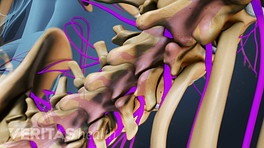
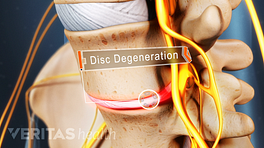
Cauda equina syndrome is a rare but serious condition that describes extreme pressure and swelling of the nerves at the end of the spinal cord.
Cauda equina syndrome is a medical emergency that calls for urgent surgical intervention.
See When Back Pain May Be a Medical Emergency
If patients with cauda equina syndrome do not receive treatment quickly, adverse results can include paralysis, impaired bladder, and/or bowel control, difficulty walking, and/or other neurological and physical problems.
Patients should be aware that acute cauda equina syndrome that results in nerve damage is extremely rare.
In This Article:
Onset of Cauda Equina Syndrome
Symptoms of cauda equina syndrome can develop suddenly, but may take weeks or months. The onset of the condition is often described using the following distinctions:
Acute onset
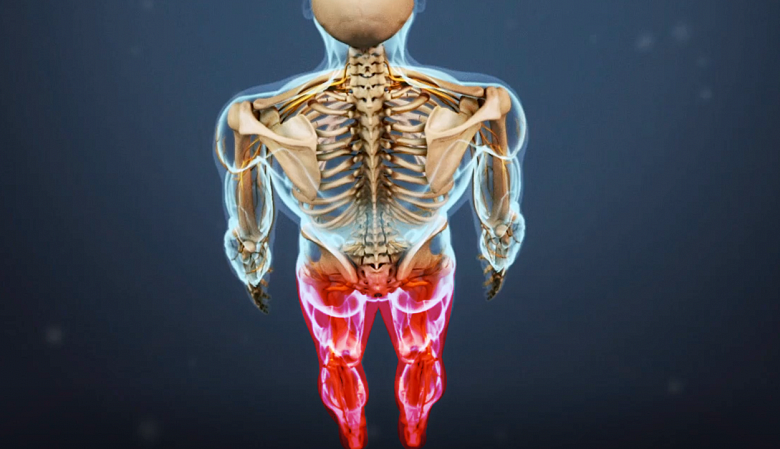
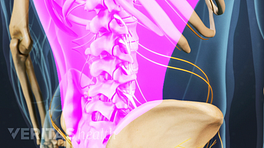
Acute cauda equina syndrome may lead to weakness and loss of sensation in one or both legs.
Acute onset is marked by a rapid development of symptoms that often includes severe low back pain and significant loss of bladder and bowel function. In an acute onset, sensory and motor deficits in the lower body typically develop within 24 hours.
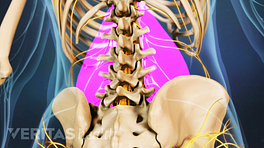
Gradual onset
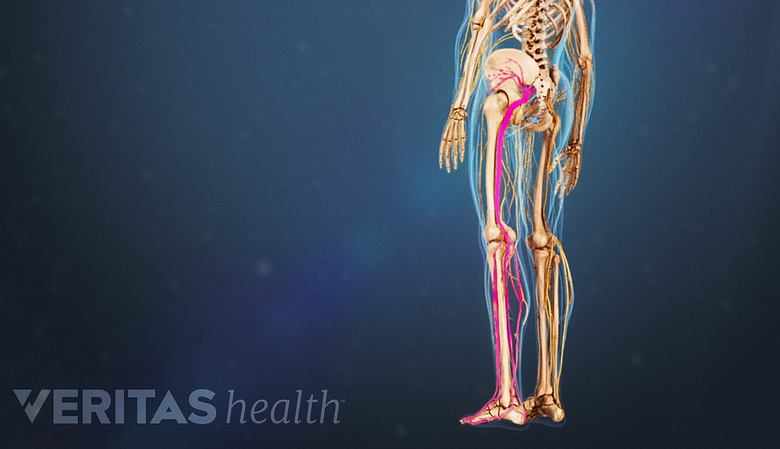
In the earlier stages, cauda equina syndrome may cause pain and numbness in one or both legs.
Symptoms can develop over progressively, and symptoms may come and go over the course of several weeks or months. Gradual onset usually typically includes partial or intermittent loss of bowel and bladder function, as well as recurring low back pain in combination with muscle weakness and numbness and bladder and/or bowel incontinence or dysfunction. Sciatica may also occur in one or both legs.
See Types of Sciatic Nerve Pain
Loss of bowel or bladder function may include incontinence (inability to retain urine or stool), and/or constipation (inability to eliminate urine or stool).
It is possible for a patient to develop cauda equina syndrome with no history of back pain, or in a patient with a long or recent history of low back pain or sciatica.
