Cervicogenic headache (CGH) is characterized by a dull, non-throbbing pain that radiates from the neck to back of the head. The pain may spread along the scalp and affect the forehead, temple, and area around the eye and/or ear.
CGH is a secondary headache that occurs when pain from an underlying source in the neck is felt in the head. Common causes of CGH include injury or trauma to the cervical spine, or systemic conditions such as rheumatoid arthritis, cancer, or infections.
In This Article:
- What Is Causing My Neck Pain and Headache?
- How Neck Pain and Headache Can Occur Together
- Neck Pain and Cervicogenic Headache
- Neck Pain and Tension Headache
- Neck Pain and Migraine Headache
How Neck Pain May Feel With CGH
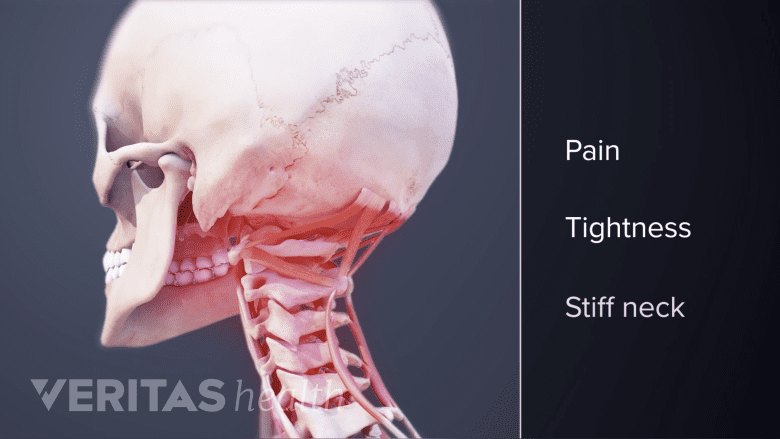
Cervicogenic headaches cause neck stiffness and restricted range of motion.
CGH pain starts in the neck and is commonly felt as a steady dull ache that may be aggravated by certain activities or postures. While CGH is typically a one-sided pain, both sides of the neck may be painful depending on the severity. In mild CGH, the neck pain is usually present only on the affected side; but in severe cases both sides of the neck may be painful. However, pain on the affected side is more dominant in severe cases. 1Sjaastad O, Fredriksen T. Cervicogenic headache: criteria, classification and epidemiology. Clin Exp Rheumatol. 2000;18:S-3. CGH may also be accompanied by some neck stiffness and reduced range of motion.
Read more: What Is Cervicogenic Headache?
Headache without neck pain can also occur in CGH. In these cases, the source of CGH may not cause neck pain, but may be tender to touch. Abnormal head movements or applying pressure (by pressing) on the back of the neck may trigger CGH.
Other Symptoms of Cervicogenic Headache

Cervicogenic headache originates at the base of the neck and extends into the forehead.
CGH may be intermittent or occur as a continuous headache. In addition to neck pain, other common symptoms of CGH may include:
- Headache. The neck pain radiates to the back of the head along the scalp and spreads over to the top of the head. The headache is felt as a dull, non-throbbing pain of mild to moderate intensity.
- Pain radiating to other areas. The pain may extend over to the forehead, temple, and area around the eye, and/or ear.
- Shoulder and arm pain. Pain in the shoulder and/or arm of the affected side is also common.
- Side-locked pain. The pain always affects one side of the head and neck.
- Blurred vision. The eye of the affected side may have blurred vision in some cases.
Many other CGH symptoms are possible but less common, such as nausea, sensitivity to light or sound, and dizziness. CGH may start as an intermittent headache and progress over time to become a continuous chronic headache. The severity and duration of CGH headache varies with each episode/exacerbation, ranging from mild to severe.
See What Causes Neck Pain and Dizziness?
Comparison of CGH with Other Headaches
Although CGH is a distinct disorder, certain symptoms may mimic migraine or tension-type headaches.
- Like CGH, migraines generally occur on one side of the head; however, CGH pain is non-throbbing and always affects the same side.
- Migraine symptoms such as nausea and sensitivity to light and sounds may be seen in rare cases of CGH.
- As in CGH, migraine pain worsens with continued activity.
- Tenderness in the muscles of the head and neck are common in both CGH and tension-type headache.
- CGH can occur at the same time along with migraine headache or tension type headache, or even trigger them.
Some occupations may increase the risk for CGH, such as hair stylists, carpenters, and drivers due to their head posture while working.2Page P. Cervicogenic Headaches: An Evidence-Led Approach To Clinical Management. International Journal of Sports Physical Therapy. 2011;6(3):254-266. CGH can be differentiated from other headaches with the help of physical examination, medical history, and diagnostic tests. Diagnostic nerve block tests are useful in identifying the exact source of CGH pain in the cervical spine.
When to Seek Medical Attention in CGH

Cervicogenic headache with arm pain and weakness necessitates medical attention.
Immediate medical attention is required in CGH caused due to serious underlying conditions such as infections, tumors or vascular complications in the head or neck. Symptoms in such cases include but are not limited to severe headache even after continued treatment, pain and tingling down the arms, high fever with stiff neck, seizures, and/or pain on coughing, sneezing, running, bending, or Valsalva maneuver.
See When Is a Stiff Neck Serious?
Once diagnosed, CGH can be well managed with appropriate treatment. Non-invasive treatments are started first, and commonly include manual therapy, medication, exercise, instrument-assisted soft tissue mobilization, and transcutaneous electrical nerve stimulation (TENS). Injections or surgeries may be considered in severe cases of CGH.

