Degenerative scoliosis, also known as adult onset scoliosis, describes a side-to-side curvature of the spine caused by degeneration of the facet joints and intervertebral discs which are the moving parts of the spine. This degeneration and resulting spinal asymmetry can occur slowly over time as a person ages. This is a completely different cause of scoliosis from the standard adolescent onset scoliosis.
If degenerative scoliosis becomes symptomatic, pain can range from a dull back ache to excruciating sensations that shoot down the leg, commonly referred to as sciatica, and make walking difficult or impossible.
In This Article:
- All About Degenerative Scoliosis
- Degenerative Scoliosis Symptoms and Diagnosis
- Treatment for Degenerative Scoliosis
- Surgery for Degenerative Scoliosis
- Degenerative Scoliosis Video
How Degenerative Scoliosis Develops
Asymmetric degenerative changes, such as osteoarthritis, are a risk factor for scoliosis.
When healthy, facet joints are like hinges that help the spine bend smoothly, and intervertebral discs are like cushions that absorb shock between vertebral bones. Everyone experiences natural degeneration of these joints and discs due to aging—the same processes that cause osteoarthritis and degenerative disc disease—but for some people these degenerative processes are accelerated and/or cause more symptoms.
See Facet Joint Disorders and Back Pain
If degeneration is more pronounced on one side of the spine, degenerative scoliosis can result. The degenerative scoliosis curve, which is often located in the low back (lumbar spine), forms a slight "C" shape as the spine abnormally curves on one side or the other. Any sideways spinal curve of at least 10 degrees, as measured by the Cobb angle on spinal radiographs (X-rays), is considered scoliosis.
See Scoliosis: Symptoms, Treatment and Surgery
Pain From Degenerative Scoliosis
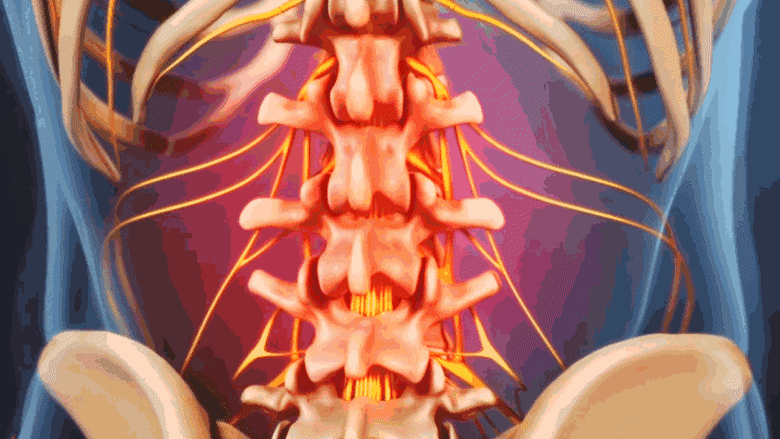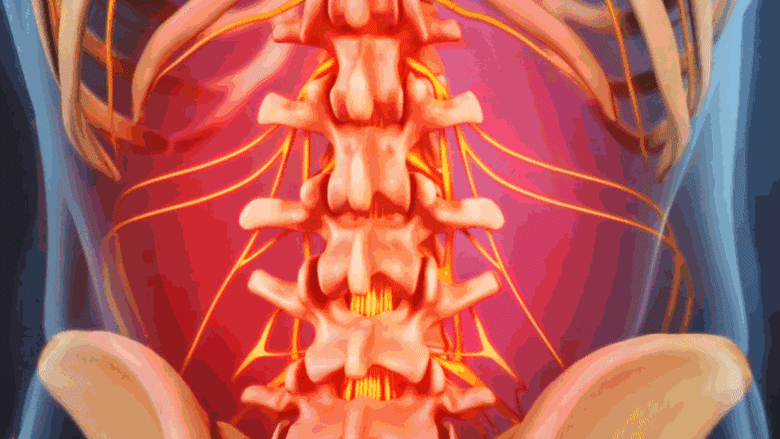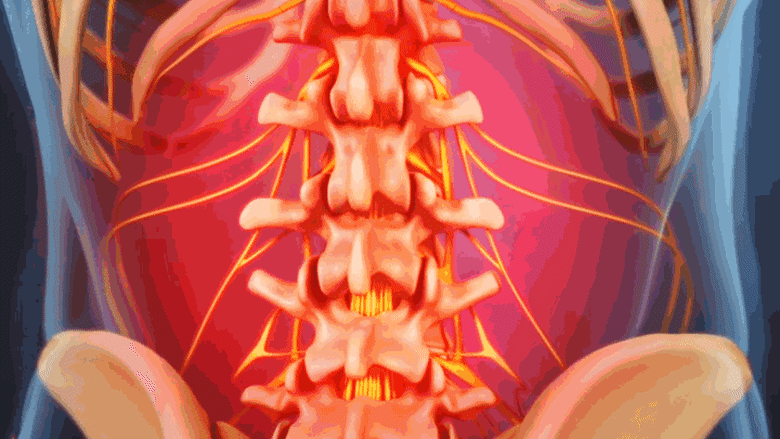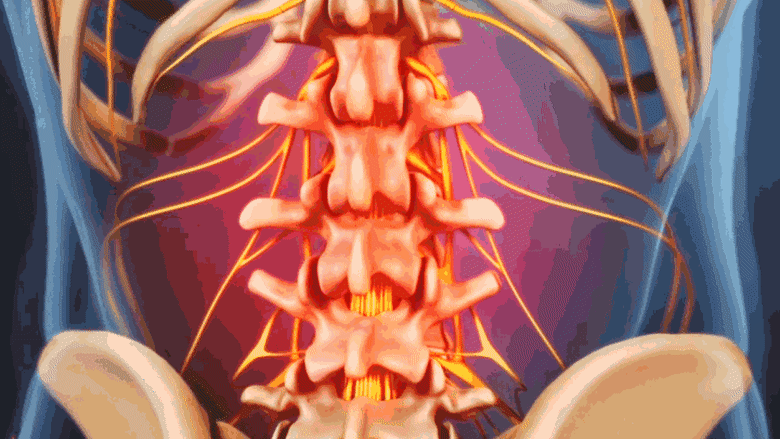
Degenerative scoliosis causes a dull ache or stiffness in the lower back.
