The success rates of epidural steroid injections can vary depending on several factors. While some patients experience significant pain relief,1Patel K, Upadhyayula S. Epidural Steroid Injections. [Updated 2019 May 2]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK470189/,2Pandey RA. Efficacy of Epidural Steroid Injection in Management of Lumbar Prolapsed Intervertebral Disc: A Comparison of Caudal, Transforaminal and Interlaminar Routes. J Clin Diagn Res. 2016;10(7):RC05–RC11. doi:10.7860/JCDR/2016/18208.8127 others may not experience any pain relief from this procedure.3Pandey RA. Efficacy of Epidural Steroid Injection in Management of Lumbar Prolapsed Intervertebral Disc: A Comparison of Caudal, Transforaminal and Interlaminar Routes. J Clin Diagn Res. 2016;10(7):RC05–RC11. doi:10.7860/JCDR/2016/18208.8127,4Manchikanti L, Kaye AD, Manchikanti K, Boswell M, Pampati V, Hirsch J. Efficacy of Epidural Injections in the Treatment of Lumbar Central Spinal Stenosis; A Systematic Review. Anesthesiology and Pain Medicine. 2015;5(1). The effects of the injection may be short-term, such as a week, or may continue for a year.
Factors that Contribute to a Successful Epidural Steroid Injection: All You Need to Know

The transforaminal and interlaminar techniques may be more effective than the caudal technique.
The efficacy of an epidural depends on many factors, including but not limited to:
- Underlying condition. This injection treatment is usually more effective in managing lower back pain with radiating leg pain or sciatica versus lower back pain alone.1Patel K, Upadhyayula S. Epidural Steroid Injections. [Updated 2019 May 2]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK470189/,5Hassan KZ, Sherman Al. Epidural Steroids. [Updated 2019 May 10]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-.Available from: https://www.ncbi.nlm.nih.gov/books/NBK537320/ While the injection may also be used to treat non-radicular, localized back pain, the efficacy may be low.3Pandey RA. Efficacy of Epidural Steroid Injection in Management of Lumbar Prolapsed Intervertebral Disc: A Comparison of Caudal, Transforaminal and Interlaminar Routes. J Clin Diagn Res. 2016;10(7):RC05–RC11. doi:10.7860/JCDR/2016/18208.8127
- Route of administration. Research indicates that the transforaminal and interlaminar routes may obtain more effective results compared to the caudal route.2Pandey RA. Efficacy of Epidural Steroid Injection in Management of Lumbar Prolapsed Intervertebral Disc: A Comparison of Caudal, Transforaminal and Interlaminar Routes. J Clin Diagn Res. 2016;10(7):RC05–RC11. doi:10.7860/JCDR/2016/18208.8127,4Manchikanti L, Kaye AD, Manchikanti K, Boswell M, Pampati V, Hirsch J. Efficacy of Epidural Injections in the Treatment of Lumbar Central Spinal Stenosis; A Systematic Review. Anesthesiology and Pain Medicine. 2015;5(1).,6Manchikanti L, Benyamin RM, Falco FJ, Kaye AD, Hirsch JA. Do Epidural Injections Provide Short- and Long-term Relief for Lumbar Disc Herniation? A Systematic Review. Clin Orthop Relat Res. 2015;473(6):1940–1956. doi:10.1007/s11999-014-3490-4
- Type of steroid. Poorly soluble or particulate steroids, such as methylprednisolone or triamcinolone, have a long duration of action. Water-soluble or non-particulate steroids, such as dexamethasone, are considered safer than particulate steroids but tend to have a short-term effect.5Hassan KZ, Sherman Al. Epidural Steroids. [Updated 2019 May 10]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-.Available from: https://www.ncbi.nlm.nih.gov/books/NBK537320/,7Knezevic NN, Jovanovic F, Voronov D, Candido KD. Do Corticosteroids Still Have a Place in the Treatment of Chronic Pain?. Front Pharmacol. 2018;9:1229. Published 2018 Nov 1. doi:10.3389/fphar.2018.01229,8Dietrich TJ, Sutter R, Froehlich JM, Pfirrmann CWA. Particulate versus non-particulate steroids for lumbar transforaminal or interlaminar epidural steroid injections: an update. Skeletal Radiology. 2014;44(2):149-155. doi:10.1007/s00256-014-2048-6
In This Article:
- Lumbar Epidural Steroid Injections for Low Back Pain and Sciatica
- How Epidural Steroid Injections Work
- Indications for Lumbar Epidural Injections
- Epidural Injection Procedure
- Epidural Steroid Injection Pain Relief Success Rates
- Epidural Steroid Injections: Risks and Side Effects
- Epidural Steroid Injections for Back Pain and Leg Pain Video
The injection may sometimes be used in combination with a comprehensive rehabilitation program to increase the likelihood of longer-term pain relief and return to everyday activities.6Manchikanti L, Benyamin RM, Falco FJ, Kaye AD, Hirsch JA. Do Epidural Injections Provide Short- and Long-term Relief for Lumbar Disc Herniation? A Systematic Review. Clin Orthop Relat Res. 2015;473(6):1940–1956. doi:10.1007/s11999-014-3490-4
Other factors that may affect the outcome of this treatment include the physician’s skill and experience in administering the injection, the use of guided fluoroscopy, and the patient’s general health. The treatment may also be more effective in treating acute pain (versus chronic symptoms).
