Sciatica is diagnosed based on the patient’s symptoms, medical history, and physical examination. Medical imaging tests and diagnostic nerve blocks may be appropriate in some cases.
In This Article:
- What You Need to Know About Sciatica
- Sciatica Symptoms
- Sciatica Causes
- Diagnosing the Cause of Sciatica
- Sciatica Treatment
- Sciatica Surgery
- Sciatica Causes and Symptoms Video
Sciatica Diagnosis: Physical Examination and Medical History
Doctors check for areas affected by pain along the sciatic nerve.
The goal of conducting a physical exam and review of medical history is to identify the pain pattern in the patient’s leg.
Sciatica pain typically follows the areas of skin – called the dermatome – that are supplied by the sciatic nerve. The pain may also include other deeper tissues outside the classic dermatomal areas, called dynatomes. It is believed that pain from all the nerve roots that comprise the sciatic nerve usually have a dynatomal distribution, except S1 nerve pain, or classic sciatica, which typically involves a dermatomal pain pattern.1Gore S, Nadkarni S. Sciatica: detection and confirmation by new method. Int J Spine Surg. 2014;8:15. Published 2014 Dec 1. doi:10.14444/1015.
Physical examination
During a physical examination, the doctor may check for:
- Localized pain in the low back, buttock, thigh, and leg
- The response to leg movements that elongate the nerve (straightening the leg)
- The response to certain stimuli, such as gently pressing the toes or calf region
The doctor may also conduct certain clinical tests to check for sciatic nerve pain.
Clinical tests for sciatica
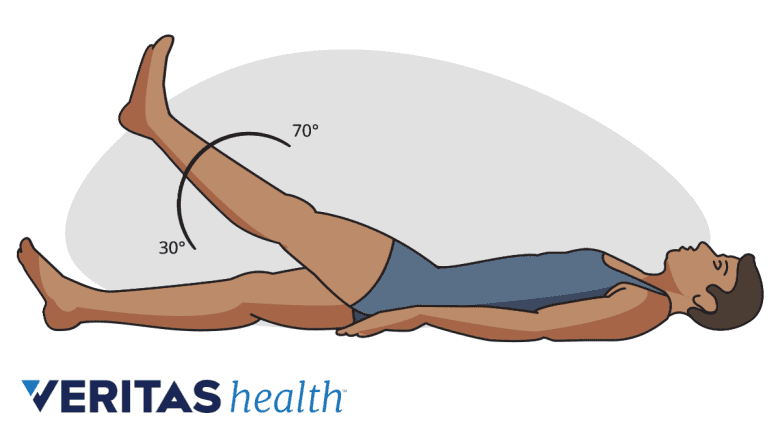
A straight leg raise test is often used to diagnose nerve root compression in the back.
A few examples of clinical tests for sciatica include1Gore S, Nadkarni S. Sciatica: detection and confirmation by new method. Int J Spine Surg. 2014;8:15. Published 2014 Dec 1. doi:10.14444/1015.:
- Straight leg raise (SLR) test. This test includes the patient lying on his/her back and lifting one leg at a time with the other leg flat or bent at the knee. A pain encountered while lifting the affected leg usually indicates sciatica.
- Slump test. This test includes the patient seated upright with hands behind the back. The patient bends (slumps) forward at the hip. The neck is bent down with the chin touching the chest and one knee is extended to a degree possible. If pain occurs in this position, sciatica may be present.
These tests, however, may be positive only when the sciatic nerve is mechanically compressed at any point along its origin, such as from a herniated disc. Other causes of sciatica such as inflammation or chemical irritation of the nerve may not cause pain in these tests.1Gore S, Nadkarni S. Sciatica: detection and confirmation by new method. Int J Spine Surg. 2014;8:15. Published 2014 Dec 1. doi:10.14444/1015.
Medical history

Doctors review the patient's medical history in detail to understand the cause of pain.
A medical history may include the doctor reviewing the following:
- The onset of pain and other symptoms
- Type, nature, and duration of pain
- Trauma or injury to the back or hip area
- The occurrence of muscle spasms or cramps in the pelvic region
- Decreased strength in the leg
See Preparing to See A Doctor for Back and Neck Pain
If sciatica is suspected, some doctors may order medical imaging or diagnostic nerve block tests. These tests are used to confirm the cause of sciatica. Medical imaging or diagnostic injections also help plan surgeries or other invasive treatments.
Medical Imaging Tests for Sciatica

An MRI scan can help doctors visualize the delicate nerves and tissues in the spine.
Medical imaging tests used in diagnosing the cause of sciatica include:
- Magnetic resonance imaging (MRI). An MRI scan allows the doctor to visualize the sciatic nerve, surrounding soft tissues, and facet joint capsules. Tumors, facet joint inflammation, and herniated discs affecting nerve roots may also be seen on MRI scans.
- Discogram. A discogram test may be helpful in determining abnormalities in an intervertebral disc. A contrast dye injected into the tissues may allow abnormalities in the disc, such as bulging or herniation to be seen on a medical imaging scan (such as computed tomography scan).
A discogram may also be useful in identifying chemically induced sciatic nerve pain.1Gore S, Nadkarni S. Sciatica: detection and confirmation by new method. Int J Spine Surg. 2014;8:15. Published 2014 Dec 1. doi:10.14444/1015.
Diagnostic Nerve Block Injections for Sciatica
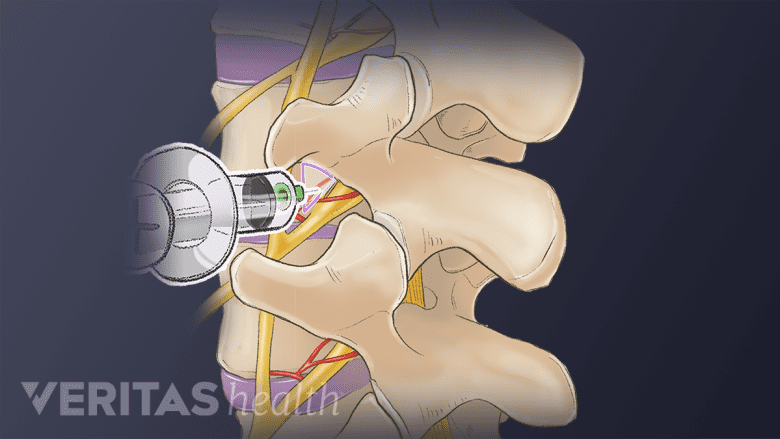
Nerve block injections aim to stop pain signals from being transmitted through a specific nerve.
Selective nerve block injections are considered an accurate and effective method in diagnosing sciatic nerve pain.
- An anesthetic solution is injected around the sciatic nerve root(s) to numb the pain transmitted by the nerve.
- The injection is performed under the guidance of fluoroscopy (live x-ray), ultrasound, or computed tomography (CT). These techniques allow the physician to guide the needle to the accurate location where the medication needs to be deposited.
If pain relief is experienced, sciatica may be confirmed.
As with any injection technique, a small risk of bleeding, nerve damage, and spinal cord tissue damage may be possible with diagnostic nerve block injections.
Watch: Sciatica Treatment Video
Once the cause of sciatica is diagnosed, a structured treatment approach for the specific condition is formulated. Both nonsurgical treatments and surgery are used to treat sciatica.
- 1 Gore S, Nadkarni S. Sciatica: detection and confirmation by new method. Int J Spine Surg. 2014;8:15. Published 2014 Dec 1. doi:10.14444/1015.

