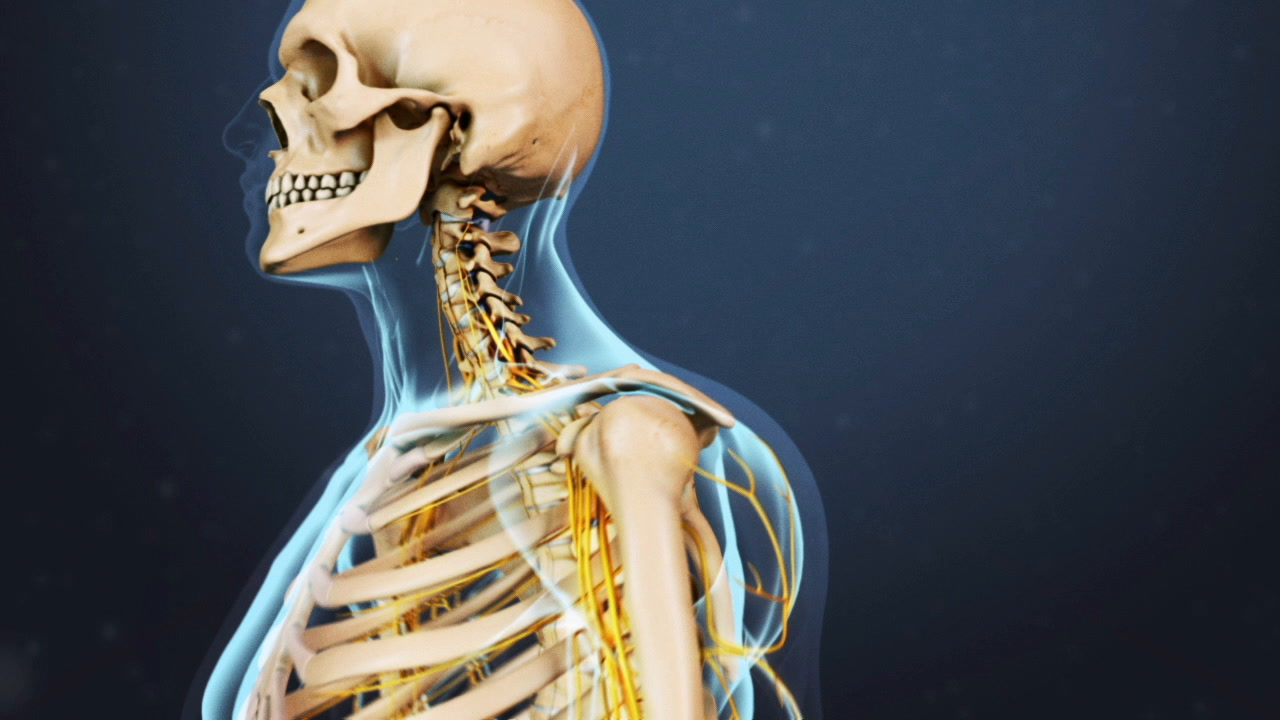
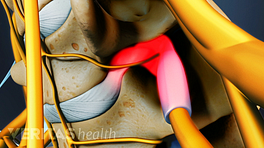
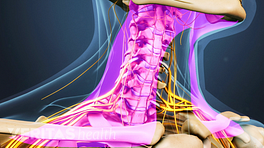
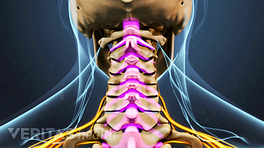
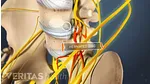
Over time, degenerative changes to the cervical vertebrae, discs and joints may have significant effects on the spinal cord, which runs from the brain through the cervical spine and thoracic spine before branching off to other parts of the body.
Cervical stenosis is one such degenerative condition that may affect the spinal cord and lead to compromised coordination of the extremities. When diagnosing cervical stenosis, doctors must determine whether progressive dysfunction (myelopathy) is present as a result of the spinal cord compression.
See Cervical Stenosis with Myelopathy
While extremely rare, progressive cases of cervical stenosis with myelopathy may result in weakness and paralysis, thus making accurate diagnosis and treatment especially important.
