Every extra pound of weight adds strain to the muscles and ligaments of the back. To compensate for extra weight, the spine tends to become tilted and stressed unevenly. Excess stomach weight typically pulls the pelvis forward (increasing lumbar lordosis), leading to aggravated lower back pain.
In This Article:
- Weight Loss for Back Pain Relief
- Weight Loss and Exercise for Patients
- Nutrition and Diet for Weight Loss
Obesity Leads to Back Pain
Obesity is associated with an increased risk of back pain. Excess weight also tends to prolong the recovery period after episodes of back pain.1Ibrahimi-Kaçuri D, Murtezani A, Rrecaj S, Martinaj M, Haxhiu B. Low back pain and obesity. Med Arch. 2015;69(2):114-116. doi:10.5455/medarh.2015.69.114-116
Persons who are obese and/or have a high percentage of body fat are:
- 33% more likely to experience low back pain2Deere KC, Clinch J, Holliday K, et al. Obesity is a risk factor for musculoskeletal pain in adolescents: findings from a population-based cohort. Pain. 2012;153(9):1932-1938. doi:10.1016/j.pain.2012.06.006
- 35% more likely to experience severe, intense pain2Deere KC, Clinch J, Holliday K, et al. Obesity is a risk factor for musculoskeletal pain in adolescents: findings from a population-based cohort. Pain. 2012;153(9):1932-1938. doi:10.1016/j.pain.2012.06.006
- Up to 43% more likely to develop chronic low back pain3Shiri R, Karppinen J, Leino-Arjas P, Solovieva S, Viikari-Juntura E. The association between obesity and low back pain: a meta-analysis. Am J Epidemiol. 2010;171(2):135-154. doi:10.1093/aje/kwp356,4Zhang TT, Liu Z, Liu YL, Zhao JJ, Liu DW, Tian QB. Obesity as a Risk Factor for Low Back Pain: A Meta-Analysis. Clin Spine Surg. 2018;31(1):22-27. doi:10.1097/BSD.0000000000000468
- For men, up to 50% more likely to experience disability and functional limitations5Davison KK, Ford ES, Cogswell ME, Dietz WH. Percentage of body fat and body mass index are associated with mobility limitations in people aged 70 and older from NHANES III. J Am Geriatr Soc. 2002;50(11):1802-1809. doi:10.1046/j.1532-5415.2002.50508.x
- For women, about 100% more likely to experience disability and functional limitations6Bener A, Alwash R, Gaber T, Lovasz G. Obesity and low back pain. Coll Antropol. 2003;27(1):95-104.
Back pain has a strong association with body mass index (BMI),6Bener A, Alwash R, Gaber T, Lovasz G. Obesity and low back pain. Coll Antropol. 2003;27(1):95-104. a mathematical formula (BMI=kg/m2) that considers one’s weight in kilograms related to height in meters. On the index, a score between 18.5 and 24.9 is considered normal, between 25 and 29.9 is considered overweight, and above 30 is considered obese.
In addition to BMI, it is also important to assess where the excess fat is stored on the body, such as around the waist or in the legs.
Notable Symptoms of Back Pain Connected to Excess Weight
Obese individuals with back pain often have more severe leg or knee pain.
Individuals who are obese or severely overweight and have back pain tend to exhibit one or more of the following symptoms:
- Fatigue during short periods of exercise
- Difficulty breathing or shortness of breath
- Pain in the leg or knee that is more severe than pain in the back
- Increase in pain with back extension7Rampersaud YR, Bidos A, Fanti C, Perruccio AV. The Need for Multidimensional Stratification of Chronic Low Back Pain (LBP). Spine (Phila Pa 1976). 2017;42(22):E1318-E1325. doi:10.1097/BRS.0000000000002237 (bending backward)
Back pain is more likely to become a chronic, ongoing condition if leg and back pain increase with extension.3Shiri R, Karppinen J, Leino-Arjas P, Solovieva S, Viikari-Juntura E. The association between obesity and low back pain: a meta-analysis. Am J Epidemiol. 2010;171(2):135-154. doi:10.1093/aje/kwp356 These symptoms make exercise challenging, but not impossible.
