Thoracic outlet syndrome is a painful condition that results from compression of the nerves and/or blood vessels running through the thoracic outlet (area between the top rib and collarbone). The symptoms are typically felt in the shoulder and arm, but sometimes can also be felt in the neck.
Common causes of thoracic outlet syndrome include:
- Traumatic injury. A major collision or fall could lead to internal changes that place more pressure on the thoracic outlet’s nerves and/or blood vessels.
- Repetitive motions. Participating in sports that involve repetitive shoulder movements—such as baseball, volleyball, or swimming. Similarly, daily tasks or work that involve reaching up above the head, such as work done by painters and construction workers, tends to increase the risk.
- Poor posture. If poor posture leads to the head drifting forward and shoulders rounding forward additional pressure tends to be put on nerves and/or blood vessels traveling through the thoracic outlet, and increases susceptibility to developing the symptoms.
See How Poor Posture Causes Neck Pain
Numerous other causes of thoracic outlet syndrome exist, and sometimes the cause is unknown. When thoracic outlet syndrome is accurately diagnosed and treated, the long-term outlook tends to be good.
In This Article:
- Little-Known Causes of Neck Pain
- Neck Pain from Fibromyalgia
- Neck Pain from Thoracic Outlet Syndrome
- Neck Pain from Lyme Disease
- Neck Pain from Crowned Dens Syndrome
- Neck Pain from Eagle Syndrome
Common Symptoms
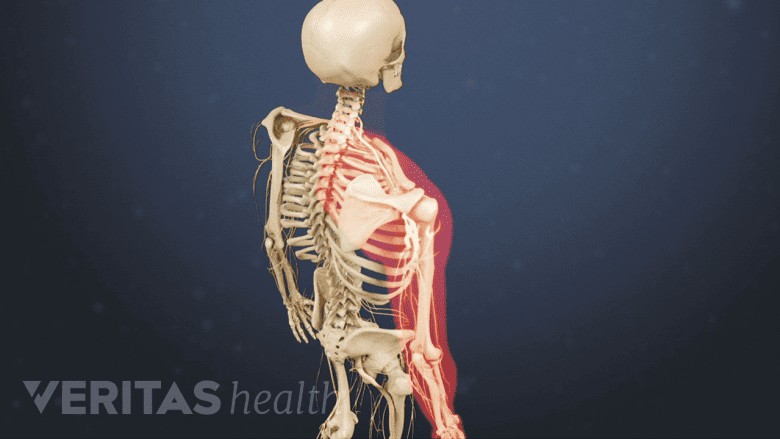
Thoracic outlet syndrome causes numbness and tingling in the shoulder, arm, and hand.
Thoracic outlet syndrome can cause several or all of the following symptoms:
- Pain felt in the hand, arm, shoulder, and/or neck, which can range anywhere from dull to sharp
- Weakened hand and/or arm that is easily fatigued
- Numbness and/or tingling felt in the shoulder, arm, and/or hand
- Swelling in the arm and hand
- Difficulty with working above the head as it exacerbates the symptoms
Numerous other thoracic outlet syndrome symptoms are possible.
Why Thoracic Outlet Syndrome Causes Neck Symptoms

In thoracic outlet syndrome, nerve compression can cause pins-and-needles tingling or numbness.
The neck symptoms from thoracic outlet syndrome can depend on whether blood vessels or nerves are being compressed. If nerves are compressed, they are more likely to feel like a pins-and-needles tingling or numbness. If blood vessels are compressed, the neck pain could feel more intense heat or cold due to poor circulation—especially when trying to sleep.
Diagnosis

Electromyography monitors muscle and nerve function by tracking electrical activity in muscles.
Thoracic outlet syndrome can mimic many other conditions, so it is important to receive a thorough examination before an accurate diagnosis can be made. Diagnosing thoracic outlet syndrome usually involves:
- Patient history. A medical professional will ask about the patient’s medical history, including when and how current symptoms may have started.
- Physical exam. Patient is examined for any signs of possible thoracic outlet syndrome, such as reduced muscle tone in the thumb or swelling in the arm. Provocative tests may be done to see if symptoms can be recreated, such as making fists while holding the arms above the head for a few minutes to see if the pain occurs.
- Imaging and diagnostic tests. Depending on whether nerve or blood vessel compression is suspected, various forms of imaging and diagnostic tests may be ordered. For example, an MRI, CT scan, or ultrasound could be useful for examining if (and where) nerve or blood vessels might be compressed. Also, nerve conduction studies can test how well electrical signals are being transferred through nerves, and an electromyography (EMG) can test electrical signals through muscles, which can also pinpoint potential problem spots.
If a combination of the physical exam and diagnostic tests suggest thoracic outlet syndrome, and other causes have been ruled out, the diagnosis is made and treatment can begin accordingly.
Treatment
Nonsurgical treatments are tried first, such as medications for pain relief and a physical therapy program to strengthen muscles and improve range of motion in the arm, shoulder, and/or neck.
If nonsurgical treatments do not provide relief or if the health of a nerve or blood vessel is at risk, surgery may be advised. Various types of surgery are possible and will depend on the location of the compression, as well as what is being compressed.