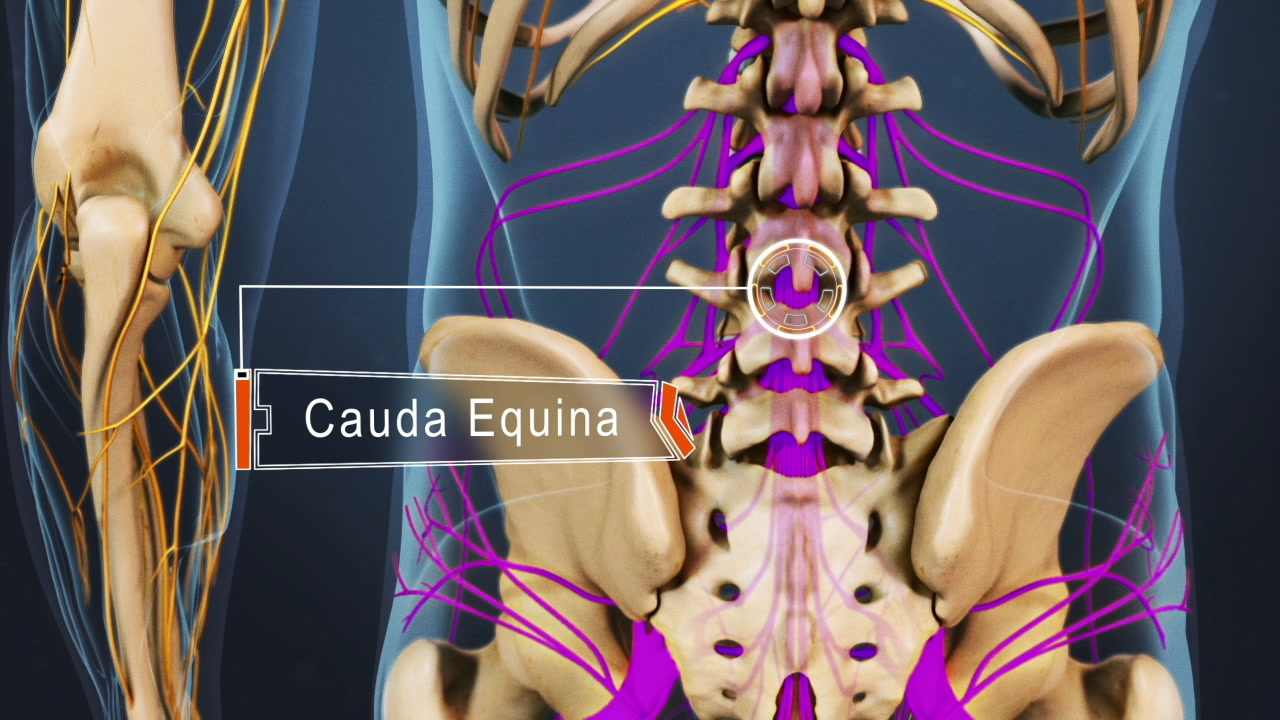
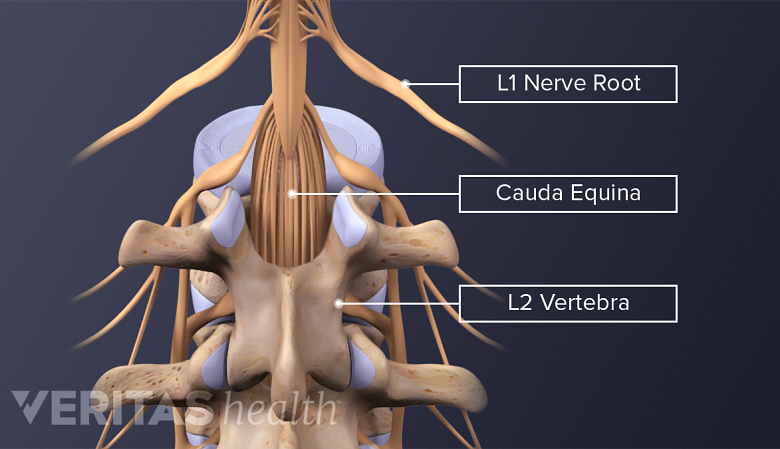
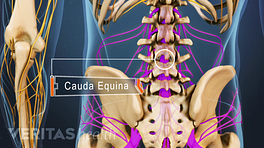
The Cauda Equina and Its Function
The cauda equina provides sensory and motor innervation to the pelvis and lower limbs.
The cauda equina gets its name from Latin for "horse’s tail," because the nerves at the end of the spine visually resemble a horse’s tail as they extend from the spinal cord, through the lumbar spine and over the sacrum, and down the back of each leg.
The cauda equina consists of about 10 pairs of nerve roots, some of which combine to form larger nerves in the lower body—one example of which is the sciatic nerve.
The cauda equina is responsible for sensory and motor innervation to the pelvis and lower limbs, as well as bowel and bladder function. If the cauda equina is damaged by inflammation or compression in the low back, symptoms may be severe and may develop quickly. Early medical attention and treatment are crucial for making as full a recovery as possible.