Persistent or newly developed pain in the lower back after pregnancy, also known as postpartum back pain, usually lasts for 6 months but may continue up to a decade.1Bergström C, Persson M, Nergård KA, Mogren I. Prevalence and predictors of persistent pelvic girdle pain 12 years postpartum. BMC Musculoskelet Disord. 2017;18(1):399. Published 2017 Sep 16. doi:10.1186/s12891-017-1760-5,2Stuber KJ, Wynd S, Weis CA. Adverse events from spinal manipulation in the pregnant and postpartum periods: a critical review of the literature. Chiropr Man Therap. 2012;20:8. Published 2012 Mar 28. doi:10.1186/2045-709X-20-8 Postpartum back pain mostly occurs while performing activities that involve body movements,3Mogren IM. Physical activity and persistent low back pain and pelvic pain post partum. BMC Public Health. 2008;8:417. Published 2008 Dec 22. doi:10.1186/1471-2458-8-417 such as walking, lifting, bending, and/or carrying the new baby, and may be relieved with rest, exercise, and home treatments. The type and severity of pain depend on the underlying cause.
In This Article:
Causes of Postpartum Back Pain
The vast majority of women who experience postpartum back pain develop the symptoms due to pregnancy-related changes in the musculoskeletal system that persist after delivery. In some cases, women may undergo bodily trauma during childbirth that directly involves the lower back and pelvic bones, joints, and/or soft tissues, causing additional pain and discomfort. The type of delivery—vaginal, instrumental, or cesarean section (C-section) may also have a role to play in postpartum back pain.4Ricci SS, Kyle T. Maternity and Pediatric Nursing. Lippincott Williams & Wilkins; 2009.
Loss of muscle tone and joint instability
The effects of pregnancy on the muscles and joints in the lower body vary. A surge in the levels of relaxin, estrogen, and progesterone hormones causes considerable joint relaxation during pregnancy. After delivery, the levels of these hormones decline significantly, causing the joints to return to the pre-pregnant state. It takes an average of 6 to 8 weeks for the joints and surrounding tissues to stabilize and bear weight effectively.4Ricci SS, Kyle T. Maternity and Pediatric Nursing. Lippincott Williams & Wilkins; 2009.
The sudden decrease in hormone levels may cause localized and/or overall effects, such as4Ricci SS, Kyle T. Maternity and Pediatric Nursing. Lippincott Williams & Wilkins; 2009.:
- A general feeling of tiredness
- Activity intolerance
- Pain in the lower back and hip
- Back pain while walking or performing an exercise
If unsupported posture and body mechanics are used at this time, the risk of further trauma to the lower back and hip are higher.4Ricci SS, Kyle T. Maternity and Pediatric Nursing. Lippincott Williams & Wilkins; 2009.
Diastasis recti
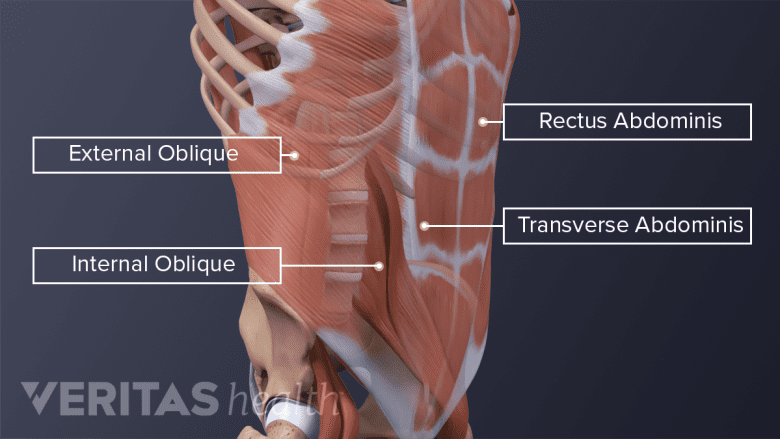
Poor abdominal muscle tone prior to pregnancy increases the risk of muscle separation after delivery.