The success rates of epidural steroid injections for the treatment of a few common conditions are discussed below.
Epidural Steroid Injections: Success Rates for Treating Sciatica from Different Conditions

Sciatica occurs when a herniated disc or narrow bony opening compresses a nerve root in the lower back.
Sciatica, which is medically known as lumbar radiculopathy, is nerve pain that originates deep in the buttock and travels down to the thigh and/or leg. Sciatica is commonly caused when a herniated disc or narrowing of the bony opening for spinal nerves (foraminal spinal stenosis) compresses a nerve root in the lumbar spine.1Patel K, Upadhyayula S. Epidural Steroid Injections. [Updated 2019 May 2]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK470189/
Clinical trial results in the treatment of sciatica pain with epidural steroid injections have the following success rates:
Lumbar herniated disc. An analysis of several large clinical trials indicated that 40% to 80% of patients experienced over 50% improvement in sciatica pain and functional outcome from 3 months up to 1 year when 1 to 4 injections were given in that year.6Manchikanti L, Benyamin RM, Falco FJ, Kaye AD, Hirsch JA. Do Epidural Injections Provide Short- and Long-term Relief for Lumbar Disc Herniation? A Systematic Review. Clin Orthop Relat Res. 2015;473(6):1940–1956. doi:10.1007/s11999-014-3490-4 Typically, a better outcome is seen in acute sciatica pain of recent onset with a lesser degree of spinal nerve compression.3Pandey RA. Efficacy of Epidural Steroid Injection in Management of Lumbar Prolapsed Intervertebral Disc: A Comparison of Caudal, Transforaminal and Interlaminar Routes. J Clin Diagn Res. 2016;10(7):RC05–RC11. doi:10.7860/JCDR/2016/18208.8127
Foraminal spinal stenosis. In a study group of 60 participants, sciatica pain was relieved in 87% of patients with mild to moderate stenosis and 42% of patients with severe stenosis. The treatment included 1 injection and the effects lasted up to 3 months.9Chang MC, Lee DG. Outcome of Transforaminal Epidural Steroid Injection According to the Severity of Lumbar Foraminal Spinal Stenosis. Pain Physician. 2018;21(1):67-72.
Other conditions such as spinal cysts or ligament thickening that cause spinal nerve compression and radicular nerve pain in the legs may also yield similar results when treated with these injections.
Effectiveness of Epidural Injections for Axial Back Pain
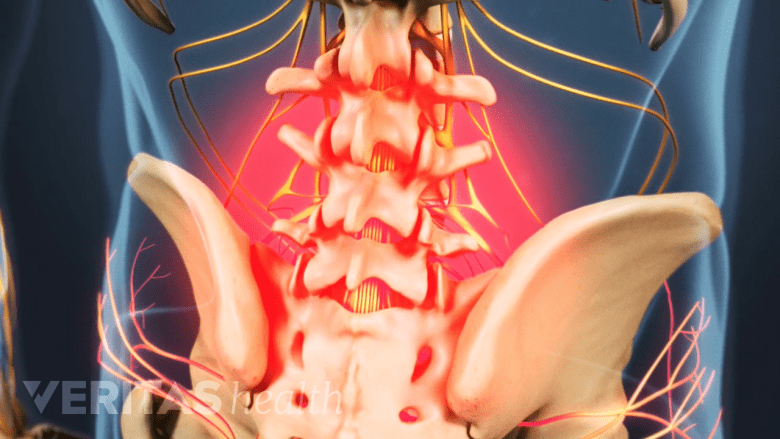
Axial low back pain refers to pain localized within the lower back area.