Types of Back Pain Related to Obesity
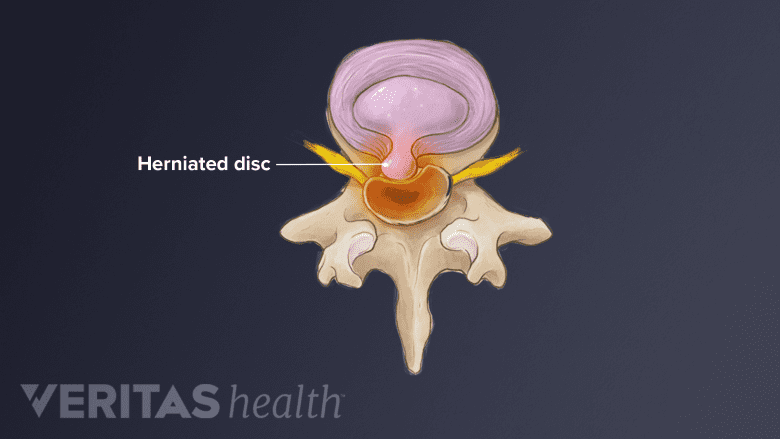
An increased body weight raises the likelihood of developing a herniated disc.
Higher body weight increases the likelihood of developing several serious health conditions, such as type 2 diabetes, high blood pressure, and heart disease. Obesity is also related to conditions that specifically affect the spine and lower back, namely:
- Herniated discs. Obese or overweight patients are considered more likely to experience a herniated disc, a common cause of leg pain or sciatica due to a lumbar radiculopathy. The disc is more likely to herniate as it is forced to compensate for the pressure of extra weight on the back.8Heliövaara M. Body height, obesity, and risk of herniated lumbar intervertebral disc. Spine (Phila Pa 1976). 1987;12(5):469-472. doi:10.1097/00007632-198706000-00009
- Osteoarthritis. Extra body weight strains joints in the spine and leads to an increased risk of developing spinal osteoarthritis. A BMI greater than 25 increases the risk of developing osteoarthritis.9King LK, March L, Anandacoomarasamy A. Obesity & osteoarthritis. Indian J Med Res. 2013;138(2):185-193.
On occasion, degenerative spinal conditions may need to be treated with surgery. Obesity has been associated with a greater risk of complication or infection in individuals who require surgery.10McGuire KJ, Khaleel MA, Rihn JA, Lurie JD, Zhao W, Weinstein JN. The effect of high obesity on outcomes of treatment for lumbar spinal conditions: subgroup analysis of the spine patient outcomes research trial. Spine (Phila Pa 1976). 2014;39(23):1975-1980. doi:10.1097/BRS.0000000000000577 Surgery typically remains worthwhile when medically indicated.8Heliövaara M. Body height, obesity, and risk of herniated lumbar intervertebral disc. Spine (Phila Pa 1976). 1987;12(5):469-472. doi:10.1097/00007632-198706000-00009,11Jain D, Berven S. Effect of Obesity on the Development, Management, and Outcomes of Spinal Disorders. J Am Acad Orthop Surg. 2019;27(11):e499-e506. doi:10.5435/JAAOS-D-17-00837 Weight loss before undergoing back surgery may help improve the postsurgical healing process.
Read more about Lumbar Spine Surgery
Ways to Reduce Weight for Back Pain Relief
Methods of weight loss have been studied for their ability to relieve pain. Active programs have fared far better than passive advice, information, or lifestyle coaching. It is important for individuals who have back pain and are overweight or obese to take action and change daily habits for long-lasting results.
