Similar to outpatient lumbar discectomy and laminotomy, approaches to a laterally located (to the side) cervical disc herniation or foraminal narrowing utilizes the same technique. Fluoroscopic guidance minimizes the incision, and tissue-splitting techniques reduce the impact to the muscles and ligaments of the spine. Magnification techniques and specialized tools can allow for a precise removal of the offending bone, tissue, or disc.
In This Article:
- Outpatient Spine Surgery Considerations
- Lumbar Discectomy Outpatient Spine Surgery
- Outpatient Lumbar Laminectomy or Laminotomy
- Outpatient Posterior Cervical Foraminotomy and Discectomy
- Outpatient Anterior Cervical Discectomy and Fusion (ACDF)
- Outpatient Lumbar Fusion
- Pain Management After Outpatient Spine Surgery
There are some important differences that should be considered for the cervical versus the lumbar discectomy procedure.
Cervical discectomy considerations
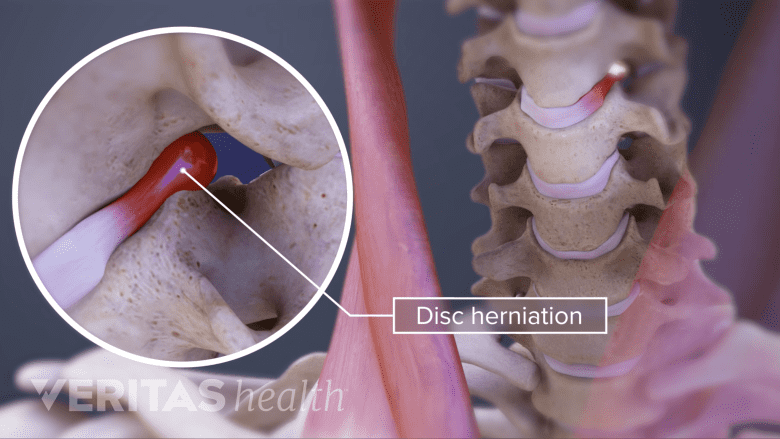
Laterally-herniated discs are an indication of discectomy.
- In the cervical spine, the disc herniation should be located to the side (laterally), or near the foramen (the gap in vertebrae in the back and to the side of the spine). With this location, there is no need for any significant retraction on the spinal cord.
- If the disc is more centrally located, meaning it has herniated toward the back of the spine and is impinging on the spinal cord, the risk associated with moving the cord away from the disc is high. Most surgeons would consider another surgical approach that allows greater visualization, rather than risk causing spinal cord injury.
Lumbar discectomy considerations
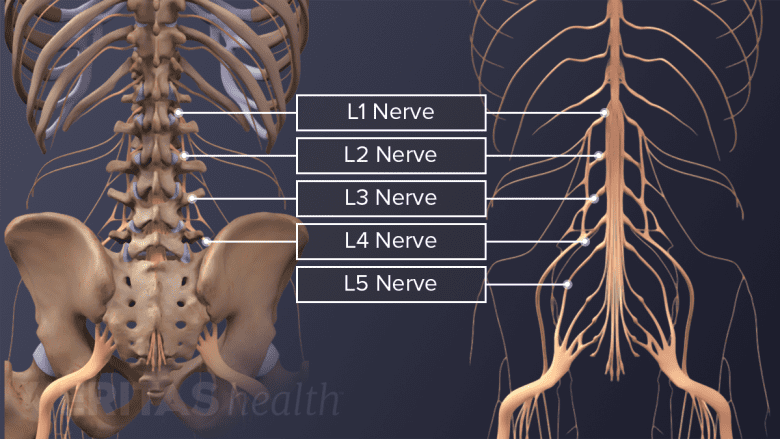
The lower end of the spinal cord branches into multiple nerves.
As the spinal cord travels down the spine, it branches out into individual nerves and exits the spinal canal, so it does not run through the lumbar spine. The branching allows individual nerves to be retracted in the lumbar spine without concern for any spinal cord damage. Therefore, for most types of disc herniations in the lumbar spine, retraction of the nerve sac is much more acceptable and tolerated in lumbar procedure.
Posterior cervical procedures may have more incision pain following surgery than occurs in the lower back. The neck muscles may be more sensitive to dissection, and it is not uncommon to need some muscle relaxers during the recovery period. Still, outpatient cervical foraminotomy/discectomy is tolerated well by most patients, and there is a high satisfaction with the procedure.

