The vertebral disc in the spine is an interesting and unique structure. The discs throughout the spine have three primary functions:
- They act as a shock absorbers in the spine, positioned between each bony vertebra.
- They act as supporting structures that hold the vertebrae of the spine together.
- They are cartilaginous joints that allow for slight mobility in the spine.
In This Article:
There are a total of 23 vertebral discs in the spinal column. Specific problems with any of these discs may prompt unique symptoms, including pain that originates in the disc itself and/or pain that is related to the disc pressing on a nearby nerve.
Anatomy of a Spinal Disc
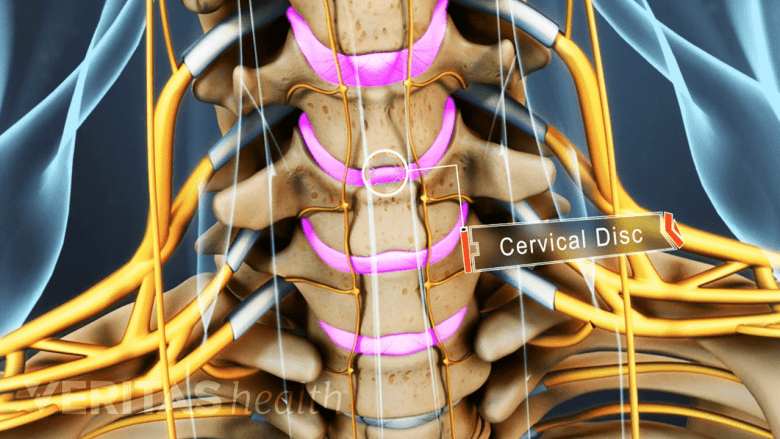
If the annulus fibrosus tears, the nucleus pulposus may leak out.
Discs are actually composed of two parts: a tough outer portion and a soft inner core, and the configuration has been likened to that of a jelly doughnut.
- Annulus fibrosus. The annulus fibrosus is outer portion of the disc. It forms the tough circular exterior and is composed of concentric sheets of collagen fibers (lamellae) that surround the inner core.
- Nucleus Pulposus. The nucleus pulposus is the inner core of the disc. It contains a loose network of fibers that are suspended in a mucoprotein gel.
The fibers of the annulus fibrosus hydraulically seal the gelatinous nucleus and evenly distribute pressure and force imposed on the structure.
The outer portion and inner core of the spinal disc fit together like two concentric cylinders. The outer portion of the disc has cartilagenous end-plates that firmly attach the disc to the vertebrae above and below.
At birth, approximately 80 percent of the disc is composed of water. In order for the disc to function properly, it must be well hydrated. The nucleus pulposus is the major carrier of the body's axial load and relies on its water-based contents to maintain strength and pliability.
Watch Lumbar Disc Anatomy Animation and Cervical Disc Anatomy Animation
Disc Degeneration
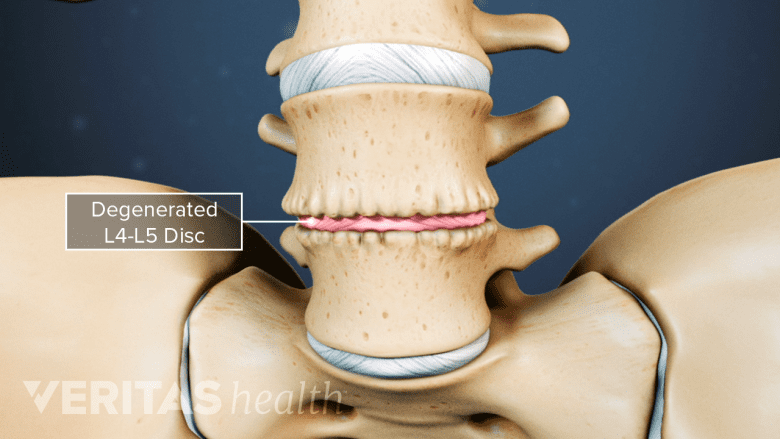
A degenerated disc can become painful.
Over time, spinal discs dehydrate and become stiffer, causing the disc to be less able to adjust to compression. While this is a natural aging process, as the disc degenerates in some individuals, it can become painful.
The most likely reason for this pain is that the degeneration can produce micromotion instability and the inflammatory proteins (the soft inner core of the disc) probably leak out of the disc space and inflame the various nerves and nerve fibers in and around the disc. Sometimes, a twisting injury damages the disc and starts a cascade of events that leads to degeneration.
The spinal disc itself has no blood supply. Without a blood supply, the disc does not have a way to repair itself, and pain created by the damaged disc can last for years.

