Neck spasms are commonly accompanied by muscle tightness, pain that ranges between achy or sharp, and/or neck stiffness. While most neck spasms go away on their own, sometimes they linger and the underlying cause must be diagnosed and treated.
In This Article:
- Understanding Neck Spasms
- What Causes Neck Spasms?
- Neck Spasms Animation
Potential Neck Spasm Causes
The underlying cause of a neck spasm may be:
Neck strain or sprain
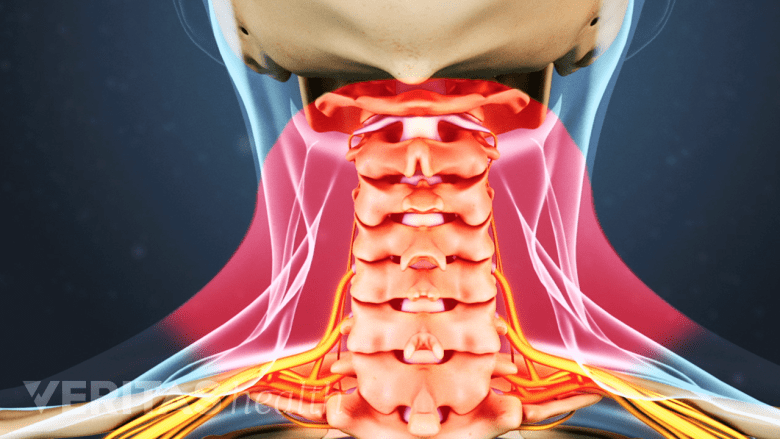
Neck muscle may tighten or spasm to protect against overextension from a minor tear or strain.
A small tear or strain in a neck muscle can cause it to tighten and/or spasm as a protective mechanism against stretching too far. An injury or sprain to a nearby ligament may cause a reflex muscle spasm where the non-injured muscle tightens in order to protect the nearby injured ligament.
Overexertion or fatigue
When a muscle is overworked, it is at increased risk for developing pain and going into spasm. Some evidence suggests that muscles worked in high-temperature environments are also at an increased risk for muscle spasms.1Cooper ER, Ferrara MS, Broglio SP. Exertional heat illness and environmental conditions during a single football season in the southeast. J Athl Train. 2006; 41(3):332-6.
Herniated disc

A herniated neck disc can induce spasms due to nerve irritation and inflammation.
If an intervertebral disc herniates in the cervical spine and starts leaking inflammatory proteins, nearby muscles in the neck can become inflamed and painful, causing them to spasm.
Facet joint osteoarthritis

Increased facet joint friction may cause neck pain and spasm.
When the facet joint’s protective cartilage starts wearing away, the adjacent vertebrae start grinding against each other. Bone spurs (osteophytes) can grow in an attempt to stabilize the joint, which increases inflammation and the risk for nerve compression, both of which may contribute to neck spasms.
See Cervical Osteoarthritis (Neck Arthritis)
Mechanical dysfunction
Any type of mechanical dysfunction that prevents the joint from going through its normal range of motion can increase the likelihood for muscle spasms. This type of joint dysfunction can have many causes, such as bone spurs, injury, poor posture, or congenital abnormalities from birth.
Peripheral neuropathy

Peripheral neuropathy can lead to sensory and motor problems, including muscle spasms.
Nerves that branch outside of the spinal canal and feed into the various parts of the body are called peripheral nerves. If a peripheral nerve in the neck becomes damaged—such as from disease or a lesion—it may malfunction by sending too many signals, altered signals, or fewer/no signals. Peripheral neuropathy can potentially lead to various problems with sensory, reflex, and motor functions, including muscle spasms.2Peripheral Neuropathy Fact Sheet. National Institutes of Health, National Institute of Neurological Disorders and Stroke. https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Peripheral-Neuropathy-Fact-Sheet. Accessed March 18, 2019.
See Understanding Neuropathy Symptoms
Myofascial pain syndrome

Myofascial pain syndrome can cause neck spasms and referred pain from trigger points in muscles.
This chronic condition occurs when painful trigger points develop within the muscles and/or their connective tissues (fascia). When this condition occurs, muscles in or near the neck are commonly affected. The muscles can become tight and spasm, and pain may increase and spread up into the head or further down the shoulder, arm, and/or upper back when a trigger point in the neck is touched.
Stress or anxiety
The physiological effects of emotional stress and anxiety have been linked to neck muscle tension and pain, which can also include spasms.
Cervical dystonia
This rare and painful disorder, also called spasmodic torticollis, involves the neck involuntarily rotating to the side and/or tilting. It can occur at any age but is more likely to develop after age 40.3Cervical Dystonia. National Organization of Rare Disorders (NORD). https://rarediseases.org/rare-diseases/cervical-dystonia. Accessed March 26, 2019. The cause of cervical dystonia is not fully understood, but there may be a genetic component as it tends to run in families. Other causes have also been suspected, such as a brain injury.
Other causes of a neck spasm are possible. Sometimes the cause of a neck spasm is not known, in which case it is considered an idiopathic muscle spasm.
If a neck spasm keeps recurring or causes enough pain or stiffness to interfere with daily activities, it is advised to visit a doctor for further evaluation.
- 1 Cooper ER, Ferrara MS, Broglio SP. Exertional heat illness and environmental conditions during a single football season in the southeast. J Athl Train. 2006; 41(3):332-6.
- 2 Peripheral Neuropathy Fact Sheet. National Institutes of Health, National Institute of Neurological Disorders and Stroke. https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Peripheral-Neuropathy-Fact-Sheet. Accessed March 18, 2019.
- 3 Cervical Dystonia. National Organization of Rare Disorders (NORD). https://rarediseases.org/rare-diseases/cervical-dystonia. Accessed March 26, 2019.

