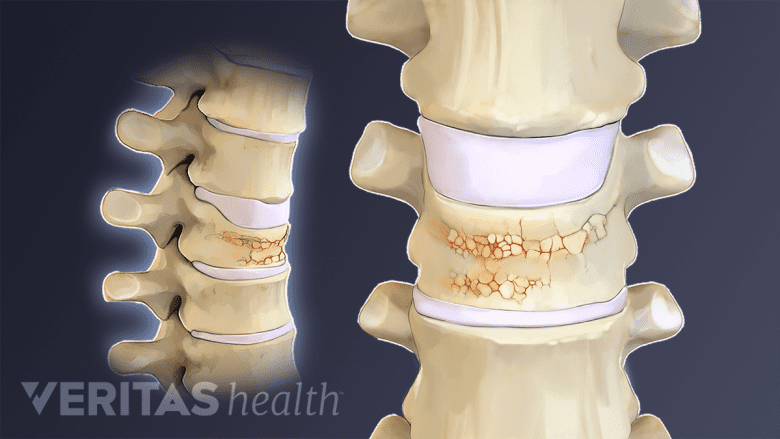
In some cases of osteoporosis, one or more vertebral bones can become so weak that they cannot fully support their load and develop tiny cracks. This type of fracture, called a vertebral compression fracture, can be painful and sometimes leads to worsening symptoms, such as tingling, numbness, weakness, or spinal deformity (kyphosis). Fortunately, you can take steps to lower your risk for vertebral compression fractures, as well as seek treatment if one occurs.
Visit your doctor regularly
If you’re dealing with a chronic condition, such as osteoporosis, it’s especially important to have regular checkups to monitor how you’re doing and whether the treatment plan needs to be adjusted. For example, your doctor might recommend certain medications for osteoporosis, such as bisphosphonates, which may reduce the risk for a vertebral compression fracture.1Byun JH, Jan S, Lee S, et al. The efficacy of bisphosphonates for prevention of osteoporotic fracture: an update meta-analysis. J Bone Metab. 2017; 24(1):37-49.
Eat healthy and quit bad habits
Everyone needs to get plenty of calcium for bone health. If you have osteoporosis or low bone mass, your doctor might also recommend calcium supplements. In addition, it is important to get plenty of vitamin D, which helps the body absorb calcium into the bones.
If you smoke, try to quit. Smoking is known to weaken bones and can worsen osteoporosis.
Regularly drinking lots of soda and/or alcohol may also contribute to weaker bones. If you are in the habit of drinking soda or alcohol every day, try to quit or cut back.
Consult with your doctor to find a balanced diet that works best for you. While it’s important to get enough calcium for bone health, too much calcium can also potentially cause problems, such as kidney stones.
Stay active but use good judgment
The phrase “use it or lose it” is especially true when it comes to your bones. Weight-bearing activities help to build and maintain bone mass. On the other hand, being inactive allows the bones to thin and weaken.
In general, it is good for people to stay active and exercise regularly. If you’ve been diagnosed with osteoporosis or low bone mass, check with your doctor regarding which activities may or may not be right for you. A supervised physical therapy program that focuses on safe resistance exercises may be recommended to help build muscle strength and bone density. Research continues to show that resistance training can strengthen both muscles and bones, even in older people, which may also lower the risk for osteoporotic fractures.2Huovinen V, Ivaska KK, Kiviranta R. Bone mineral density is increased after a 16-week resistance training intervention in elderly women with decreased muscle strength. Eur J Endocrinol. 2016; 175(6):571-582.
See How a Physical Therapist Can Help with Exercise
Most people with osteoporosis are encouraged to do some form of weight-bearing exercise as a way to better maintain bone mass, but some activities may be discouraged. For example, your doctor might advise against heavy lifting, doing sit-ups, or bending over to touch the toes, which could put undue stress on the spine.
Don’t ignore a compression fracture
Any time you have back pain that lasts more than a week or two, it is important to see the doctor. Ignoring back pain and potential vertebral compression fractures may lead to bigger problems down the road, such as increased pain, tingling, numbness, weakness, and severe spinal deformity.
See Vertebral Fracture Symptoms
Most vertebral compression fractures are treated nonsurgically, such as with rest, pain medications, or applying ice and/or heat while the fracture eventually heals on its own. If the pain cannot be successfully managed with nonsurgical treatments, surgery may be considered. A couple of surgical options for vertebral compression fractures include:
Vertebroplasty. This minimally-invasive procedure involves carefully placing a needle through the back and into the compression fracture, delivering bone cement to fill the cracks and re-stabilize the vertebra.
Kyphoplasty. This procedure is similar to vertebroplasty, except that a small balloon is inserted and expanded into the compression fracture to help restore the collapsed vertebra closer to its original height before injecting the bone cement.
Some studies have found that both vertebroplasty and kyphoplasty have been effective at reducing pain from vertebral compression fractures, especially when done within 2 months of sustaining the fracture.3Takahashi S, Hoshino M, Terai H et al. Differences in short-term clinical and radiological outcomes depending on timing of balloon kyphoplasty for painful osteoporotic vertebral fracture. Journal of Orthopaedic Science. 2018; 23(1):51-6.
By following these tips, you’re well on your way to protecting your spine and successfully managing osteoporosis.
Learn more:
- 1 Byun JH, Jan S, Lee S, et al. The efficacy of bisphosphonates for prevention of osteoporotic fracture: an update meta-analysis. J Bone Metab. 2017; 24(1):37-49.
- 2 Huovinen V, Ivaska KK, Kiviranta R. Bone mineral density is increased after a 16-week resistance training intervention in elderly women with decreased muscle strength. Eur J Endocrinol. 2016; 175(6):571-582.
- 3 Takahashi S, Hoshino M, Terai H et al. Differences in short-term clinical and radiological outcomes depending on timing of balloon kyphoplasty for painful osteoporotic vertebral fracture. Journal of Orthopaedic Science. 2018; 23(1):51-6.