Localized lower back pain is typically caused due to inflammatory changes within the spinal soft tissues or lumbar discs.3Pandey RA. Efficacy of Epidural Steroid Injection in Management of Lumbar Prolapsed Intervertebral Disc: A Comparison of Caudal, Transforaminal and Interlaminar Routes. J Clin Diagn Res. 2016;10(7):RC05–RC11. doi:10.7860/JCDR/2016/18208.8127,10Chang, Douglas, Zlomislic, Vinko. Chapter 273. Lumbar Spinal Injections. In: Chapman, Michael W. Chapman's Orthopaedic Surgery. Philadelphia: Lippincott Williams & Wilkins. https://www.researchgate.net/publication/327034223_Lumbar_spinal_injections_Chapman's_Orthopaedic_Surgery_Chapter_273. Accessed June 26, 2019.,11Fujii K, Yamazaki M, Kang JD, et al. Discogenic Back Pain: Literature Review of Definition, Diagnosis, and Treatment. JBMR Plus. 2019;3(5):e10180. Published 2019 Mar 4. doi:10.1002/jbm4.10180
In a study involving 120 participants with axial low back pain, treatment with 4 injections given over a span of 1 year showed more than 50% improvement in pain and functional outcome in 68% of patients.12Manchikanti L, Pampati V, Benyamin RM, Boswell MV. Analysis of efficacy differences between caudal and lumbar interlaminar epidural injections in chronic lumbar axial discogenic pain: local anesthetic alone vs. local combined with steroids. Int J Med Sci. 2015;12(3):214–222. Published 2015 Jan 20. doi:10.7150/ijms.10870 Other studies have reported pain relief for 2 years when 6 injections were spaced out and given during this period.13Manchikanti L, Cash, McManus, Pampati. Fluoroscopic caudal epidural injections in managing chronic axial low back pain without disc herniation, radiculitis, or facet joint pain. Journal of Pain Research. October 2012:381. doi:10.2147/jpr.s35924
Analyzing Success Rates for Neurogenic Claudication
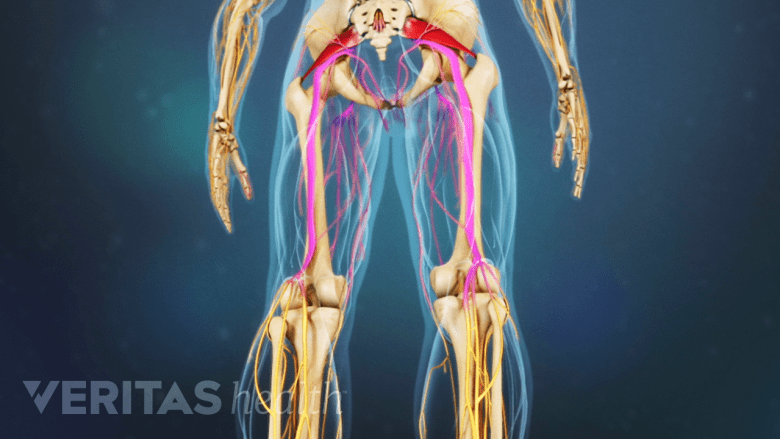
Epidural steroid injections may help relieve leg pain while walking.
Neurogenic claudication, characterized by pain felt in both legs while walking variable distances, is usually treated with bilateral transforaminal epidural steroid injections (given on both sides of the spine).
A study involving 22 participants showed 30% of patients experiencing pain relief at 1 month, 53% at 3 months, and 44% at 6 months after receiving bilateral injections.14Farooque M, Salzman MM, Ye Z. Effectiveness of Bilateral Transforaminal Epidural Steroid Injections in Degenerative Lumbar Spinal Stenosis Patients With Neurogenic Claudication: A Case Series. PM&R. 2016;9(1):26-31. doi:10.1016/j.pmrj.2016.06.002 Other studies have reported pain relief for 2 years when 6 injections were spaced out and given during this period.4Manchikanti L, Kaye AD, Manchikanti K, Boswell M, Pampati V, Hirsch J. Efficacy of Epidural Injections in the Treatment of Lumbar Central Spinal Stenosis; A Systematic Review. Anesthesiology and Pain Medicine. 2015;5(1).
