Spinal Decompression Therapy involves stretching the spine, using a traction table or similar motorized device, with the goal of relieving back pain and/or leg pain.
This procedure is called nonsurgical decompression therapy (as opposed to surgical spinal decompression, such as laminectomy and microdiscectomy).
In This Article:
- All About Spinal Decompression Therapy
- How Spinal Decompression Therapy is Thought to Work
- Potential Candidates for Spinal Decompression Therapy
Theory of Spinal Decompression
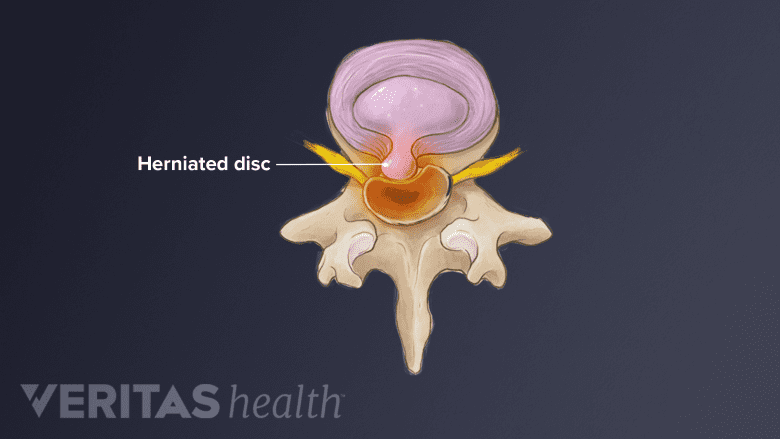
Spinal decompression aims to create negative pressure, potentially aiding herniated disc retraction.
Spinal decompression devices use the same basic principle of spinal traction that has been offered by chiropractors, osteopaths, and other appropriately trained health professionals for many years.
Both traction and decompression therapy are applied with the goals of relieving pain and promoting an optimal healing environment for bulging, degenerating, or herniated discs.
See What's a Herniated Disc, Pinched Nerve, Bulging Disc...? and What Is Degenerative Disc Disease?
Spinal decompression is a type of traction therapy applied to the spine in an attempt to bring about several theoretical benefits including:
- Create a negative intradiscal pressure to promote retraction or repositioning of the herniated or bulging disc material.
- Create a lower pressure in the disc that will cause an influx of healing nutrients and other substances into the disc.1
Clinical Evidence
While the fundamental theory of spinal decompression is widely accepted as valid, there is a lack of evidence supporting decompression therapy as being efficacious. Additionally there are some potential risks.
Although some studies that do not include control groups conclude that decompression therapy is efficacious, the few that do generally conclude that mechanized spinal decompression is no better than sham decompression. [Schimmel JJ, et al. European Spine Journal 18(12):1843-50, 2009] Thus, there is insufficient evidence that spinal decompression therapy is as effective, or more effective, than less expensive manual methods in treating back pain or injured herniated discs.2
A review of medical literature to date indicates that most clinical trials examining the efficacy of spinal decompression therapy or traction were lacking in one or more areas, such as inadequate numbers of subjects to make a statistically valid conclusion, lack of blinding (the patient or provider is unaware of the treatment given), no comparison to a placebo group (called a sham-controlled study), or lack of comparison to a treatment alternative.3 At the time of this article, few clinical studies of spinal decompression therapy have been published in peer-reviewed medical journals.