The uterus enlarges during pregnancy to accommodate the growing fetus. This change causes the muscles of the abdominal wall to stretch substantially. The stretching results in loss of muscle tone in the abdominal region with the possible separation of certain muscles, such as the rectus abdominis. Women who have poor abdominal muscle tone prior to pregnancy are at a higher risk of separation of the rectus abdominis muscle. This condition is called diastasis recti and causes the muscles to become loose and have poor tone after delivery.4Ricci SS, Kyle T. Maternity and Pediatric Nursing. Lippincott Williams & Wilkins; 2009.
Diastasis recti may compromise postural stability and contribute to lower back and pelvic pain. If the pelvic floor muscles are also weak, urinary incontinence and dysfunction of the pelvic muscles may also occur. 5Doubkova L, Andel R, Palascakova-Springrova I, Kolar P, Kriz J, Kobesova A. Diastasis of rectus abdominis muscles in low back pain patients. BMR. 2018;31(1):107-112. doi:10.3233/BMR-169687
Posterior pelvic pain (pelvic girdle pain)
Pelvic changes begin during pregnancy and while these changes resolve uneventfully in some women, others develop chronicity due to persistent symptoms, which may last for several months to years.1Bergström C, Persson M, Nergård KA, Mogren I. Prevalence and predictors of persistent pelvic girdle pain 12 years postpartum. BMC Musculoskelet Disord. 2017;18(1):399. Published 2017 Sep 16. doi:10.1186/s12891-017-1760-5
New mothers with posterior pelvic pain experience a continuous, dull pain in the lower back. Some women have more intense symptoms, such as sharp and stabbing pain.1Bergström C, Persson M, Nergård KA, Mogren I. Prevalence and predictors of persistent pelvic girdle pain 12 years postpartum. BMC Musculoskelet Disord. 2017;18(1):399. Published 2017 Sep 16. doi:10.1186/s12891-017-1760-5
Bruising, fracture, or dislocation of the coccyx

Rarely, the coccyx is forced backward beyond its normal range of motion during childbirth, causing increased pain.
Coccydynia, the medical term for tailbone pain, is a condition that may affect women who have a difficult vaginal delivery due to a large newborn, excessive weight gained during pregnancy, or an instrumental delivery.
See Coccydynia (Tailbone Pain)
The coccygeal segment forms the bottommost part of the spine, and this segment may be forced backward beyond its normal range of motion during childbirth.6Foye PM. Coccydynia. Physical Medicine and Rehabilitation Clinics of North America. 2017;28(3):539-549. doi:10.1016/j.pmr.2017.03.006,7Lirette LS, Chaiban G, Tolba R, Eissa H. Coccydynia: an overview of the anatomy, etiology, and treatment of coccyx pain. Ochsner J. 2014;14(1):84–87. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3963058/ While this condition is self-limiting and resolves itself in a few weeks or months, the symptoms can be debilitating.
Coccydynia causes severe pain at the very bottom of the spine and makes activities such as getting up from a chair or bed painful.
Read more about Coccydynia (Tailbone Pain) Symptoms
Sacral stress fracture
Similar to tailbone trauma, the fused vertebrae of the sacral spine in the pelvic region may undergo stress fracture during childbirth. In addition to the risk factors for coccydynia mentioned above, a sacral stress fracture may also occur due to increased curvature in the lower back, the use of blood-thinning agents, such as heparin, or osteoporosis of pregnancy.8Roller RL, Walker EA, Michelitch SW. Postpartum sacral fracture in a 30-year-old female. Radiol Case Rep. 2015;4(3):264. Published 2015 Dec 7. doi:10.2484/rcr.v4i3.264
Sacral stress fractures cause severe pain in the rear pelvic region and make weight-bearing in this region painful.8Roller RL, Walker EA, Michelitch SW. Postpartum sacral fracture in a 30-year-old female. Radiol Case Rep. 2015;4(3):264. Published 2015 Dec 7. doi:10.2484/rcr.v4i3.264 For example, sitting may be notably uncomfortable.
