Choice of treatment for a spine compression fracture depends first on getting an accurate diagnosis of the cause of the fracture.
In This Article:
- When Back Pain Is a Spine Compression Fracture
- Vertebral Fracture Symptoms
- Osteoporosis: The Primary Cause of Collapsed Vertebrae
- Diagnosing Vertebral Compression Fractures
- Compression Fracture Treatment
Osteoporosis
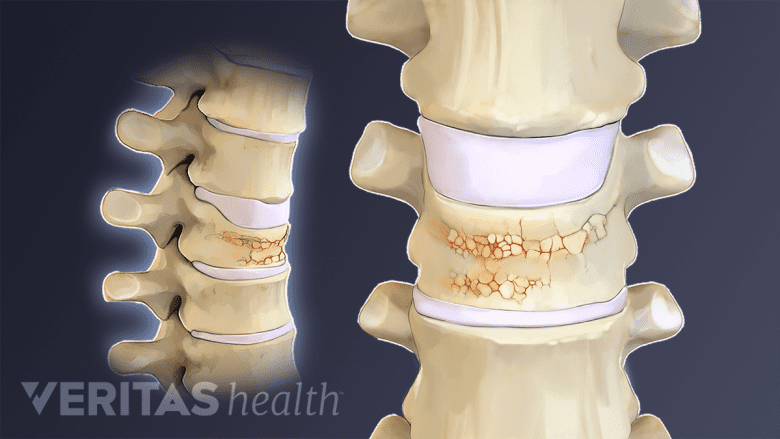
Osteoporosis is by far the most common cause of vertebral compression fractures, especially in women over the age of 50. It is also more common than most people think in people age 40-50, and it is reasonably common in men over age 50.
See Who Is at Risk for Osteoporosis?
Osteoporosis causes bones to thin and become more brittle and weak. The thinning bones can collapse during normal activity, leading to a spinal fracture. These compression fractures can cause a great deal of pain and can permanently alter the shape and strength of the spine.
Spinal fractures due to osteoporosis often occur while doing something that causes relatively minor trauma to the spine, such as opening a window, an insignificant fall, or twisting while lifting.
Advanced cases of osteoporosis can even lead to a vertebral fracture with routine activities that would normally not cause any trauma, such as sneezing, coughing, or turning over in bed.
Trauma
Trauma to the spinal vertebrae can also lead to minor or severe fractures. Such trauma could come from a fall, a forceful jump, a car accident, or any event that stresses the bones in the spine past its breaking point.
Cancer/Tumor
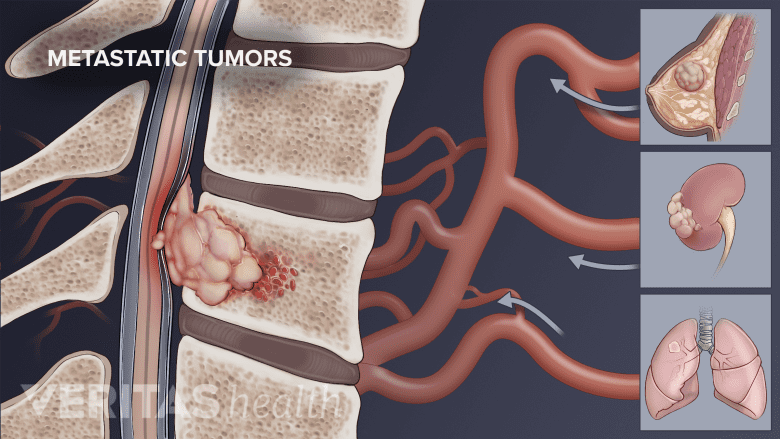
Metastatic tumors can weaken the vertebrae, leading to possible fractures.
Some types of cancer can also cause a weakening of the vertebrae in the spine to the point where they may fracture. It is not uncommon for metastatic cancer that starts in another part of the body to spread to bones in the spine.
A compression fracture of the spine that appears for little or no reason may be the first indication that an unrecognized cancer has spread to the spine. Cancer or multiple myeloma should be considered in patients who also have hypercalcemia, otherwise unexplained anemia, weight loss, or proteinuria.
The first step in obtaining the best treatment is to get an accurate diagnosis of the compression fracture and the underlying cause of the fracture.

