When cervical degenerative disc disease progresses, more than just the discs are affected. As the disc loses hydration and starts to collapse, it has a reduced ability to handle axial loads and cushion the vertebrae. Other joints become more stressed and can experience degeneration, such as the uncovertebral joints (Luschka joints) located on the sides of the vertebrae, and the facet joints located at the back of the vertebrae. Other nearby structures, including ligaments, can also experience more inflammation and degeneration.
Various surgical options are available for treating symptoms of cervical degenerative disc disease. The choice typically comes down to which vertebral level(s) are affected, as well as the specific location(s) within the vertebral level(s) that are causing compression of a nerve root and/or the spinal cord.
In This Article:
- Deciding on Surgery for Cervical Degenerative Disc Disease
- Treatments to Try Before Cervical Spine Surgery
- Surgical Options for Cervical Degenerative Disc Disease
Anterior vs. Posterior Approach
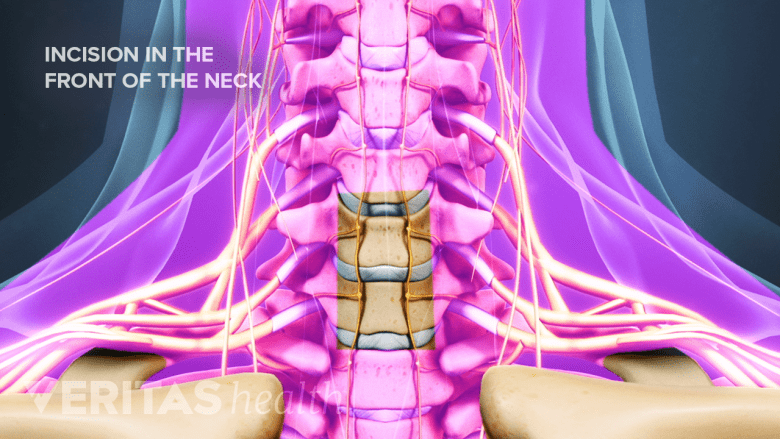
The anterior approach starts with a one- to two-inch incision in the front of the neck.
There are two general surgical approaches that can be taken to access the cervical spine:
- Anterior approach through the front of the neck. Only a thin layer of muscle beneath the skin is cut and other soft tissues are gently moved to the side, such as the esophagus, trachea, and/or larynx. This approach is needed when removing an entire disc (discectomy) and/or addressing degeneration at the front of the spine. Compared to the posterior approach, the anterior approach typically involves less pain afterward but there is some risk for experiencing challenges with speaking and/or swallowing for a few days or longer while recovering. An approach that occurs more to the side may be referred to as an anterolateral approach.
- Posterior approach through the back of the neck. Thicker muscles are cut, so postoperative pain may be greater, but there is more direct access to the cervical spine because fewer soft tissues are in the way compared to an anterior approach. A posterior approach is typically needed if only part of the disc is removed (microdiscectomy) and/or when addressing degeneration that is at the back of the spine.
Some surgeries for symptoms of cervical degenerative disc disease involve both an anterior and posterior approach.
Common Surgeries for Cervical Degenerative Disc Disease
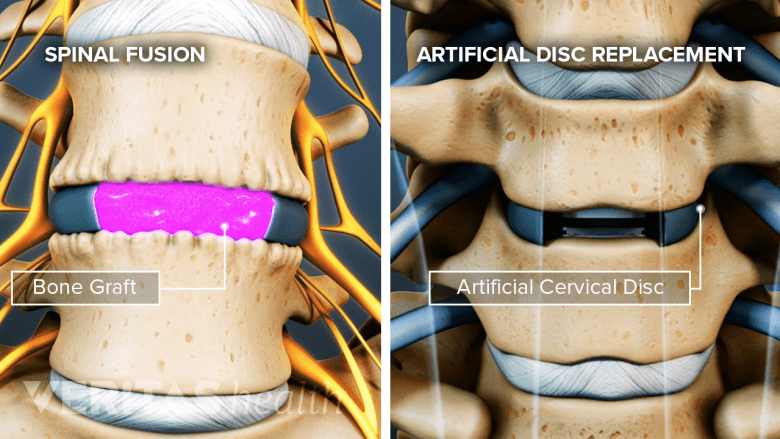
An artificial disc restores motion, and a spinal fusion eliminates motion in the spinal segment.
The two most common surgeries for cervical degenerative disc disease both involve a discectomy (removal of an intervertebral disc) but differ in how they restore that vertebral level’s disc space to its normal height:
- Anterior cervical discectomy and fusion (ACDF). After the discectomy is performed through the front of the neck, a bone graft is implanted in the space where the disc was removed. Hardware, such as a cage or plate, is also installed to hold the adjacent vertebrae in place and help facilitate the bone graft to grow and eventually fuse these two vertebrae into one solid bone. Even though the hardware is no longer needed after the bones have fused together many months later, the hardware is not removed.
- Artificial disc replacement (ADR). The disc is removed the same as in ACDF, but ADR replaces the damaged disc with an artificial disc to maintain more of the normal spinal motions rather than setting up a solid fusion.
ACDF is the more common surgery, but ADR is increasingly being performed. In cases where more than one disc needs to be removed, sometimes a hybrid surgery is performed, such as with fusion at one level and then artificial disc replacement at the level immediately above.
Less Common Surgeries
If spinal degeneration has reached the point of causing compression or inflammation of the spinal cord, a surgery that creates more space within the spinal canal may be needed. Some possibilities include:
- Anterior cervical corpectomy. An entire vertebral body is removed, along with the adjacent disc above and below. In place of the removed vertebral body, a cage and bone graft are inserted to facilitate a bone fusion. This surgery is typically only performed if compression of the spinal cord is extensive.
- Posterior cervical laminectomy. The lamina (the vertebral bone’s arch that protects the spinal cord) is removed at the degenerated vertebral level to decompress the spinal cord. Variations of this surgery include laminotomy (removing only a small part of the lamina) and laminoplasty (restructuring the lamina for more space).
- Posterior cervical foraminotomy. A small part of the bone around the foramen (the hole where the nerve root exits the spinal canal) is removed to decompress the nerve root and any other soft tissues.
Other surgical options may also be available. These surgeries may be performed on their own or in conjunction with others. For example, a foraminotomy could be done in addition to a laminectomy.
It should also be noted that while anterior cervical discectomy and fusion is the most common surgery for cervical degenerative disc disease, posterior cervical fusion surgery is also a possibility. However, posterior cervical fusion is typically done in cases where a fracture, deformity, or tumor is present, rather than for degenerative disc disease.

