Pain usually occurs when the nerves relay a pain signal following an injury or damage somewhere in the body. Neuropathic pain—also called nerve pain—is different, resulting from damage to the nerves themselves.
In This Article:
Common Factors Contributing to Neuropathic Pain

Cancer or tumors may be a common contributing factor to neuropathic pain.
Uncovering the cause of nerve damage is the first step in treating neuropathic pain. Factors that often cause or contribute to neuropathic pain include:
- Cancer
- Compression of a nerve or nerves
- Diabetes
- Excessive alcohol use
- Exposure to medication-related or other toxins
- Hormonal disorders
- Immune system disorders
- Infections
- Vitamin deficiencies
Unfortunately, the cause of neuropathic pain cannot always be determined or reversed. In these cases treatment may allow nerves to heal gradually, easing the pain. When medical care for the pain is delayed, the pain can be more difficult to manage, requiring more aggressive treatment.
See Types of Back Pain: Acute Pain, Chronic Pain, and Neuropathic Pain
Relief of Neuropathic Pain Symptoms Takes Priority
If no cause of neuropathic pain is found—or if the cause cannot be eliminated or reversed—treatment emphasizes relief of symptoms and strategies to improve daily functioning. There is no single treatment to cure or prevent neuropathic pain.
Early treatment is important to treat the symptoms, however. Receiving care as soon as possible may help prevent or lessen problems that often accompany neuropathy, such as depression, sleeplessness, and diminished functioning.
See Chronic Pain and Insomnia: Breaking the Cycle
Common Treatments Target Causes, Symptoms
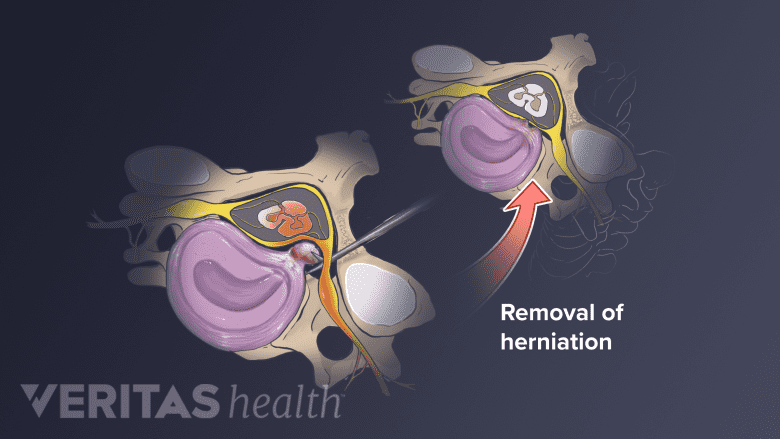
Neuropathy caused by a herniated disc sometimes requires surgical intervention.
Neuropathy takes many forms, and the treatments for neuropathic pain are varied as well. Following are three common causes and treatments for neuropathic pain:
Multiple malfunctions. When peripheral nerves in more than one part of the body malfunction at the same time, the condition is called polyneuropathy. Diabetes is the most common etiology—or cause—of polyneuropathy.
Treating the underlying issue may stabilize the condition, reducing symptoms. This could involve better blood sugar control in people with diabetic neuropathy to reduce symptoms and prevent additional damage to the nerves. If a vitamin deficiency is causing the pain, changes in diet or supplementation will typically be recommended.
- Nerve compression. Nerves can be compressed at any point, leading to pain. The pressure could be from a herniated disc, a trapped median nerve in carpal tunnel syndrome, or other causes. Decompression surgery releases the pressure on the nerve, relieving the pain.1 This treatment is typically effective when a small number of nerves are affected, but not when nerves over a wide area are compressed.
- Injury to a nerve. The immediate area of injury as well as nearby areas can be affected when a nerve is injured due to a sudden impact. Neuropathic pain caused by an injury to a nerve may improve with time. Having the injury checked by a doctor is advised, however, to avoid the risk of further damage.
This is not a comprehensive list of causes. A wide range of conditions can cause neuropathic pain in the peripheral and central nervous systems.
See All About Neuropathy And Chronic Back Pain
Treatment by an interdisciplinary pain management team can be useful for the typically severe symptoms of neuropathy. In these settings, professionals from various specialties work together to reduce patients’ symptoms and improve functioning.