The most recommended ways (tier 1 and tier 2 weight management services12Jennings A, Hughes CA, Kumaravel B, et al. Evaluation of a multidisciplinary Tier 3 weight management service for adults with morbid obesity, or obesity and comorbidities, based in primary care. Clin Obes. 2014;4(5):254-266. doi:10.1111/cob.12066) to lose weight include:
- A healthy diet
- Frequent, moderate to high-intensity exercise
- Counseling with a professional to achieve behavioral changes13Armstrong MJ, Mottershead TA, Ronksley PE, Sigal RJ, Campbell TS, Hemmelgarn BR. Motivational interviewing to improve weight loss in overweight and/or obese patients: a systematic review and meta-analysis of randomized controlled trials. Obes Rev. 2011;12(9):709-723. doi:10.1111/j.1467-789X.2011.00892.x
Avoiding physical activity due to fatigue and shortness of breath weakens the back further, and indirectly leads to more intense back pain. Fear of pain with movement (kinesiophobia) is a mediating factor between intense pain and limited ability to perform daily tasks.14Varallo G, Scarpina F, Giusti EM, et al. Does Kinesiophobia Mediate the Relationship between Pain Intensity and Disability in Individuals with Chronic Low-Back Pain and Obesity?. Brain Sci. 2021;11(6):684. Published 2021 May 22. doi:10.3390/brainsci11060684 For some, overcoming the fear of physical activity is an important step to losing weight and relieving pain.
Alternative ways (tier 3 weight management services) to lose weight include:
- A low-energy liquid diet, which is best followed under medical supervision10McGuire KJ, Khaleel MA, Rihn JA, Lurie JD, Zhao W, Weinstein JN. The effect of high obesity on outcomes of treatment for lumbar spinal conditions: subgroup analysis of the spine patient outcomes research trial. Spine (Phila Pa 1976). 2014;39(23):1975-1980. doi:10.1097/BRS.0000000000000577
- Prescription medications, such as orlistat (Xenical), which may lead to serious liver injury10McGuire KJ, Khaleel MA, Rihn JA, Lurie JD, Zhao W, Weinstein JN. The effect of high obesity on outcomes of treatment for lumbar spinal conditions: subgroup analysis of the spine patient outcomes research trial. Spine (Phila Pa 1976). 2014;39(23):1975-1980. doi:10.1097/BRS.0000000000000577
- Leptin therapy, which are hormone injections that help prevent the body from regaining lost weight10McGuire KJ, Khaleel MA, Rihn JA, Lurie JD, Zhao W, Weinstein JN. The effect of high obesity on outcomes of treatment for lumbar spinal conditions: subgroup analysis of the spine patient outcomes research trial. Spine (Phila Pa 1976). 2014;39(23):1975-1980. doi:10.1097/BRS.0000000000000577
Tier 4 weight management involves bariatric surgery, which reduces the severity of back pain and disability scores and increases the quality of life.15Stefanova I, Currie AC, Newton RC, et al. A Meta-analysis of the Impact of Bariatric Surgery on Back Pain. Obes Surg. 2020;30(8):3201-3207. doi:10.1007/s11695-020-04713-y
Bariatric surgery is usually considered for individuals whose body mass index is above 35 to 40, if safer and healthier methods of weight loss have not proven effective over 6 to 12 months. Bariatric surgery poses numerous short-term and long-term risks, such as bleeding of the digestive tract, bowel obstruction, nutritional deficiencies, hernia, a venous blood clot that moves into the lungs (venous thromboembolism), reoperation, and rarely, death.16Arterburn DE, Telem DA, Kushner RF, Courcoulas AP. Benefits and Risks of Bariatric Surgery in Adults: A Review. JAMA. 2020;324(9):879-887. doi:10.1001/jama.2020.12567
Bariatric surgery can only do so much to help an individual lose weight and to help curb food cravings. It is important that bariatric surgery is combined with a nutritional program and regular exercise. The patient has to be highly motivated to not only lose weight but also to keep the weight off.