Number of Epidural Steroid Injections Needed for Pain Relief
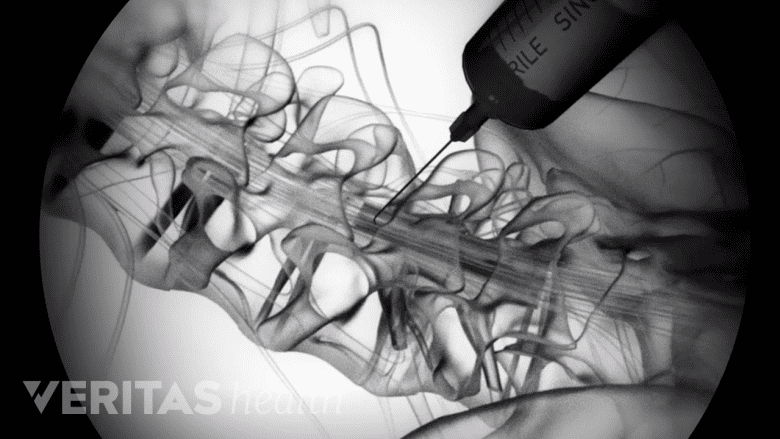
Fluoroscopy helps the physician guide the needle accurately into the epidural space.
Research indicates that an additional injection may be given if the following criteria are met3Pandey RA. Efficacy of Epidural Steroid Injection in Management of Lumbar Prolapsed Intervertebral Disc: A Comparison of Caudal, Transforaminal and Interlaminar Routes. J Clin Diagn Res. 2016;10(7):RC05–RC11. doi:10.7860/JCDR/2016/18208.8127:
- More than 50% of pain reduction was experienced after the first injection
- The effect of the first injection decreased after a considerable relief period, for example, over 1 month
Common guidelines recommend that if more than 4 epidural steroid injections are needed in 1 year, the underlying condition must be managed by other treatment methods.3Pandey RA. Efficacy of Epidural Steroid Injection in Management of Lumbar Prolapsed Intervertebral Disc: A Comparison of Caudal, Transforaminal and Interlaminar Routes. J Clin Diagn Res. 2016;10(7):RC05–RC11. doi:10.7860/JCDR/2016/18208.8127
To improve the overall outcome of the procedure and reduce the risk of side effects, using a blunt needle, live fluoroscopy, and administering a small test dose initially may be helpful.15Pountos I, Panteli M, Walters G, Bush D, Giannoudis PV. Safety of Epidural Corticosteroid Injections. Drugs R D. 2016;16(1):19–34. doi:10.1007/s40268-015-0119-3
Benefits of Combining Physical Therapy with Epidural Steroid Injection

Combining physical therapy and epidural steroid injection treatment may help improve the overall outcome.
A guided physical therapy program may be combined with the epidural steroid injection treatment for an added benefit. Studies suggest that combining physical therapy with the injection treatment of herniated discs may improve the quality of pain relief and overall satisfaction in the patient.16van Helvoirt H, Apeldoorn AT, Ostelo RW, et al. Transforaminal Epidural Steroid Injections Followed by Mechanical Diagnosis and Therapy to Prevent Surgery for Lumbar Disc Herniation. Pain Medicine. 2014;15(7):1100-1108. doi:10.1111/pme.12450 Injection treatment of lower back conditions such as lumbar spinal stenosis may benefit from improved quality of life and overall health when combined with physical therapy; with no direct effect on pain-relief values.17Hammerich A, Whitman J, Mintken P, et al. Effectiveness of Physical Therapy Combined With Epidural Steroid Injection for Individuals With Lumbar Spinal Stenosis: A Randomized Parallel-Group Trial. Archives of Physical Medicine and Rehabilitation. 2019;100(5):797-810. doi:10.1016/j.apmr.2018.12.035,18Akuthota V, Hammerich AS, Mintken PE, et al. Effectiveness of Physical Therapy as an Adjunct to Epidural Steroid Injections in the Treatment of Lumbar Spinal Stenosis: A Pilot Randomized Controlled Trial. The Spine Journal. 2012;12(9):S146. doi:10.1016/j.spinee.2012.08.379
- 1 Patel K, Upadhyayula S. Epidural Steroid Injections. [Updated 2019 May 2]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK470189/
- 2 Pandey RA. Efficacy of Epidural Steroid Injection in Management of Lumbar Prolapsed Intervertebral Disc: A Comparison of Caudal, Transforaminal and Interlaminar Routes. J Clin Diagn Res. 2016;10(7):RC05–RC11. doi:10.7860/JCDR/2016/18208.8127
- 3 Pandey RA. Efficacy of Epidural Steroid Injection in Management of Lumbar Prolapsed Intervertebral Disc: A Comparison of Caudal, Transforaminal and Interlaminar Routes. J Clin Diagn Res. 2016;10(7):RC05–RC11. doi:10.7860/JCDR/2016/18208.8127
- 4 Manchikanti L, Kaye AD, Manchikanti K, Boswell M, Pampati V, Hirsch J. Efficacy of Epidural Injections in the Treatment of Lumbar Central Spinal Stenosis; A Systematic Review. Anesthesiology and Pain Medicine. 2015;5(1).
