice of treatment as well as the extent of treatment.
- Somatosensory evoked potentials (SSEPs) or motor evoked potentials (MEPs) to provide a measure of the electrical conductivity of the spinal cord across the compressed segments. Such testing may also be performed as a baseline in anticipation of monitoring of the spinal cord during surgery itself with the same studies.
Differential Diagnosis
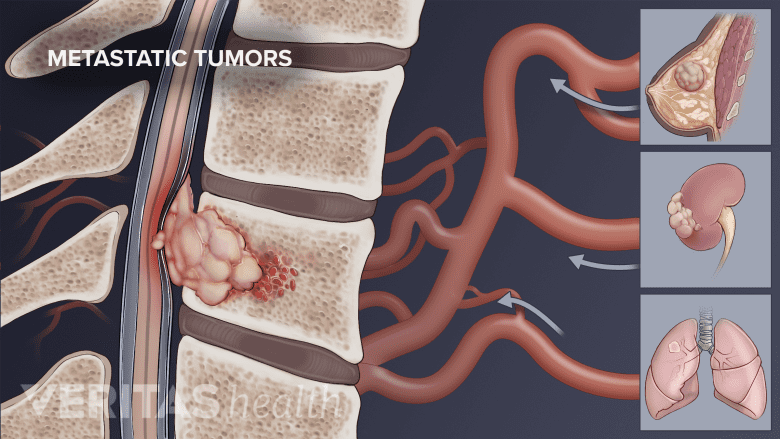
Certain spinal cord tumors may have similar symptoms as cervical spondylotic myelopathy.
To arrive at an accurate diagnosis, it is critical for the physician to consider other disorders that have similar symptoms as cervical spondylotic myelopathy (a "differential diagnosis").
Other conditions associated with neck pain and arm pain, motor-sensory-reflex changes, and signs of spinal cord dysfunction include
- Progressive forms of multiple sclerosis
- Amyotrophic lateral sclerosis (Lou Gehrig's disease)
- Hereditary spastic paraplegia
- Sub acute combined degeneration of the spinal cord associated with vitamin B12 deficiency
- Certain spinal cord tumors or vascular conditions, such as an AVM (anteriovenous malformation)
- Combined system disease

