The thoracic spine has 12 nerve roots (T1 to T12) on each side of the spine that branch from the spinal cord and control motor and sensory signals mostly for the upper back, chest, and abdomen.
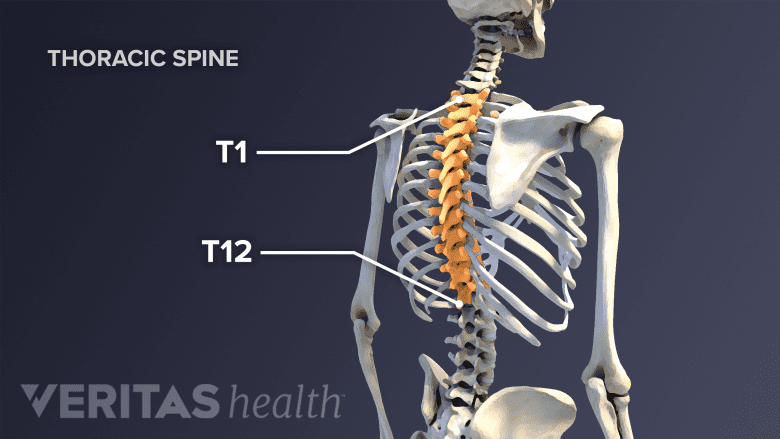
Each thoracic spinal nerve is named for the vertebra above it. For example, the T3 nerve root runs between the T3 vertebra and T4 vertebra. There are 12 thoracic spinal nerve root pairs (two at each thoracic vertebral level), starting at vertebral level T1-T2 and going down to T12-L1.
In This Article:
Thoracic Nerve Functions
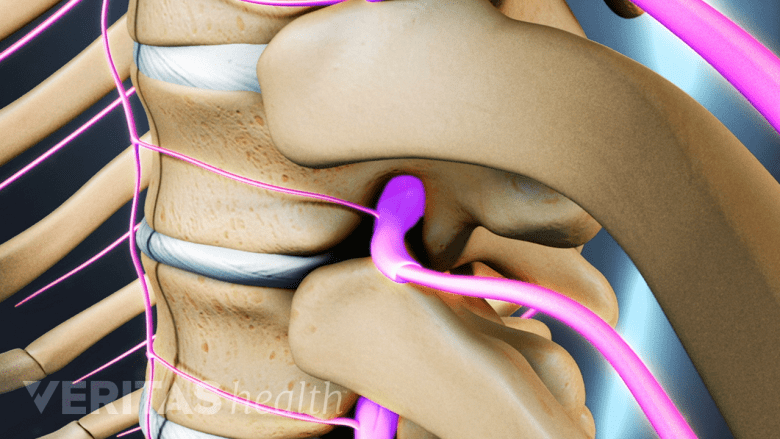
Nerves exit the spinal column through the intervertebral foramina.
Each thoracic nerve root exits the spinal canal through a bony hole, called an intervertebral foramen. This bony hole is formed by two adjacent vertebrae, and its size and shape can slightly shift as the vertebrae move.
See Vertebrae in the Vertebral Column
After branching from the spinal cord and traveling through the foramen, a thoracic nerve root branches into two different nerve bundles that feed into the nerves at the front (ventral ramus) and back (dorsal ramus) of the body. At the T1 through T11 levels, the ventral ramus eventually becomes an intercostal nerve that travels along the same path as the ribs (specifically between the innermost and internal intercostal muscles that connect adjacent ribs). At T12, the ventral ramus becomes a subcostal nerve that travels beneath the twelfth rib. At T1 through T12, the dorsal ramus goes into the back muscles and also provides sensation to the skin.
The motor and sensory functions provided by a thoracic nerve root are determined by its vertebral level. While these functions can slightly vary from person to person, they typically are as follows:
- T1 and T2 (top two thoracic nerves) feed into nerves that go into the top of the chest as well as into the arm and hand.
- T3, T4, and T5 feed into the chest wall and aid in breathing.
- T6, T7, and T8 can feed into the chest and/or down into the abdomen.
- T9, T10, T11, and T12 can feed into the abdomen and/or lower in the back. Watch Spinal Motion Segment: T12-L1 Animation
How Thoracic Nerves Can Become Painful

Thoracic spinal nerves become painful when they are impinged by a herniated disc or degenerative spinal changes.
If any of the thoracic nerves become inflamed, such as from a thoracic herniated disc or a narrowing of the foramen, thoracic radiculopathy can develop with symptoms of pain, tingling, numbness, and/or weakness radiating along the nerve root. These symptoms typically follow a pattern as noted above, based on the affected nerve root’s location and functions. For example, T3 radiculopathy could radiate pain and other symptoms into the chest via the branch of the nerve root that becomes an intercostal nerve traveling along the route between the third and fourth ribs. Also, if the branch of the thoracic nerve going toward the back becomes inflamed, pain and other symptoms could be felt in the back at or near the location of the inflammation.
See Radiculopathy, Radiculitis and Radicular Pain
It should also be noted that a severe strain of a muscle between ribs (intercostal muscle) may cause an intercostal nerve to become inflamed, painful, and possibly make breathing more difficult.
Thoracic Spinal Cord Injury
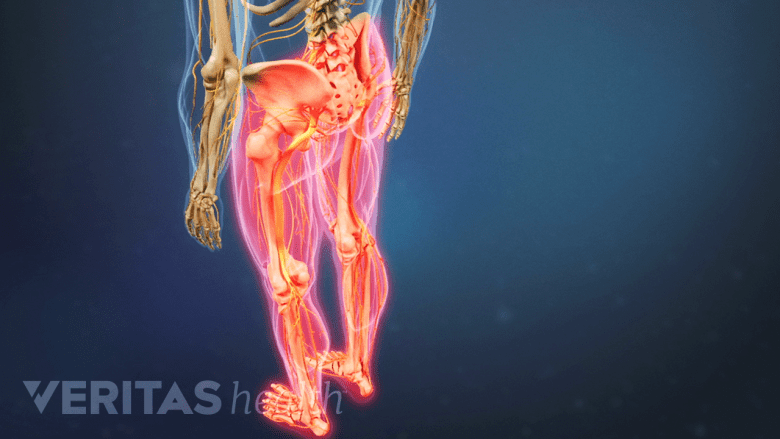
Serious injury to the spinal cord could lead to permanent dysfunction in the lower body.
The spinal cord is the main bundle of nerves that runs from the base of the brain all the way down through the cervical spine and thoracic spine before splitting into a bundle of nerve roots (cauda equina) in the lumbar spine. The brain exchanges electrical signals with the rest of the body via the spinal cord.
Watch Spinal Cord and Spinal Nerves: What is the Difference? Animation
The spinal cord is normally protected within the spinal canal. However, if a vertebra is fractured by trauma, such as a motor vehicle accident or gunshot wound, it is possible for the spinal cord to sustain a lesion that leads to a permanent injury.
Spinal cord injuries are usually classified based on the spinal nerve root level where function is reduced or completely lost. For example, a T6 spinal cord injury would impair or lose function at the T6 nerve root level and below. In this case, the person would likely have full use of the arms and breathing ability, but may have weakness, numbness, and other problems in the abdominal area and below, such as paralysis of both legs and bowel/bladder dysfunction.

