Most episodes of arm pain due to a cervical herniated disc will resolve over a period of weeks to a couple of months with nonsurgical treatment and pain management. However, if the pain lasts longer than 6 to 12 weeks, or if the pain and disability are severe and unresponsive to nonsurgical treatments, spine surgery may be a reasonable option.
Watch Video: Can Herniated Discs Heal on Their Own?
The goal of surgery for a cervical herniated disc is to remove the damaged disc and ensure that the nerve root and/or spinal cord is decompressed. This procedure may alleviate radiating pain and prevent progression of neurological deficits, such as tingling, numbness, and/or weakness going into the arm.
In This Article:
Types of Surgery for a Cervical Herniated Disc
Some of the more common types of surgery for a cervical herniated disc include:
Anterior cervical discectomy and spine fusion (ACDF)

ACDF surgery is a common approach used for treating cervical herniated disc.
ACDF surgery is the most common method among spine surgeons for treating a cervical herniated disc. In this surgery, the disc is removed through a small one-inch incision in the front of the neck. After removing the disc, the disc space itself is set up for the adjacent vertebrae to eventually grow together and fuse. A plate can be added in front of the graft for added stability and possibly a better fusion success rate.
Cervical artificial disc replacement
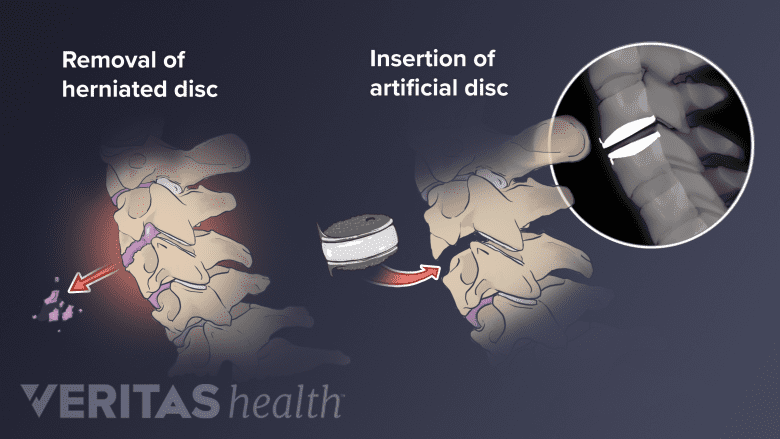
The artificial disc may replicate both the structure and function of the natural disc.
As in an ACDF surgery, an cervical artificial disc replacement surgery involves removing the affected disc through a small incision in the front of the neck. Instead of fusing the adjacent vertebrae, an artificial disc is implanted in the disc space between the adjacent vertebrae. The goal of the artificial disc is to mimic the form and function of the original disc.
Posterior cervical discectomy
This surgery is similar to a posterior (from the back) lumbar discectomy. It may be a reasonable approach for cervical discs that herniate laterally into the neural foramen (the tunnel that the nerve travels through to exit the spinal canal). This posterior approach is more difficult than an anterior approach because there are many veins in this area that can result in bleeding, and the bleeding limits visualization during the surgery. This approach also necessitates more manipulation to the spinal cord and creates a higher risk of complication.
See Posterior Cervical Decompression (Microdiscectomy) Surgery
Although any major surgery has possible risks and complications, with an experienced spine surgeon serious complications from cervical discs surgery are rare. The two most common surgeries, ACDF and artificial disc replacement, are both considered reliable surgeries with favorable outcomes in terms of reducing radiating pain and tingling stemming from a compressed nerve root.
See Anterior Cervical Discectomy and Fusion Complications and Potential Complications and Risks of Cervical Disc Replacement Surgery
Postoperative Care and Recovery

A neck brace may be used for additional support after cervical spine surgery.
For anterior surgery on the cervical spine, such as an ACDF or artificial disc replacement, the recovery tends to be quicker and less painful than posterior procedures. An anterior surgery is done through a small incision in the front of the neck rather than cutting through thicker muscles in the back of the neck. As such, the patient can usually go home the same day or after a one-night stay in the hospital after an anterior surgery. The hospital stay after posterior cervical spine surgery may be a few days longer.
See ACDF Surgery Postoperative Care
If arm pain was present before surgery, it typically goes away fairly quickly after the procedure. Neck pain may take longer to abate, especially in or near the area where the procedure was performed. Any numbness or weakness in the arm may take weeks, months, or longer. Depending on the severity of the nerve root injury caused by the herniated disc, some arm pain, weakness, and/or numbness may remain permanently after the surgery.
Postoperatively, most spine surgeons prescribe a neck brace, although the type of brace and length of usage is variable. Also, most spine surgeons will ask their patients to limit their activities postoperatively, although the amount of restrictions and the length of time tend to vary. Ask your spine surgeon before the surgery what his or her usual protocol is regarding postoperative care.
Editor’s Top Picks
- ACDF: Anterior Cervical Discectomy and Fusion
- Cervical Disc Replacement Surgery Video
- Surgical Options for Cervical Radiculopathy from a Herniated Cervical Disc
- Surgical Procedure for Cervical Disc Replacement
- Anterior Cervical Discectomy and Fusion Complications
- Cervical Herniated Disc Treatment Animation

