Surgery to address degenerative disc disease is usually only recommended if pain is severe and nonsurgical treatments, such as pain medications and physical therapy, are ineffective. The goal of surgery is to alter the underlying mechanisms in the spine causing pain, such as excessive micro-motion, inflammation, and/or muscle tension.
Surgery may eventually be considered for degenerative disc disease.
Nonsurgical treatments are typically suggested for no less than 6 to 12 weeks before surgery is considered, although in most cases nonsurgical treatments are used for much longer. It is estimated that only between 10% and 20% of lumbar disc degeneration cases and up to 30% of cervical disc degeneration cases are not successfully treated using nonsurgical methods, and warrant surgery to relieve pain and improve mobility.1Healthy Quality Ontario. Artificial Discs for Lumbar and Cervical Degenerative Disc Disease –Update: An Evidence-Based Analysis. Ontario Health Technology Assessment Series. 2006;6(10):1-98.
Prior to deciding whether to have surgery for degenerative disc disease, patients should consider the risks and benefits.
In This Article:
- What Is Degenerative Disc Disease?
- Causes of Degenerative Disc Disease Pain
- Common Symptoms of Degenerative Disc Disease
- Degenerative Disc Disease Treatment Guidelines
- Surgical Treatments for Degenerative Disc Disease
- Lumbar Degenerative Disc Disease Video
Considerations Before Spine Surgery
There are several factors to consider before opting for surgical treatment if it is recommended, including:
- Recovery process. The recovery period following spinal surgery can consist of a combination of physical therapy, pain medications, or wearing a back or neck brace
- Lifestyle considerations. The everyday lifestyle changes needed for either nonsurgical or surgical treatment may be considerable. In the case of surgery, a long recovery process may require significant time off from work. Additionally, regular physical therapy, and pain management will be required for optimal results.
- Imaging evidence of disc degeneration. Spinal surgery for degenerative disc pain is typically only recommended if an imaging scan correlates to the specific cause of pain, and even then outcomes are not always predictable.
Spinal surgery is always elective, meaning it is the patient’s choice whether or not to have the procedure. A spinal fusion is the most common procedure used for degenerative disc pain. In recent years, artificial disc replacement has become more widely used as devices and surgical methods have improved.
Spinal Fusion for Degenerative Disc Disease

A fused joint eliminates instability and reduces pain caused by micro-motions.
During a spinal fusion surgery, two adjacent vertebrae are grafted together to alter the underlying mechanisms causing pain. A fused joint eliminates instability at a spinal segment, reducing pain caused by micro-motions, muscle tension, and/or inflammation. Joint fusion can also allow for a more thorough decompression of pinched nerves.
A spinal fusion procedure typically consists of the following steps:
- Under general anesthesia, an incision is made to approach the spine. For a cervical fusion, the incision is usually made in the front of the neck. For a lumbar fusion, an incision may be made in the back, front, or side of the body.
- Muscles surrounding the spine are cut away or pushed to the sides to access the spine.
- The degenerating disc is removed from the disc space.
- A bone graft and/or instruments are implanted across the disc space to stabilize the spinal segment and encourage bone growth.
- The spinal muscles are replaced or reattached, and the incision site is closed with sutures.
A fusion surgery sets up the mechanisms for bone growth, and the fusion occurs in the months following the procedure. For this reason, the complete recovery process from a fusion surgery can last up to a year, although a majority of patients are back to their regular activities within six weeks.
See Spinal Fusion Surgery Recovery: 1 to 3 Months After
Following surgery, use of a back or neck brace may be advised to keep the spine stabilized and to minimize painful movements that can undermine the healing process. Additionally, physical therapy is usually recommended to condition the muscles to better support the spine, and pain medications are prescribed to manage post-surgical pain.
Artificial Disc Replacement Surgery

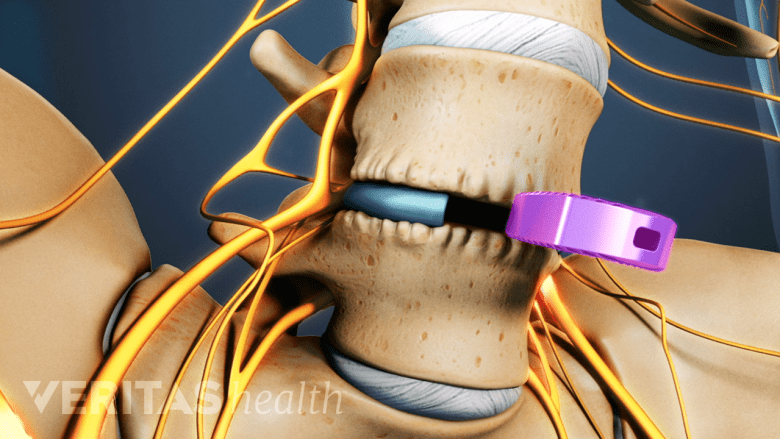
Replacing the degenerated disc with an artificial disc preserves motion.
Degenerative disc pain can also be significantly reduced or eliminated by implanting a device that mimics the natural support and motion of a spinal disc in a procedure called Artificial Disc Replacement (ADR). Unlike a spinal fusion, this procedure is intended to maintain motion at a spinal segment after surgery.
In this procedure:
- The spine is approached through a small incision under general anesthesia. During a cervical ADR, the incision is usually made in the front of the neck; during a lumbar ADR, the incision is usually made in the back directly over the spine.
- The muscles are moved to the side or cut away from the spine.
- The degenerated disc is removed entirely, as is any degenerated portions of the spinal joints or adjacent vertebrae in the disc space.
- The artificial disc is inserted into the disc space using x-ray imaging to guide the device. Some devices also include metal plates that are attached to either vertebrae facing the disc space.
- The muscles surrounding the spine are reattached, and the wound is closed.
Artificial discs are typically made of metal or plastic materials. The recovery process from an artificial disc replacement usually consists of a combination of pain medications, physical therapy, and possibly wearing a back or neck brace. Recovery from this procedure can take up to 6 months.
See Lumbar Artificial Disc Surgery Recovery and Recovery from Cervical Artificial Disc Replacement Surgery
- 1 Healthy Quality Ontario. Artificial Discs for Lumbar and Cervical Degenerative Disc Disease –Update: An Evidence-Based Analysis. Ontario Health Technology Assessment Series. 2006;6(10):1-98.