When to See a Doctor
Leg numbness, weakness, or worsening of prior symptoms require immediate medical attention.
Back pain that does not subside with rest or home treatments, such as a massage, heat therapy, or gentle stretching and exercise, and/or pain that progresses over time may require medical attention. As a general rule, troubling symptoms, such as newly occurring numbness or weakness in the leg(s) or worsening of previous leg pain and numbness symptoms, must be reported to a doctor.
See Management of Back Pain in Pregnancy
A doctor can accurately diagnose the underlying cause of the pain and formulate a treatment plan. For breastfeeding mothers, it is advisable to consult a doctor before taking any pain-relieving medication. The type and dosage of pain-relieving medications vary, and not all over-the-counter medications are safe while breastfeeding.
Postpartum back pain may be a continuing symptom of pregnancy or develop as a new symptom after labor and delivery.9Schwerla F, Rother K, Rother D, Ruetz M, Resch K-L. Osteopathic Manipulative Therapy in Women With Postpartum Low Back Pain and Disability: A Pragmatic Randomized Controlled Trial. J Am Osteopath Assoc. 2015;115(7):416. doi:10.1097/gco.0b013e3283404ea110.7556/jaoa.2015.087 Failure to adequately treat the symptoms may lead to chronic pain, affect daily functioning, and reduce the overall quality of life. Women are encouraged to seek medical attention to relieve the symptoms and address the underlying problem. Having a pain-free back after labor and delivery will help new mothers care for their newborn more effectively and enjoy the early phases of motherhood.
- 1 Bergström C, Persson M, Nergård KA, Mogren I. Prevalence and predictors of persistent pelvic girdle pain 12 years postpartum. BMC Musculoskelet Disord. 2017;18(1):399. Published 2017 Sep 16. doi:10.1186/s12891-017-1760-5
- 2 Stuber KJ, Wynd S, Weis CA. Adverse events from spinal manipulation in the pregnant and postpartum periods: a critical review of the literature. Chiropr Man Therap. 2012;20:8. Published 2012 Mar 28. doi:10.1186/2045-709X-20-8
- 3 Mogren IM. Physical activity and persistent low back pain and pelvic pain post partum. BMC Public Health. 2008;8:417. Published 2008 Dec 22. doi:10.1186/1471-2458-8-417
- 4 Ricci SS, Kyle T. Maternity and Pediatric Nursing. Lippincott Williams & Wilkins; 2009.
- 5 Doubkova L, Andel R, Palascakova-Springrova I, Kolar P, Kriz J, Kobesova A. Diastasis of rectus abdominis muscles in low back pain patients. BMR. 2018;31(1):107-112. doi:10.3233/BMR-169687
- 6 Foye PM. Coccydynia. Physical Medicine and Rehabilitation Clinics of North America. 2017;28(3):539-549. doi:10.1016/j.pmr.2017.03.006
- 7 Lirette LS, Chaiban G, Tolba R, Eissa H. Coccydynia: an overview of the anatomy, etiology, and treatment of coccyx pain. Ochsner J. 2014;14(1):84–87. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3963058/
- 8 Roller RL, Walker EA, Michelitch SW. Postpartum sacral fracture in a 30-year-old female. Radiol Case Rep. 2015;4(3):264. Published 2015 Dec 7. doi:10.2484/rcr.v4i3.264
- 9 Schwerla F, Rother K, Rother D, Ruetz M, Resch K-L. Osteopathic Manipulative Therapy in Women With Postpartum Low Back Pain and Disability: A Pragmatic Randomized Controlled Trial. J Am Osteopath Assoc. 2015;115(7):416. doi:10.1097/gco.0b013e3283404ea110.7556/jaoa.2015.087

