Vertebral osteomyelitis refers to an infection of the vertebral body in the spine. It is a fairly rare cause of back pain, especially in young healthy adults.
Generally, the infection is spread to the vertebral body by a vascular route. The veins in the lower spine (Batson’s plexus) drain the pelvis and provide for a direct route of entry for the bacteria to get into the spine. For this reason, there is a preponderance of infections in the spine that occur after a urologic procedure (e.g. cystoscopy).
See Lumbar Spine Anatomy and Pain
Vertebral osteomyelitis may also be referred to as spinal osteomyelitis, or a spinal infection.
In This Article:
- Osteomyelitis, a Spinal Infection
- Osteomyelitis Symptoms
- Osteomyelitis Diagnosis
- Osteomyelitis Treatments
Common Causes of Osteomyelitis
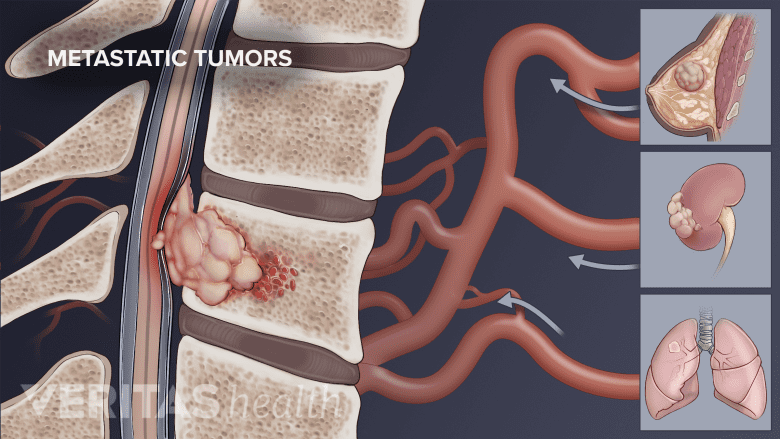
Cancers and tumors weaken the immune system, increasing the body's vulnerability to infections.
Patients susceptible to osteomyelitis include:
- Elderly patients
- Intravenous drug users
- Individuals whose immune systems are compromised
Conditions that compromise the immune system include:
- Long-term systemic administration of steroids to treat conditions such as rheumatoid arthritis
- Insulin Dependent Diabetes Mellitus
- Organ transplant patients
- Acquired Immune Deficiency Syndrome (AIDS)
- Malnutrition
- Cancer
Intravenous drug abuse is a growing cause of spinal infections. Typically, the organism most likely to infect the spine is Staphylococcus Aureus, but in the intravenous drug population, Pseudomonas infection is also a common cause of spinal infection. The treatment for these two pathogens requires different antibiotic therapy.
In the past, tuberculosis infections caused by Mycobacterium Tuberculosis were very common. In North America, this type of infection is not common anymore, but it remains a common organism and cause of spinal infections in countries where there is a lot of poverty. Intravenous drug users are more likely than other patients to contract Mycobacterium Tuberculosis.
Most vertebral body infections occur in the lumbar spine because of the blood flow to this region of the spine. Tuberculosis infections have a predilection for the thoracic spine, and intravenous drug abusers are more likely to contract an infection of the cervical spine.


