A computed tomography scan with myelogram, also called CT myelography, is a minimally invasive diagnostic study that combines the comprehensive imaging advantages of myelography and the high resolution of a conventional CT. 1 Patel DM, Weinberg BD, Hoch MJ. CT Myelography: Clinical Indications and Imaging Findings. RadioGraphics. 2020;40(2):470-484. doi: 10.1148/rg.2020190135 The technique involves two basic steps:
- Injecting a radiographically opaque dye (which is illuminated by x-ray) into the spine, which deposits near the space around the spinal nerve roots
- Conducting a CT scan by discharging a series of x-ray beams around the area to be imaged, creating a sequence of two-dimensional images, and illuminating the areas where the dye gets deposited
This combination study provides excellent spatial resolution to portray details of the spinal bones and spinal cord, making it an important diagnostic tool in the evaluation of several spinal conditions. 1 Patel DM, Weinberg BD, Hoch MJ. CT Myelography: Clinical Indications and Imaging Findings. RadioGraphics. 2020;40(2):470-484. doi: 10.1148/rg.2020190135
CT with myelogram is complementary to other detailed diagnostic studies, such as magnetic resonance imaging (MRI)—and is recommended when these studies are contraindicated or inadequate, or high-resolution functional spine imaging is required for pre-or postsurgical evaluation.
In This Article:
- Introduction to Diagnostic Studies for Back and Neck Pain
- X-Ray of the Spine
- Computerized Tomography (CT) Scan
- Computerized Tomography (CT) Scan with Myelogram
- Electromyography (EMG)
- Somatosensory Evoked Potentials (SSEP)
How CT Myelography Is Different from MRI
Both MRI and CT myelography provide quality images of the spinal tissues. MRI scans are popular due to their noninvasive imaging technique, lack of ionizing radiation, and high-contrast resolution. Despite these advantages, the presence of metals, surgical fittings, or injuries from metallic objects lodged in the body, can make an MRI scan impossible. Also, patient-related factors, such as body habitus, a feeling of claustrophobia, and/or the inability to stay still for a long duration can make MRI a difficult option. 1 Patel DM, Weinberg BD, Hoch MJ. CT Myelography: Clinical Indications and Imaging Findings. RadioGraphics. 2020;40(2):470-484. doi: 10.1148/rg.2020190135
In these cases, CT myelography may serve as a useful alternative. The CT myelography technique also allows for the patient to be positioned in different ways (bending the spine forward and/or backward) while performing the test, capturing various dynamic views from different angles, which is not possible in MRI. 1 Patel DM, Weinberg BD, Hoch MJ. CT Myelography: Clinical Indications and Imaging Findings. RadioGraphics. 2020;40(2):470-484. doi: 10.1148/rg.2020190135
MRI has overall better contrast resolution than CT myelography, but the injected contrast agent in CT myelography provides excellent contrast resolution of the spinal cord and nerve roots in the spine. 1 Patel DM, Weinberg BD, Hoch MJ. CT Myelography: Clinical Indications and Imaging Findings. RadioGraphics. 2020;40(2):470-484. doi: 10.1148/rg.2020190135
Uses of Spinal CT with Myelogram
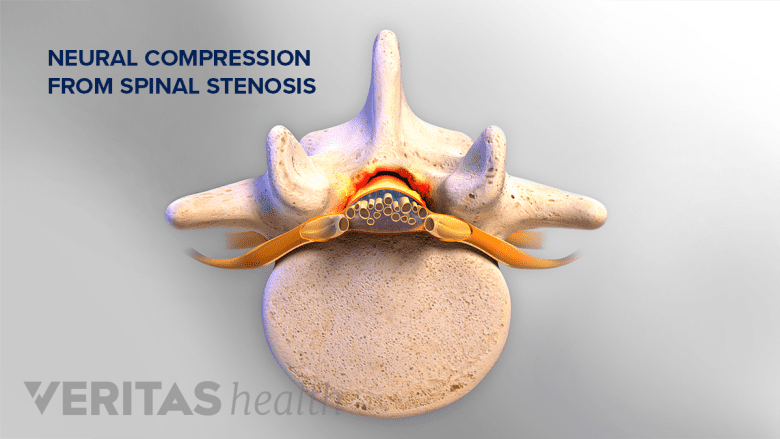
A CT scan with myelogram helps diagnose back or neck pain from spinal conditions like stenosis.
A CT scan with myelogram dynamically demonstrates the structures that contact, compress, or displace the spinal cord, nerve roots, and/or thecal sac (group of membranes surrounding the spinal cord and cauda equina), assisting in the diagnosis of back or neck pain from 1 Patel DM, Weinberg BD, Hoch MJ. CT Myelography: Clinical Indications and Imaging Findings. RadioGraphics. 2020;40(2):470-484. doi: 10.1148/rg.2020190135 :
- Degenerative conditions affecting the spinal canal and/or neural foramina, such as spinal stenosis
- Arachnoid conditions (conditions affecting the thin, transparent membrane loosely surrounding the spinal cord), such as arachnoid web, adhesions, arachnoid cysts
- Bone-related problems in the spine, including degenerative changes; defects; and injuries, such as facet joint osteoarthritis and osteoarthritis of the spine
- Cancers and tumors of the spine, including metastatic spine tumors
CT myelogram may also be used while a surgeon is performing a surgical procedure, to help guide the instrument or needle to the accurate target tissue.
Risks of Spinal CT with Myelogram
Spinal headache is a potential side effect of a CT scan with myelogram.
As with any radiographic imaging technique, CT is associated with the risk of exposure to ionizing radiation. The benefit of an accurate diagnosis usually outweighs this risk in most people, except in pregnant women due to the potential damage to the growing fetus. If pregnancy is suspected or confirmed, the treating physician should be informed, and alternative studies may be recommended.
The coexistent myelogram process may incur risks due to the injection procedure or the dye used in the process.
- Spinal headache. A spinal headache may occur due to needle puncture of the membranes covering the spinal cord, causing a leak of spinal fluid. Spinal headache usually increases when the patient is upright and subsides on lying down. The headache typically begins within 2 to 3 days after the procedure and resolves with rest and fluid intake. If the spinal headache continues, a procedure called "epidural blood patch" may be performed, where blood is withdrawn from the patient's arm and injected into the epidural space in the back (to create a blood patch). This procedure places pressure over the site that is leaking spinal fluid to stop the leak and in turn resolve the headache.
- Allergic reaction to the dye. Adverse reactions to the injected dye are rare and usually mild. Symptoms may include itching, rash, sneezing, nausea, and/or anxiety. Serious adverse reactions, such as hives, are rarely encountered.
- Nerve root and spinal cord damage. Rarely, injury from the spinal needle and bleeding around the nerve roots in the spinal canal may result in weakness and/or numbness in the treated area or infection of the spinal cord.
Mild pain at the injection site usually resolves in a day or two and may be treated with ice packs.
CT myelography is done on an outpatient basis and patients return home the same day. Any troubling symptoms after a CT myelography procedure must be discussed with the treating physician.
When indicated, CT with myelogram is a useful tool in the complete treatment process of back and neck pain. This study helps surgeons assess the spinal structures during surgeries and in following up after surgery to evaluate the progress of treatment and healing of the spine.
Read more about Getting an Accurate Back Pain Diagnosis
- 1 Patel DM, Weinberg BD, Hoch MJ. CT Myelography: Clinical Indications and Imaging Findings. RadioGraphics. 2020;40(2):470-484. doi: 10.1148/rg.2020190135

