Symptoms of back pain due to a spinal infection often develop insidiously and over a long period of time.
In This Article:
- Osteomyelitis, a Spinal Infection
- Osteomyelitis Symptoms
- Osteomyelitis Diagnosis
- Osteomyelitis Treatments
Symptoms and Complications of Vertebral Osteomyelitis
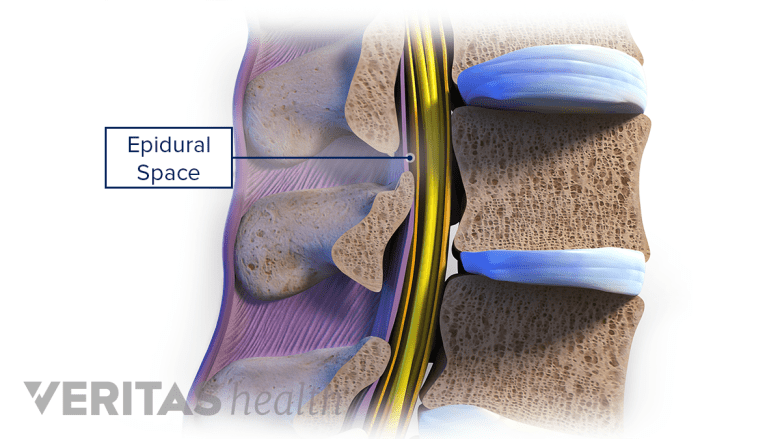
Spinal infection in the epidural space can compress the nerves, causing possible complications.
In addition to back pain, which is present in over 90% of patients with vertebral osteomyelitis, general symptoms may include one or a combination of the following constitutional symptoms:
- Fever, chills, or shakes
- Unplanned weight loss
- Nighttime pain that is worse than daytime pain
- Swelling and possible warmth and redness around the infection site
A spinal infection rarely affects the nerves in the spine. However, the infection may move into the spinal canal and cause an epidural abscess, which can place pressure on the neural elements. If this happens in the cervical or thoracic spine, it can result in paraplegia or quadriplegia. If it happens in the lumbar spine it can result in cauda equina syndrome (a syndrome that leads to bowel and bladder incontinence, saddle anesthesia, and possible lower extremity weakness).
The most common site of vertebral bone infection is in the lower back, or lumbar spine, followed by the thoracic(upper) spine, the cervical spine(neck). It may also develop in the sacrum, the bone at the very bottom of the spine that connects to the pelvis.
See Sacroiliac Joint Dysfunction (SI Joint Pain)
Symptoms of vertebral osteomyelitis are highly variable depending on the patient, the location of the infection, and how far advanced it is. For example, while a fever is a typical symptom, some people may have no fever and others may run a high fever.
Lumbar infections may also present with pain when standing, irritation of muscles such as the psoas muscle (hip flexor) and hamstring (knee flexor), and a loss of lumbar lordosis. Cervical Spine Anatomy may present with torticollis (the inability to straighten out one’s neck).
Due to the variable, often vague, and general symptoms of the disease, vertebral osteomyelitis often goes undetected until the infection is quite advanced.