- 1 Ibrahimi-Kaçuri D, Murtezani A, Rrecaj S, Martinaj M, Haxhiu B. Low back pain and obesity. Med Arch. 2015;69(2):114-116. doi:10.5455/medarh.2015.69.114-116
- 2 Deere KC, Clinch J, Holliday K, et al. Obesity is a risk factor for musculoskeletal pain in adolescents: findings from a population-based cohort. Pain. 2012;153(9):1932-1938. doi:10.1016/j.pain.2012.06.006
- 3 Shiri R, Karppinen J, Leino-Arjas P, Solovieva S, Viikari-Juntura E. The association between obesity and low back pain: a meta-analysis. Am J Epidemiol. 2010;171(2):135-154. doi:10.1093/aje/kwp356
- 4 Zhang TT, Liu Z, Liu YL, Zhao JJ, Liu DW, Tian QB. Obesity as a Risk Factor for Low Back Pain: A Meta-Analysis. Clin Spine Surg. 2018;31(1):22-27. doi:10.1097/BSD.0000000000000468
- 5 Davison KK, Ford ES, Cogswell ME, Dietz WH. Percentage of body fat and body mass index are associated with mobility limitations in people aged 70 and older from NHANES III. J Am Geriatr Soc. 2002;50(11):1802-1809. doi:10.1046/j.1532-5415.2002.50508.x
- 6 Bener A, Alwash R, Gaber T, Lovasz G. Obesity and low back pain. Coll Antropol. 2003;27(1):95-104.
- 7 Rampersaud YR, Bidos A, Fanti C, Perruccio AV. The Need for Multidimensional Stratification of Chronic Low Back Pain (LBP). Spine (Phila Pa 1976). 2017;42(22):E1318-E1325. doi:10.1097/BRS.0000000000002237
- 8 Heliövaara M. Body height, obesity, and risk of herniated lumbar intervertebral disc. Spine (Phila Pa 1976). 1987;12(5):469-472. doi:10.1097/00007632-198706000-00009
- 9 King LK, March L, Anandacoomarasamy A. Obesity & osteoarthritis. Indian J Med Res. 2013;138(2):185-193.
- 10 McGuire KJ, Khaleel MA, Rihn JA, Lurie JD, Zhao W, Weinstein JN. The effect of high obesity on outcomes of treatment for lumbar spinal conditions: subgroup analysis of the spine patient outcomes research trial. Spine (Phila Pa 1976). 2014;39(23):1975-1980. doi:10.1097/BRS.0000000000000577
- 11 Jain D, Berven S. Effect of Obesity on the Development, Management, and Outcomes of Spinal Disorders. J Am Acad Orthop Surg. 2019;27(11):e499-e506. doi:10.5435/JAAOS-D-17-00837
- 12 Jennings A, Hughes CA, Kumaravel B, et al. Evaluation of a multidisciplinary Tier 3 weight management service for adults with morbid obesity, or obesity and comorbidities, based in primary care. Clin Obes. 2014;4(5):254-266. doi:10.1111/cob.12066
- 13 Armstrong MJ, Mottershead TA, Ronksley PE, Sigal RJ, Campbell TS, Hemmelgarn BR. Motivational interviewing to improve weight loss in overweight and/or obese patients: a systematic review and meta-analysis of randomized controlled trials. Obes Rev. 2011;12(9):709-723. doi:10.1111/j.1467-789X.2011.00892.x
- 14 Varallo G, Scarpina F, Giusti EM, et al. Does Kinesiophobia Mediate the Relationship between Pain Intensity and Disability in Individuals with Chronic Low-Back Pain and Obesity?. Brain Sci. 2021;11(6):684. Published 2021 May 22. doi:10.3390/brainsci11060684
- 15 Stefanova I, Currie AC, Newton RC, et al. A Meta-analysis of the Impact of Bariatric Surgery on Back Pain. Obes Surg. 2020;30(8):3201-3207. doi:10.1007/s11695-020-04713-y
- 16 Arterburn DE, Telem DA, Kushner RF, Courcoulas AP. Benefits and Risks of Bariatric Surgery in Adults: A Review. JAMA. 2020;324(9):879-887. doi:10.1001/jama.2020.12567