Painful symptoms of degenerative scoliosis are similar to lumbar osteoarthritis and/or lumbar degenerative disc disease because they are all part of the same degenerative process. Degenerative scoliosis can trigger the following types of discomfort:
- Dull ache or stiffness in the mid to low back
- Shock-like back pain that can radiate down the buttock and into the leg
- Pins-and-needles tingling and/or numbness that can radiate down the buttock and into the leg
- Sharp leg pain that develops while walking but subsides with rest
It should be noted that spinal joint inflammation or nerve impingement is the main source of degenerative scoliosis pain, not the abnormal sideways curvature of the spine.
The Course of Degenerative Scoliosis
It is difficult to determine exactly how many people have degenerative scoliosis because many cases never cause significant symptoms and go undetected. However, one study estimated at least 60% of the population over age 60 has at least mild degenerative scoliosis.1Schwab F, Dubey A, Gamez L, El Fegoun AB, et al. Adult scoliosis: prevalence, SF-36, and nutritional parameters in an elderly volunteer population. Spine. 2005; 30(9): 1082-5.
If degenerative scoliosis becomes symptomatic, the pain typically starts gradually. Early symptoms are most commonly a dull ache or stiffness in the mid to low back that comes and goes. Nonsurgical treatment options—such as physical therapy, medications, or avoiding strenuous activities—are usually sufficient.
In rare cases, scoliosis surgery may be considered when the pain persists or is negatively affecting quality of life despite multiple treatment efforts. Although, given the population with symptomatic degenerative scoliosis trends toward age 65 and older, some people should still avoid the surgery due to other age-related risk factors, such as having fragile bones or a weakened heart.
When Adult Scoliosis Means Degenerative Scoliosis
Sometimes there is confusion over the term “adult scoliosis” because it is commonly used to refer to the following two types of scoliosis:
- Degenerative scoliosis. This type of scoliosis usually starts after age 50 as the spine continues to naturally degenerate, or wear out, due to aging. Technically, this is also known as adult onset scoliosis, but many people just shorten that and say adult scoliosis.
- Idiopathic scoliosis. This type of scoliosis, which has no known cause, typically begins during adolescence. It is often called adolescent idiopathic scoliosis or just adolescent scoliosis. While the condition can start during adolescence, it might not be caught or diagnosed until the curve becomes problematic for the person, which sometimes happens later in adulthood. Even though a case could technically be idiopathic scoliosis, it might be referred to as adult scoliosis if the person getting treatment is an adult.
The term adult scoliosis technically refers to any scoliosis in a skeletally mature patient. While knowing exactly what someone means when they say adult scoliosis is usually unimportant in casual conversation, understanding the patient’s exact type of adult scoliosis is critical for determining an effective treatment plan.
When Degenerative Scoliosis Is Serious

Rarely, degenerative scoliosis causes loss of bowel and bladder control.
If degenerative scoliosis causes the spinal cord or a nerve root to become impinged, either through stenosis (narrowing of the spinal canal) or severe bending of the spine, nerve function could be jeopardized. Initially, this is often felt as a sharp or shock-like pain in the back that can radiate down the buttock and/or into the leg, or as tingling or numbness that can radiate down into the leg. This is commonly referred to as sciatica or sciatic pain. The medical term for this type of radiating pain is radiculopathy. While unlikely, it is possible for degenerative scoliosis to cause permanent leg weakness or problems with bladder/bowel control.
- 1 Schwab F, Dubey A, Gamez L, El Fegoun AB, et al. Adult scoliosis: prevalence, SF-36, and nutritional parameters in an elderly volunteer population. Spine. 2005; 30(9): 1082-5.

