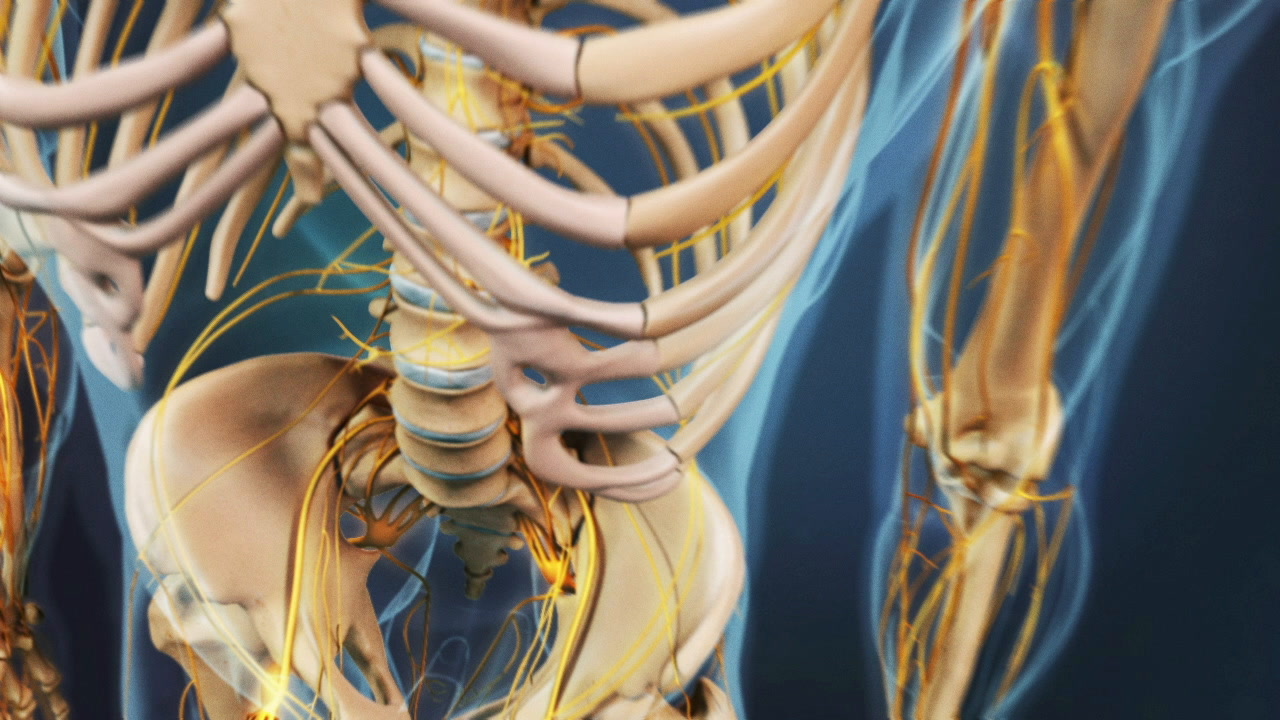
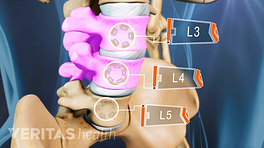
Disc degeneration is not a problem most people associate with adolescents and young adults, but it can develop at a young age. Called juvenile disc disorder, or juvenile discogenic disorder, it usually leads to pain in the lower back.
The disorder generally affects young people in their late teens to early 30s. Sometimes an injury is to blame, but the medical community is divided about other causes. Many doctors believe a genetic disposition to disc degeneration is a major factor. Others cite wear and tear on the body as the main cause.
See Common Symptoms of Degenerative Disc Disease
How Schmorl's Nodes and Juvenile Disc Disorder Develop
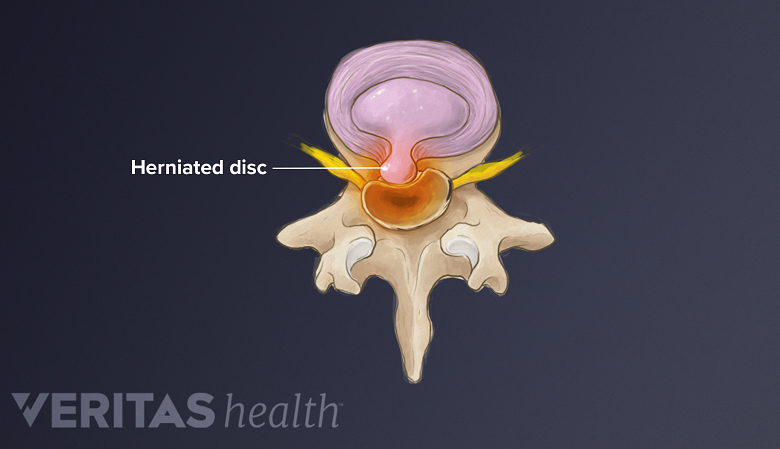
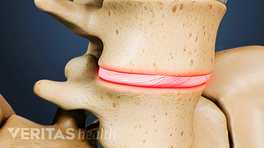
Juvenile disc disease occurs when the end plates cannot withstand spinal pressures.
