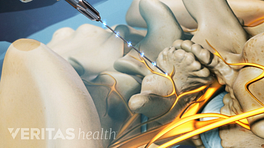
Basivertebral nerve ablation involves inserting a thin radiofrequency probe into the vertebral body to create a heat lesion on the basivertebral nerve.
Patients typically do not feel pain during the procedure due to the use of local anesthesia and/or sedation. Moderate conscious sedation or general anesthesia can be utilized for this procedure depending on patient and provider preference. 1 Sayed D, Naidu RK, Kiran Klaus Patel, et al. Best Practice Guidelines on the Diagnosis and Treatment of Vertebrogenic Pain with Basivertebral Nerve Ablation from the American Society of Pain and Neuroscience. 2022;Volume 15:2801-2819. doi:10.2147/jpr.s378544 , 2 Tieppo Francio V, Sayed D. Basivertebral Nerve Ablation. [Updated 2023 May 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK572127/
The procedure is performed in an ambulatory surgery center or a hospital’s outpatient department, and most patients can return home the same day. 1 Sayed D, Naidu RK, Kiran Klaus Patel, et al. Best Practice Guidelines on the Diagnosis and Treatment of Vertebrogenic Pain with Basivertebral Nerve Ablation from the American Society of Pain and Neuroscience. 2022;Volume 15:2801-2819. doi:10.2147/jpr.s378544
The procedure is well-tolerated by most patients, and the side effects are typically minor and transient. As with any injection procedure, there are risks of serious complications, but the incidence is rare. 2 Tieppo Francio V, Sayed D. Basivertebral Nerve Ablation. [Updated 2023 May 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK572127/ , 3 Conger A, Schuster NM, Cheng DS, et al. The Effectiveness of Intraosseous Basivertebral Nerve Radiofrequency Neurotomy for the Treatment of Chronic Low Back Pain in Patients with Modic Changes: A Systematic Review. Pain Med. 2021;22(5):1039-1054. doi:10.1093/pm/pnab040
In This Article:
- Basivertebral Nerve Ablation for Lower Back Pain
- Basivertebral Nerve Ablation Explained Step-by-Step
- Basivertebral Nerve Ablation Animation
Step 1: Diagnosis and Medical Clearance
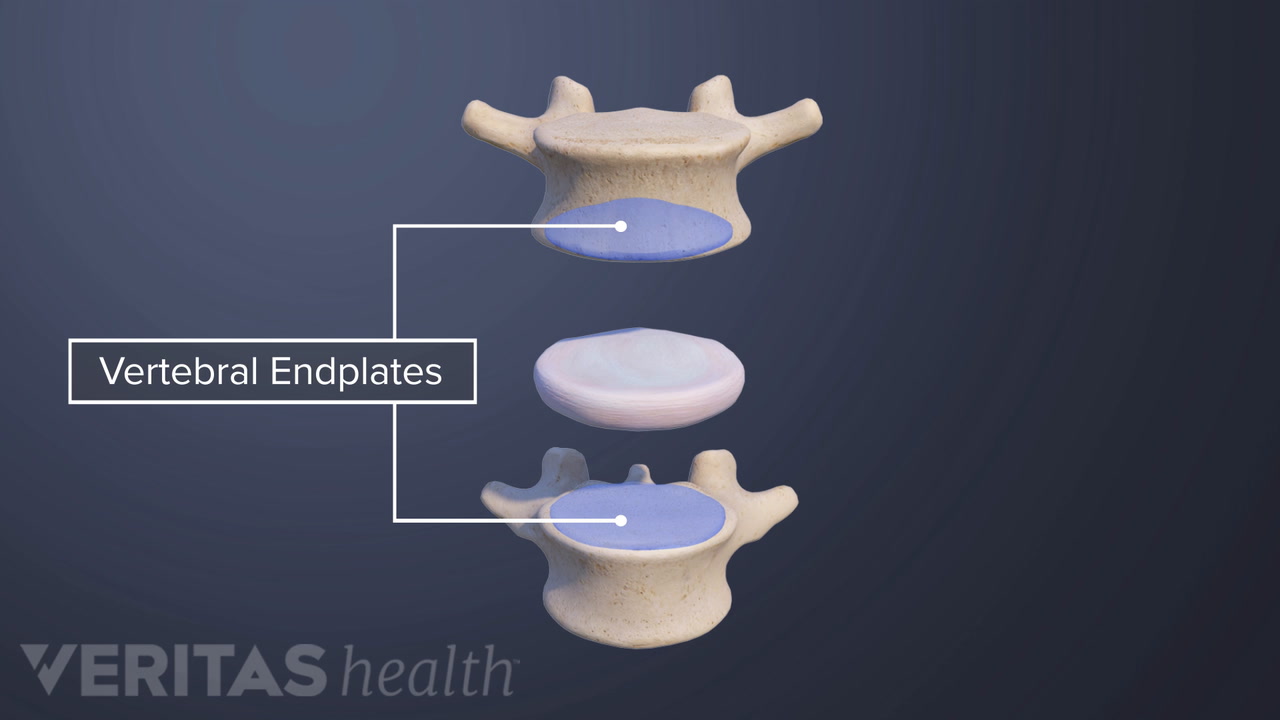
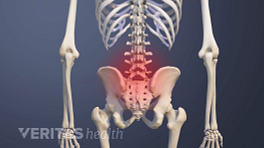
Basivertebral nerve ablation is only performed in patients diagnosed with vertebral endplate damage as the cause of their lower back pain, referred to as vertebrogenic pain.
