Treating pain in the C2-C5 spinal motion segments typically begins with nonsurgical methods. Unstable vertebral injuries or worsening neurological deficits, such as arm or leg numbness or weakness may require surgical intervention.
In This Article:
Nonsurgical Treatment for C2-C5
Nonsurgical treatments for C2-C5 are discussed below.
Physical therapy
Physical therapy can help strengthen neck muscles, improve posture, and increase the range of motion after an injury to the C2-C5 motion segments. Physical therapy is usually performed under the guidance of a physical therapist and may include exercises, stretches, massage, and/or other treatments.
See Physical Therapy for Neck Pain Relief
Cervical traction
Traction is a therapeutic method that relieves pain by stretching and realigning the spine. The stretch is achieved manually by a therapist or by using spinal traction devices. This method opens up the neuroforamina, relieving spinal nerve compression.
Pain-relieving medication
Prescription and over-the-counter (OTC) medication may help reduce neck pain.
Taking pain-relieving medication such as non-steroidal anti-inflammatory drugs (NSAIDs), opioids, tramadol, and/or corticosteroids may help control pain from trauma and/or radiculopathy. These medications may be obtained with a prescription or over-the-counter (OTC).
Injection procedures
Cervical steroid injections and radiofrequency ablation (RFA) are minimally invasive procedures and usually considered after other nonsurgical and non-interventional methods have been tried.
Injection procedures, in general, carry a small risk of hematoma, bleeding, and/or nerve damage.
Steroid injection

Steroid injections help reduce inflammation and pain stemming from the C2-C5 spinal segments.
Steroids or anesthetic medication may be injected in the epidural space, neuroforamen, facet joints, or at the medial branch nerves supplying the facet joints. Conditions such as radicular pain from herniated discs or non-radiating pain such as that from whiplash injuries may be treated with these injections.
Watch: Cervical Epidural Steroid Injection Video
Radiofrequency Ablation
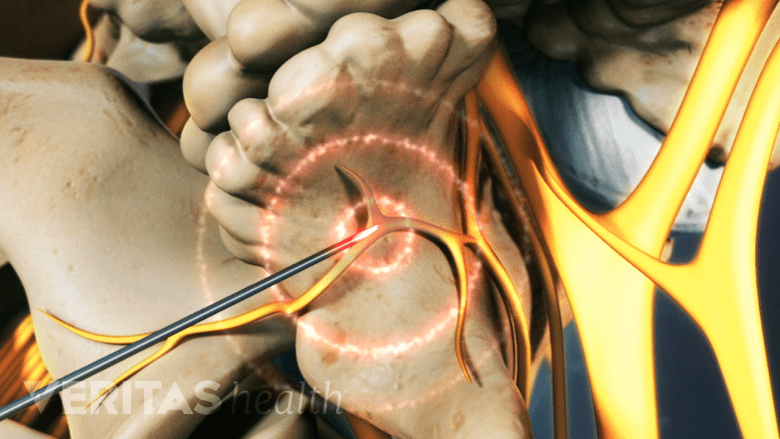
Targeted application of heat to a nerve can be used to interrupt its pain pathway.
RFA involves heating a part of the pain-transmitting nerve with a radiofrequency needle to create a heat lesion. This resulting lesion prevents the nerve from sending pain signals to the brain. RFA of medial branch nerves may help control pain transmitted from the facet joint. RFA is performed if patient responds favorably to the medial branch blocks, but does not have sustained relief after these blocks.
See Radiofrequency Ablation (RFA) for Facet and Sacroiliac Joint Pain
Other nonsurgical pain management techniques such as acupuncture, transcutaneous electrical nerve stimulation (TENS), cognitive behavioral therapy, and biofeedback may be included in the C2-C5 treatment program.
In rare cases, for injuries that do not recover with nonsurgical methods or cause progression of symptoms such as numbness and weakness in one or both arms, surgical methods may be considered.
Surgical Treatment for C2-C5
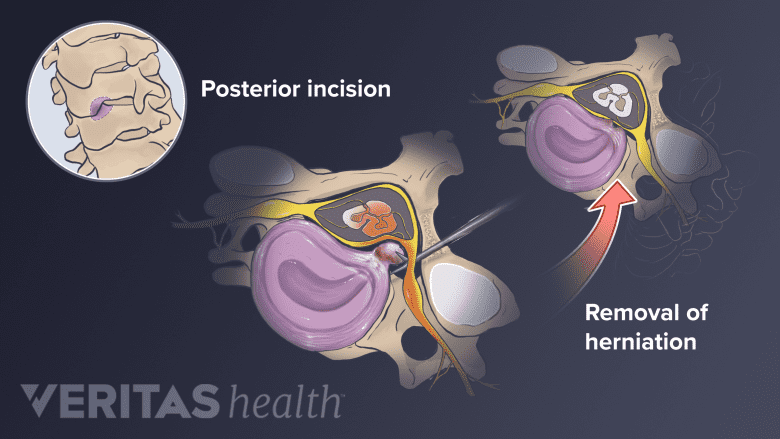
A posterior cervical decompression surgery is performed to remove a part of a herniated disc from the back of the neck.
Surgery on the C2-C5 motion segments may be performed from the front or back of the neck. Some surgeries may be performed via both approaches. 1Marcon RM, Cristante AF, Teixeira WJ, Narasaki DK, Oliveira RP, de Barros Filho TE. Fractures of the cervical spine. Clinics (Sao Paulo). 2013;68(11):1455–1461. doi:10.6061/clinics/2013(11)12.
Common surgical techniques performed in the C2-C5 motion segments include:
- Surgery to remove all or part of a disc such as anterior cervical discectomy and fusion (ACDF), cervical artificial disc replacement (ADR), and posterior cervical decompression. These surgeries typically help relieve pressure on compressed nerve roots, reducing radicular pain and at times can be utilized to reduce pain stemming from the disc itself.
- Surgery on the vertebrae such as laminectomy or foraminotomy. These surgeries include removal of portions of overgrown bone (bone spurs) and/or removing part of a vertebra may help relieve pressure on compressed nerves.
Watch: Cervical Laminectomy Video
Depending on the severity or location of the injury, one or more procedures may be performed at the same time. In many cases, symptom relief is experienced within a few weeks after surgery.
A small risk of serious complications such as excessive bleeding, allergic reaction, infection, and others may exist following these surgeries.
- 1 Marcon RM, Cristante AF, Teixeira WJ, Narasaki DK, Oliveira RP, de Barros Filho TE. Fractures of the cervical spine. Clinics (Sao Paulo). 2013;68(11):1455–1461. doi:10.6061/clinics/2013(11)12.