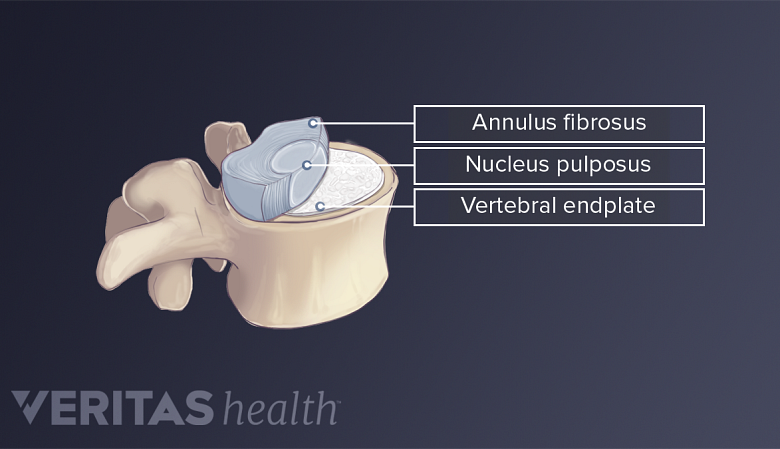
Juvenile disc disorder occurs when the parts of the vertebrae called end plates are too weak to withstand the pressures inside the disc spaces. The end plates are the very top and bottom portions of the vertebrae that attach to the cartilaginous disc between each vertebra.
See Lumbar Spine Anatomy and Pain
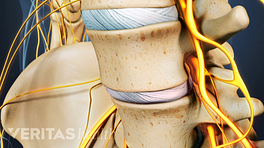
When the end plates of the vertebrae are weak, portions of the tough cartilage of the disc may the protrude into the end plate, and potentially into the vertebra. These protrusions are called Schmorl’s nodes and can be a cause of pain.
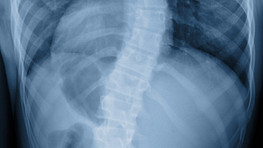
Juvenile disc disorder shares many similarities with disc degeneration in older adult patients, but also an important difference. Unlike older adult patients who usually experience degeneration in one or two discs, those with juvenile disc disorder usually have degeneration in all or most of the lumbar discs.
Juvenile disc disorder serves as a reminder that back pain in young adults should always be medically evaluated. If the individual is an adolescent, parents should ask him or her to be as specific as possible about where it hurts and what activities make it worse. The individual should see a doctor as soon as possible. Untreated back pain can lead to degenerative disc disease, which can limit future physical activities. Juvenile disc disorder treatments are typically less invasive when begun soon after symptoms develop.
Juvenile Disc Disorder Symptoms
Lifting heavy objects can cause pain at the site of disc damage.
Continuing pain in the back and neck is common, and may be felt at the site or sites of the disc damage. These are other common signs of juvenile disc disorder:
- Pain goes away with rest, but increases after sitting for long periods
- Running, walking, or often changing positions eases the pain
- Pain increases when twisting, picking up heavy objects, or bending over
- Pain radiates to other areas
Nonsurgical Treatment Options
Nonsurgical treatments are usually recommended first for people with juvenile disc disorder. A wide variety of treatments are available, and often it is a process of trial and error to see what is most effective in managing the pain.
Exercise
Exercise aims to strengthen muscles in the abdomen and lower back.
People with juvenile disc disorder don’t need to restrict their physical activities, and can participate in sports unless that causes pain. A balanced exercise program including daily hamstring stretches, strength training, and aerobic conditioning is best.
See Specific Hamstring Stretches for Back Pain Relief
Exercise helps build up the core muscles in the abdomen and back and enhances circulation, which helps with overall spine health. Adolescents who are inactive have a higher rate of back pain because they become deconditioned and weaker.
Treatment may include targeted exercises, including physical therapy. In addition to developing an individualized plan of exercises, physical therapists can be helpful in teaching patients about “body mechanics,” the best body movements and postures to avoid pain. A physical therapist is also a good resource on how to set up an ergonomic work area.
Other treatments
Other interventions may be helpful in easing discomfort, including:
- Using hot packs or heating pads
- Application of ice or cold packs to alleviate pain after activity
- Pain relievers and/or anti-inflammatory medications
- Massage
- Transcutaneous Electrical Nerve Stimulation (TENS)
- Epidural steroid injections
When Surgery Is Considered For Juvenile Disc Disorder
Microdiscectomy may be indicated for a herniated disc compressing the nerve root.
Because the degeneration typically occurs in multiple discs, generally a multi-level fusion would be needed. As a general rule, multi-level fusions are best avoided, as fusing multiple levels of the spine is an extensive surgery and changes the natural biomechanics of the spine—which can in and of itself lead to more pain.
If a disc herniation is compressing a nerve root, however, surgery may be advisable. This type of surgery is called a microdiscectomy. It is a much less invasive surgery and can relieve pain without changing the natural biomechanics of the spine.
See How Microdiscectomy Surgery Is Performed
Because of the age of many patients with this disorder, doctors may discuss patients’ long-term vocational plans. A doctor may suggest people with this condition avoid occupations that involve heavy manual labor, if possible. Such jobs might not make the degeneration worse, but could lead to bouts of low back pain and difficulty in performing such work.
Read more about the causes of Back Pain in Children