An epidural steroid injection is a minimally invasive procedure that is performed at a doctor’s office, surgical center, or hospital. Patients usually return home the same day. The injection may be administered by spine and pain management specialists, such as physiatrists, anesthesiologists, radiologists, neurologists, and spine surgeons.
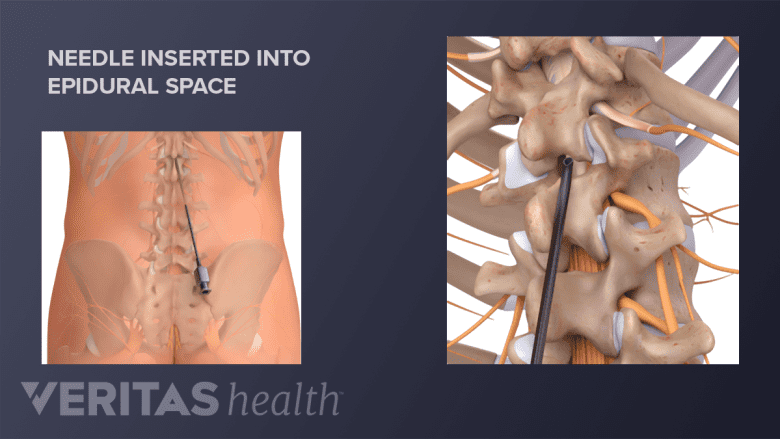
In the epidural injection procedure, the steroid medication is injected into the epidural space.
A complete list of current medications and medications taken in the recent past, such as blood thinners and antibiotics, must be discussed with the doctor. Some of these medications may need to be stopped a few days before the injection procedure to avoid complications. It will also be necessary to sign a consent form before the procedure after the possible benefits and risks have been discussed with the doctor.
In This Article:
- Lumbar Epidural Steroid Injections for Low Back Pain and Sciatica
- How Epidural Steroid Injections Work
- Indications for Lumbar Epidural Injections
- Epidural Injection Procedure
- Epidural Steroid Injection Pain Relief Success Rates
- Epidural Steroid Injections: Risks and Side Effects
- Epidural Steroid Injections for Back Pain and Leg Pain Video
Preparing to Receive an Epidural Steroid Injection
The injection procedure is usually scheduled for the morning. Instructions typically include no eating and drinking for about 6 hours before the procedure. A hospital gown is worn to allow better access to the injection site. Conscious sedation using relaxation medication may be given to ease the patient’s anxiety.
Procedure for Lumbar Epidural Steroid Injection: Steps and Precautions
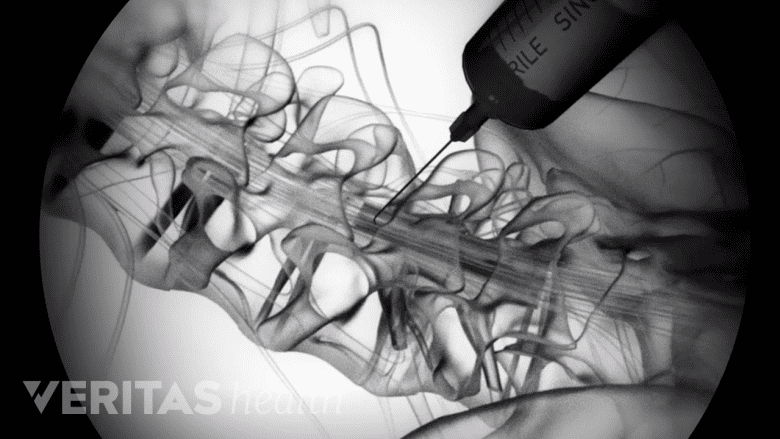
A contrast dye is injected into the epidural space to check the spread of the injected contents.
The injection is usually given while the patient lies on their stomach (prone position) on a fluoroscopy (live x-ray) table. The procedure may take up to 30 minutes. The doctor may decide to use a transforaminal, interlaminar, or caudal route to administer the injection. An intravenous (IV) line is started if relaxation medicine is needed.
The common steps involved in the injection procedure are as follows1Patel K, Upadhyayula S. Epidural Steroid Injections. [Updated 2019 May 2]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK470189/:
- The skin over the injection site is marked and cleaned with betadine.
- A fluoroscopic x-ray is used to locate the correct vertebral level for needle guidance; the live images can be seen on a computer screen.
- A local anesthetic is injected into the skin and underlying tissues to numb the area.
- An epidural spinal needle is inserted into the intended injection site and guided using fluoroscopy.
- A contrast dye is injected into the epidural space to check the spread of the injected contents.
- Once the spread is confirmed, the steroid medication is injected into the epidural space.
A tingling or mild burning sensation or the feeling of pressure may be experienced as the medication enters the epidural space. When the injection is completed, the irritation and discomfort usually disappear within a few minutes. The patient is usually monitored in a recovery room for 30 minutes to an hour where vital signs are continuously monitored.
Driving and strenuous physical activities and flying in an airplane are not recommended on the same day after the procedure.
Recovery and Post-Injection Care Following Epidural Injection
While the local anesthetic in an epidural steroid injection usually provides immediate pain relief,2Chang, Douglas, Zlomislic, Vinko. Chapter 273. Lumbar Spinal Injections. In: Chapman, Michael W. Chapman's Orthopaedic Surgery. Philadelphia: Lippincott Williams & Wilkins. https://www.researchgate.net/publication/327034223_Lumbar_spinal_injections_Chapman's_Orthopaedic_Surgery_Chapter_273. Accessed June 26, 2019. it may take up to 2 weeks for the steroids to take effect.3Hassan KZ, Sherman Al. Epidural Steroids. [Updated 2019 May 10]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-.Available from: https://www.ncbi.nlm.nih.gov/books/NBK537320/
Returning to daily activities

Ice packs may be applied at the injection site if pain occurs.
Regular activities may be resumed slowly on the day after the injection. Ice packs may be used at home if pain occurs at the injection site. Ice packs are usually used for 15 to 20 minutes at a time with a break of at least two hours in between to avoid skin injury. Hot baths, sauna, and swimming are usually not recommended for 2 to 3 days after the injection to avoid the risk of infection.
The epidural injection procedure is usually painless, but light soreness or discomfort may occur in some patients over the next day or two. With adequate precautionary measures and post-injection care of the treatment site, patients can typically resume all their daily activities within a week of the injection.
- 1 Patel K, Upadhyayula S. Epidural Steroid Injections. [Updated 2019 May 2]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK470189/
- 2 Chang, Douglas, Zlomislic, Vinko. Chapter 273. Lumbar Spinal Injections. In: Chapman, Michael W. Chapman's Orthopaedic Surgery. Philadelphia: Lippincott Williams & Wilkins. https://www.researchgate.net/publication/327034223_Lumbar_spinal_injections_Chapman's_Orthopaedic_Surgery_Chapter_273. Accessed June 26, 2019.
- 3 Hassan KZ, Sherman Al. Epidural Steroids. [Updated 2019 May 10]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-.Available from: https://www.ncbi.nlm.nih.gov/books/NBK537320/