- 5 Hassan KZ, Sherman Al. Epidural Steroids. [Updated 2019 May 10]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-.Available from: https://www.ncbi.nlm.nih.gov/books/NBK537320/
- 6 Manchikanti L, Benyamin RM, Falco FJ, Kaye AD, Hirsch JA. Do Epidural Injections Provide Short- and Long-term Relief for Lumbar Disc Herniation? A Systematic Review. Clin Orthop Relat Res. 2015;473(6):1940–1956. doi:10.1007/s11999-014-3490-4
- 7 Knezevic NN, Jovanovic F, Voronov D, Candido KD. Do Corticosteroids Still Have a Place in the Treatment of Chronic Pain?. Front Pharmacol. 2018;9:1229. Published 2018 Nov 1. doi:10.3389/fphar.2018.01229
- 8 Dietrich TJ, Sutter R, Froehlich JM, Pfirrmann CWA. Particulate versus non-particulate steroids for lumbar transforaminal or interlaminar epidural steroid injections: an update. Skeletal Radiology. 2014;44(2):149-155. doi:10.1007/s00256-014-2048-6
- 9 Chang MC, Lee DG. Outcome of Transforaminal Epidural Steroid Injection According to the Severity of Lumbar Foraminal Spinal Stenosis. Pain Physician. 2018;21(1):67-72.
- 10 Chang, Douglas, Zlomislic, Vinko. Chapter 273. Lumbar Spinal Injections. In: Chapman, Michael W. Chapman's Orthopaedic Surgery. Philadelphia: Lippincott Williams & Wilkins. https://www.researchgate.net/publication/327034223_Lumbar_spinal_injections_Chapman's_Orthopaedic_Surgery_Chapter_273. Accessed June 26, 2019.
- 11 Fujii K, Yamazaki M, Kang JD, et al. Discogenic Back Pain: Literature Review of Definition, Diagnosis, and Treatment. JBMR Plus. 2019;3(5):e10180. Published 2019 Mar 4. doi:10.1002/jbm4.10180
- 12 Manchikanti L, Pampati V, Benyamin RM, Boswell MV. Analysis of efficacy differences between caudal and lumbar interlaminar epidural injections in chronic lumbar axial discogenic pain: local anesthetic alone vs. local combined with steroids. Int J Med Sci. 2015;12(3):214–222. Published 2015 Jan 20. doi:10.7150/ijms.10870
- 13 Manchikanti L, Cash, McManus, Pampati. Fluoroscopic caudal epidural injections in managing chronic axial low back pain without disc herniation, radiculitis, or facet joint pain. Journal of Pain Research. October 2012:381. doi:10.2147/jpr.s35924
- 14 Farooque M, Salzman MM, Ye Z. Effectiveness of Bilateral Transforaminal Epidural Steroid Injections in Degenerative Lumbar Spinal Stenosis Patients With Neurogenic Claudication: A Case Series. PM&R. 2016;9(1):26-31. doi:10.1016/j.pmrj.2016.06.002
- 15 Pountos I, Panteli M, Walters G, Bush D, Giannoudis PV. Safety of Epidural Corticosteroid Injections. Drugs R D. 2016;16(1):19–34. doi:10.1007/s40268-015-0119-3
- 16 van Helvoirt H, Apeldoorn AT, Ostelo RW, et al. Transforaminal Epidural Steroid Injections Followed by Mechanical Diagnosis and Therapy to Prevent Surgery for Lumbar Disc Herniation. Pain Medicine. 2014;15(7):1100-1108. doi:10.1111/pme.12450
- 17 Hammerich A, Whitman J, Mintken P, et al. Effectiveness of Physical Therapy Combined With Epidural Steroid Injection for Individuals With Lumbar Spinal Stenosis: A Randomized Parallel-Group Trial. Archives of Physical Medicine and Rehabilitation. 2019;100(5):797-810. doi:10.1016/j.apmr.2018.12.035
- 18 Akuthota V, Hammerich AS, Mintken PE, et al. Effectiveness of Physical Therapy as an Adjunct to Epidural Steroid Injections in the Treatment of Lumbar Spinal Stenosis: A Pilot Randomized Controlled Trial. The Spine Journal. 2012;12(9):S146. doi:10.1016/j.spinee.2012.08.379