In This Article:
- Spinal Cord Compression and Dysfunction from Cervical Stenosis
- Cervical Spinal Stenosis Video
Symptoms of Spinal Cord Compression and Dysfunction
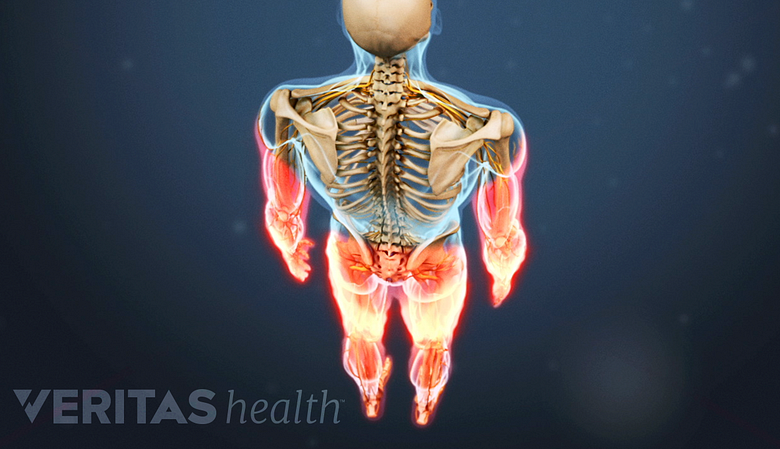
Cervical stenosis with myelopathy causes pain and weakness in both upper and lower limbs.
It's important to know that in many cases cervical stenosis is asymptomatic, meaning that the spinal cord is compressed but the patient is not experiencing any of the common symptoms. In these cases, the patient may simply be monitored to ensure that the spinal cord continues to function normally and that myelopathy (i.e. spinal cord dysfunction) does not develop as a result of the compression.
In other situations, cervical stenosis with myelopathy may present itself in symptoms that include a heavy feeling in the arms and legs, cervical pain that is referred to the arm, shooting pains in the arms and legs, and/or difficulty walking and performing activities involving fine motor skills (handwriting, buttoning a shirt, etc.)
When cervical stenosis with myelopathy is present, the spinal cord - specifically the long tracts that run inside it - is affected, possibly leading to impaired or abnormal functioning that may be observed during a physical examination, including:
- Increased muscular tone in the legs. Muscle tone refers to the amount of tension or resistance to movement in a muscle; increased muscle tone may make it difficult to make certain movements, like walking and moving one foot in front of the other (tandem walking).
- Hyperreflexia. Heightened deep tendon reflexes in the knee and ankle are potential indicators of spinal cord compression and dysfunction.
- Clonus. Upon forcing the ankle to extend, the patient's foot rapidly beats up and down.
- Babinski reflex. When scratching the sole of the foot, the big toe moves up rather than down (the normal movement), most often prompting a closer examination of the spinal cord.
- Hoffman's reflex. Upon flicking the middle finger, the thumb and middle finger flex.
-
Since cervical stenosis with myelopathy is typically related to some sort of spinal cord instability, various diagnostic tests may be conducted to get a closer examination of the spine.
Diagnosis and Treatment of Spinal Cord Dysfunction
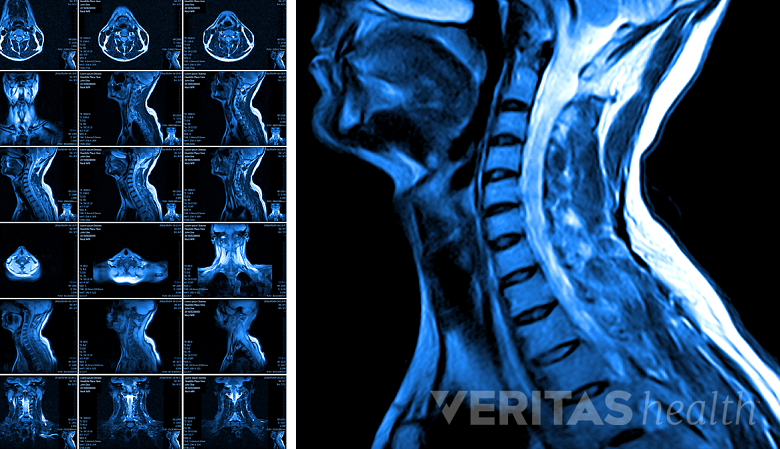
MRI scan is a useful tool in diagnosing spinal cord compression and dysfunction.
An MRI scan, a CT with myelogram, lateral cervical spine X-rays, and electrical studies called Somatosensory Evoked Potentials (SSEP) are some tests that may be used to further confirm the spinal cord compression and dysfunction.
In order to stop the progressive dysfunction of the spinal cord and restore the patient's neurological condition, cervical spine surgery that decompresses the spinal canal is typically needed.