Treatments for sacroiliac joint dysfunction (SI joint pain) typically focus on alleviating pain and restoring normal motion in the joint. Most cases of SI joint pain are effectively managed using non-surgical treatments.
In This Article:
- Sacroiliac Joint Dysfunction (SI Joint Pain)
- Sacroiliac Joint Dysfunction Symptoms and Causes
- Accurate Diagnosis of Sacroiliac Joint Dysfunction
- Treatment Options for Sacroiliac Joint Dysfunction
- Surgical Treatment for Sacroiliac Joint Pain
- Sacroiliac Joint Dysfunction Video
Initial Treatments for Sacroiliac Joint Pain
Initial treatments for sacroiliac joint pain typically include:
Brief rest period
A rest period of 1 to 2 days may be advised. Resting for longer than a couple days is not recommended, as doing so may worsen stiffness and cause increased pain and generalized deconditioning.
Applying ice or heat
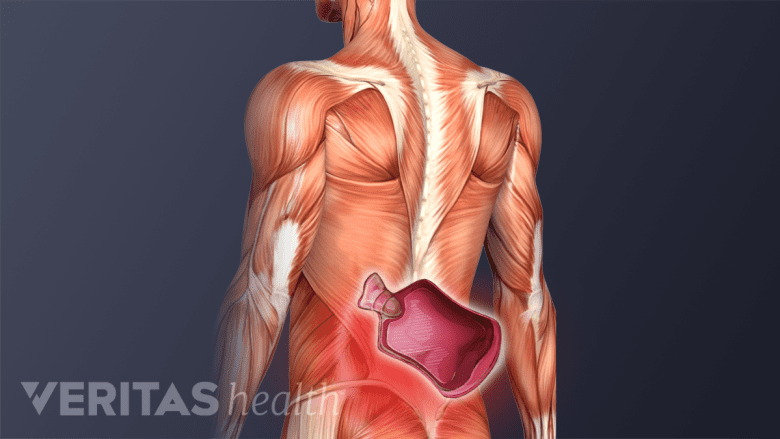
Heat therapy relaxes muscles and fosters healing by improving blood flow.
Ice applied to the low back and pelvis can reduce inflammation and alleviate pain and discomfort. Heat applied around the joint may help relieve pain by reducing muscle tension or spasms.
Pain medication
NSAIDs provide anti-inflammatory effects and help calm inflammation and pain in the back.
Over-the-counter pain relievers (such as acetaminophen) and anti-inflammatory medications (NSAIDs, such as ibuprofen or naproxen) may be recommended for mild to moderate pain relief. Prescription medications such as muscle relaxants or narcotic painkillers may be used during episodes of severe, acute pain. These medications must be used with caution, as they are highly addictive and can cause severe side effects.
See Medications for Back Pain and Neck Pain
Manual manipulation
Manual manipulation provided by a chiropractor, osteopathic doctor, or other qualified health professional can be highly effective if sacroiliac joint pain is caused by too little motion (hypomobility). This therapy consists of manual procedures applied to the SI joint and lower back region with the goal of reducing joint fixation and muscle tension, and restoring normal range of motion.1Bise CG, Piva SR, Erhard R. Manual Therapy. In: Orthopaedic Physical Therapy Secrets. Elsevier; 2017:85-94. doi:10.1016/b978-0-323-28683-1.00012-6
See Chiropractic Procedures for the Sacroiliac Joint
Supports or braces
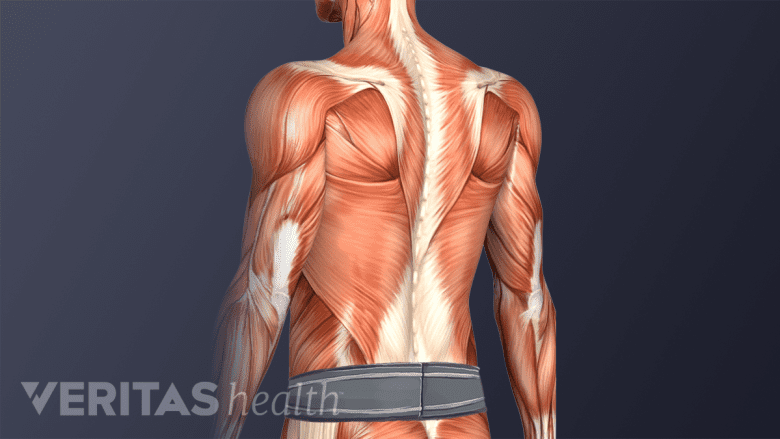
A pelvic brace can help stabilize the spine and assist in the recovery process.
When the SI joint is too loose (hypermobile), a pelvic brace can be wrapped around the waist and pulled snugly to stabilize the area. A pelvic brace is about the size of a wide belt and can be helpful when the joint is inflamed and painful.
Sacroiliac joint injections
A local anesthetic (such as lidocaine or bupivacaine) is injected with an anti-inflammatory medication (such as a corticosteroid) to reduce inflammation and help alleviate pain. The pain relief from a joint injection can help minimize pain when starting a physical therapy program and returning to normal activity levels.
There is no single approach to managing SI joint pain that will work for everyone. A combination of non-surgical treatments is usually necessary for effective pain relief. Additionally, a period of trial-and-error may be needed to find treatments that address specific symptoms.
Watch How to Avoid an SI Joint Pain Flare-Up Video
Physical Therapy for Sacroiliac Joint Pain
Hamstring stretches promote flexibility and reduce muscle tightness in the lower back and legs.
Physical therapy to rehabilitate the sacroiliac joint typically includes:
Stretching to reduce muscle tension and spasms in the lower back, hips, and pelvis, including the piriformis, gluteus maximus, and hamstring muscles. Tension in these muscles caused by sacroiliac joint dysfunction can be the primary cause of pain.
Strengthening exercises to better support the sacroiliac joint and pelvis/lower back. Better support for the joint can come from strengthening the abdominal muscles, lateral trunk muscles, and low back muscles.
See Strengthening Exercises for Sacroiliac Joint Pain Relief
Aerobic exercise to elevate blood flow and bring nutrients and oxygen to damaged tissues, which can facilitate the healing process. Low-impact aerobics may be needed for SI joint dysfunction to minimize pain from exercise, and can include stationary cycling, running on an elliptical, or water aerobics.
Exercises for sacroiliac joint dysfunction are designed to gently return the joint to normal function and mobility, in turn reducing pain and other symptoms. Exercises may be individualized and vary from case to case.
- 1 Bise CG, Piva SR, Erhard R. Manual Therapy. In: Orthopaedic Physical Therapy Secrets. Elsevier; 2017:85-94. doi:10.1016/b978-0-323-28683-1.00012-6

