By the time ankylosing spondylitis starts causing neck pain and stiffness, the same symptoms are likely already present in the lower back. Ankylosing spondylitis almost always starts in the lower back (lumbar spine) and sacroiliac joints many months or years before reaching the neck (cervical spine).
Even though symptoms typically start lower in the spine, many people start experiencing neck pain from ankylosing spondylitis before receiving a diagnosis for the condition.
In This Article:
- Neck Pain from Ankylosing Spondylitis
- Diagnosis of Neck Pain from Ankylosing Spondylitis
- Treatment of Neck Pain from Ankylosing Spondylitis
- Medications for Neck Pain Caused by Ankylosing Spondylitis
- Ankylosing Spondylitis Video
Diagnosing Ankylosing Spondylitis
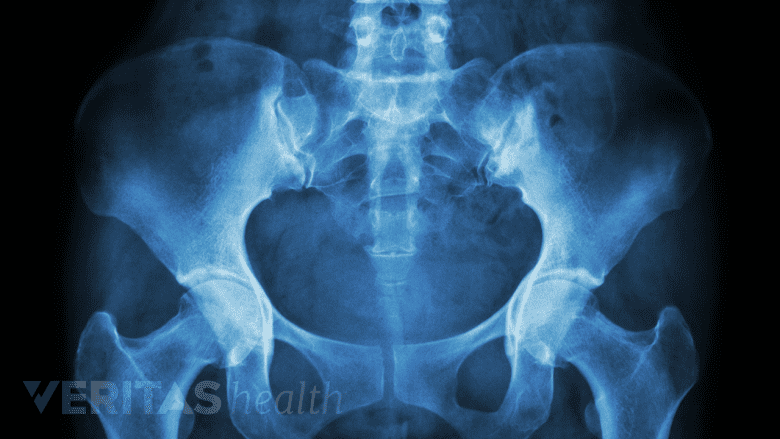
An x-ray showing inflammation in the sacroiliac joints is important for diagnosing ankylosing spondylitis.
There is no single test or symptom that can officially diagnose ankylosing spondylitis. Instead, it is diagnosed by following a process of gathering evidence that increasingly points to ankylosing spondylitis while ruling out other conditions.
This diagnostic process typically involves four general steps:
- Patient history. Information is collected in the doctor’s office regarding overall medical history, current symptoms, and lifestyle, such as activity levels and dietary habits.
- Physical exam. The patient’s posture is observed for any abnormalities suggesting spinal degeneration, such as if the head cannot reach the wall while standing with the back against the wall. In addition, the physician may palpate (touch) the neck and back along the spine for areas of tenderness or tightness, and the rib cage and spine’s range of motion is examined for any signs of reduced mobility.
- Imaging studies. An xray image that shows in the sacroiliac joint(connecting lower spine and pelvis) has traditionally been a key factor in diagnosing ankylosing spondylitis. However, sometimes an x-ray cannot pick up these changes in the sacroiliac joint until years after the symptoms have started. Other methods to view the spine may catch changes from ankylosing spondylitis sooner—such as MRI or CT scans—but they are also more expensive.
- Blood tests. These tests can screen for inflammatory markers and genetic risk factors, which could indicate a higher likelihood of having ankylosing spondylitis. For example, most people with ankylosing spondylitis carry a gene called HLA-B27, so detecting it can be helpful to confirm a diagnosis when symptoms are already present.1Overview of ankylosing spondylitis. Spondylitis Association of America web site. Published June 2016. Accessed January 29, 2018.
Read more about Ankylosing Spondylitis Diagnosis on Arthritis-health.com
Delayed Diagnosis of Ankylosing Spondylitis
Many people with ankylosing spondylitis do not receive a diagnosis within the first few years of onset, possibly because initial symptoms may be relatively manageable and a lack of family history for the condition makes it harder to diagnose.2Dincer U, Cakar E, Kiralp MZ, Dursun H. Diagnosis delay in patients with ankylosing spondylitis: possible reasons and proposals for new diagnostic criteria. Clin Rheumatol. 2008; 27(4): 457-62. However, having ankylosing spondylitis diagnosed sooner rather than later may slow progression of the disease.3Haroon N, Inman RD, Learch TJ, et a. The impact of TNF-inhibitors on radiographic progression in ankylosing spondylitis. Arthritis Rheum. 2013; 65(10):2645-54.
- 1 Overview of ankylosing spondylitis. Spondylitis Association of America web site. Published June 2016. Accessed January 29, 2018.
- 2 Dincer U, Cakar E, Kiralp MZ, Dursun H. Diagnosis delay in patients with ankylosing spondylitis: possible reasons and proposals for new diagnostic criteria. Clin Rheumatol. 2008; 27(4): 457-62.
- 3 Haroon N, Inman RD, Learch TJ, et a. The impact of TNF-inhibitors on radiographic progression in ankylosing spondylitis. Arthritis Rheum. 2013; 65(10):2645-54.

