Our spines are remarkable—they're made up of incredibly intricate systems of bones, ligaments, tendons, and muscles that work together to enable movement in all directions. While all of this movement is great, the potential downside is that it can contribute to injuries and wear-and-tear damage over time that may lead to back pain and stiffness.
Understanding how movement impacts your spine can help you better communicate with your physician and hopefully get an accurate diagnosis for faster treatment and pain relief. With this in mind, here are 5 common ways that motion can contribute to back pain:
1. Large spinal muscles are easily strained with twisting motions
The most common reason motion causes back or neck pain has little to do with the bones in your spine. Instead, it’s related to the muscles and ligaments that surround your spine.
When you twist your lower back, such as during a golf swing or while bending to unload grocery bags, you run the risk of overstretching or tearing any of the large muscles or supporting ligaments around your spine. In response to this damage, the surrounding area will usually become inflamed. This inflammation can lead to a back spasm , which can potentially lead to severe lower back pain.
Strains and tears in the spinal muscles and ligaments are a common cause of lower back pain.
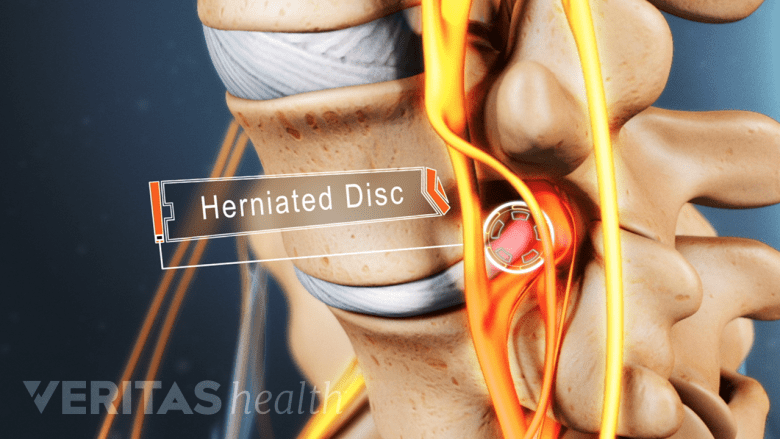
2. Lumbar spine motion can cause a disc herniation
Your lumbar spine (lower back) is constantly in motion, and it also carries the entire weight of your upper body. This makes your lumbar spine particularly prone to injuries.
See Causes of Pain in the Lumbar Spine
The motion in your lumbar spine is divided into 5 spinal motion segments. Each of these segments is made up of 2 cartilage-covered facet joints and a spinal disc that provides shock absorption and prevents adjacent vertebrae from grinding together.
Your two lowest discs (the L4-L5 and L5-S1) endure the most strain, and therefore are the most likely to become herniated.1He A, Wang WZ, Qiao PF, Qiao GY, Cheng H, Feng PY. Quantitative Evaluation of Compressed L4-5 and S1 Nerve Roots of Lumbar Disc Herniation Patietns by Diffusion Tensor Imaging and Fiber Tractography. World Neurosurgery. 2018; 115, e45-e52. doi:10.1016/j.wneu.2018.03.134 A herniation can lead to sciatic pain that radiates down your leg and to your foot.
Symptoms of a lumbar herniated disc vary widely.
3. Overuse and injuries can lead to cartilage breakdown
Repetitive motions and overuse injuries, especially for athletes, can lead to spinal osteoarthritis—or the mechanical breakdown of the cartilage between your aligning facet joints in the back portion of the spine.
See Causes of Osteoarthritis and Spinal Arthritis
When this happens, the facet joints become inflamed, and progressive joint degeneration creates more frictional pain. As your back pain progresses, the motion and flexibility of the spine decreases.
See Symptoms and Diagnosis of Facet Joint Disorders
Typical symptoms include:
- More stiffness and pain in the lower spine and sacroiliac joint in the mornings and later in the day.
- Decreased pain during the day as normal movements stir the fluid lubricant of the joints.
- Low back pain radiating to the pelvis, buttocks, or thighs—and sometimes to the groin.
While overuse and injuries can potentially accelerate the development of osteoarthritis later in life, it is important to remember that staying active is a key part of a healthy lifestyle. Check with your doctor as to which exercises are appropriate for you, and how to perform exercises safely.
Excessive motion in the spine can lead to cartilage breakdown.
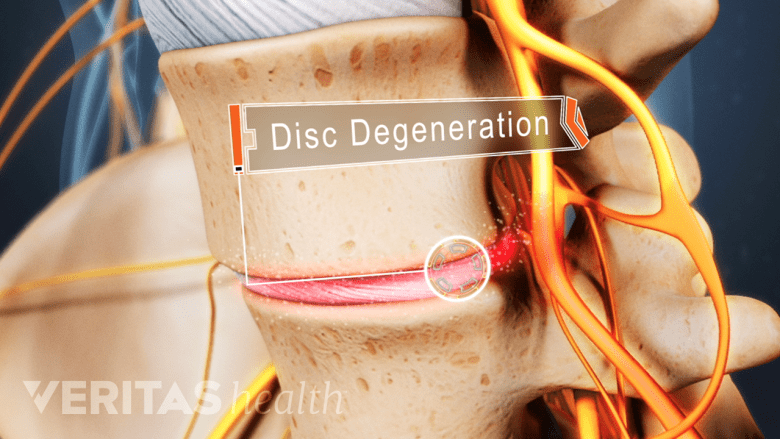
4. Disc degeneration may lead to pain from micro-motion
Disc degeneration in your spine can create excessive micro-motion at a vertebral level and lead to lower back pain, a condition termed lumbar degenerative disc disease.
Common symptoms of degenerative disc disease include:
- Low back pain that generally worsens with prolonged sitting or holding stationary positions
- Worsened pain with certain movements, such as bending, lifting, or twisting.
See Causes of Degenerative Disc Disease Pain
Potential pain relief may be experience when changing positions frequently, and lying day may be most comfortable.
Micro-motion from disc degeneration can lead to lower back pain.
5. Bone spurs can form to compensate for too much motion
Over time, excessive motion in your spine can lead to inflammation and enlarged spinal joints. When this happens, bone spurs—or small, irregular growths on the bone—typically form on your facet joints in response to joint instability from the degeneration. The bony overgrowths can eventually become big enough to reduce joint motion and cause more swelling and stiffness.
While spurs can be a normal part of aging and do not directly cause pain, they may become large enough to irritate or compress nerves passing through spinal structures. This may result in diminished room for the nerves to pass—which is referred to as spinal stenosis.
Over time, degeneration of the facet joints in your lower back can result in the formation of a fluid-filled sac called a synovial cyst. These cysts are benign, but if they put pressure on the spinal canal they can, like bone spurs, cause symptoms of spinal stenosis.
Bone spurs are a marker of spinal degeneration, and are quite common in people over the age of 60.
When discussing your back pain with a doctor, try to remember which activities make the pain better or worse. Sharing this information with your doctor may help him or her more accurately identify the specific cause of your pain.
Learn more:
- 1 He A, Wang WZ, Qiao PF, Qiao GY, Cheng H, Feng PY. Quantitative Evaluation of Compressed L4-5 and S1 Nerve Roots of Lumbar Disc Herniation Patietns by Diffusion Tensor Imaging and Fiber Tractography. World Neurosurgery. 2018; 115, e45-e52. doi:10.1016/j.wneu.2018.03.134