Unlike the diagnostic process for non-specific lower back pain, which tends to be complex and less definitive, the diagnosis of vertebrogenic pain is confirmed with specific MRI findings (called Modic changes). 1 Sayed D, Naidu RK, Kiran Klaus Patel, et al. Best Practice Guidelines on the Diagnosis and Treatment of Vertebrogenic Pain with Basivertebral Nerve Ablation from the American Society of Pain and Neuroscience. 2022;Volume 15:2801-2819. doi:10.2147/jpr.s378544 , 2 Tieppo Francio V, Sayed D. Basivertebral Nerve Ablation. [Updated 2023 May 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK572127/
Steps for ensuring a correct diagnosis include 1 Sayed D, Naidu RK, Kiran Klaus Patel, et al. Best Practice Guidelines on the Diagnosis and Treatment of Vertebrogenic Pain with Basivertebral Nerve Ablation from the American Society of Pain and Neuroscience. 2022;Volume 15:2801-2819. doi:10.2147/jpr.s378544 , 2 Tieppo Francio V, Sayed D. Basivertebral Nerve Ablation. [Updated 2023 May 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK572127/ :
- Medical history to evaluate primary symptoms, conditions, and medications and to rule out alternative causes of pain that would necessitate a different treatment
- Physical examination to assess the patient’s suitability for the procedure, establish baseline pain and functional status, and to identify any contraindications
- Laboratory tests to rule out bleeding disorders and/or infection
- Imaging tests, specifically a magnetic resonance imaging (MRI) scan, to confirm the presence of Type 1 or Type 2 Modic changes
Importantly, a thorough evaluation evaluates the safety and potential risks of the ablation procedure for the individual patient. 1 Sayed D, Naidu RK, Kiran Klaus Patel, et al. Best Practice Guidelines on the Diagnosis and Treatment of Vertebrogenic Pain with Basivertebral Nerve Ablation from the American Society of Pain and Neuroscience. 2022;Volume 15:2801-2819. doi:10.2147/jpr.s378544
Step 2: Preparing for the BVN Ablation
Preparation in the days leading up to a BVN ablation includes requirements such as:
- Temporarily stopping or reducing the dose of blood-thinning medications 2 to 7 days before the procedure is sometimes advised to reduce the risk of excessive bleeding. 4 Smith CC, Schneider B, McCormick ZL, et al. Risks and Benefits of Ceasing or Continuing Anticoagulant Medication for Image-Guided Procedures for Spine Pain: A Systematic Review. Pain Med. 2018;19(3):438-448. doi:10.1093/pm/pnx152
- Informing the healthcare providers involved in the procedure of all current vitamins and supplements, as these products could potentially impact bleeding risk or sedating medications.
- Scheduling transportation and/or supervision after returning home due to the use of anesthesia and possibly sedating medications. 1 Sayed D, Naidu RK, Kiran Klaus Patel, et al. Best Practice Guidelines on the Diagnosis and Treatment of Vertebrogenic Pain with Basivertebral Nerve Ablation from the American Society of Pain and Neuroscience. 2022;Volume 15:2801-2819. doi:10.2147/jpr.s378544 , 2 Tieppo Francio V, Sayed D. Basivertebral Nerve Ablation. [Updated 2023 May 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK572127/
- Fasting on the day of the procedure is required if anesthesia or sedation will be used. 5 American Society of Anesthesiologists. Practice Guidelines for Preoperative Fasting and the Use of Pharmacologic Agents to Reduce the Risk of Pulmonary Aspiration: Application to Healthy Patients Undergoing Elective Procedures: An Updated Report by the American Society of Anesthesiologists Task Force on Preoperative Fasting and the Use of Pharmacologic Agents to Reduce the Risk of Pulmonary Aspiration. Anesthesiology. 2017;126(3):376-393. doi:10.1097/ALN.0000000000001452
Additionally, while not always required, quitting all forms of nicotine ingestion – smoking, vaping, chewing, nicotine replacement therapy – is encouraged to improve overall health, as nicotine impairs healing and increases the risk of complications. 6 An D, Ayob F, Rajaleelan W, Chung F, Wong J. Preoperative smoking cessation as part of surgical prehabilitation. Can J Anaesth. 2019;66(4):476-479. doi:10.1007/s12630-018-01283-7
To ensure safety, it is recommended to consult with the prescribing physician before discontinuing any medication or changing the dosage.
Step 3: The Basivertebral Nerve Ablation Procedure
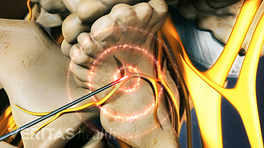
In BVN ablation, a heat lesion is created on the basivertebral nerve to prevent pain signals from reaching the brain.
On the day of the procedure, the basivertebral nerve ablation procedure is typically done as follows: 2 Tieppo Francio V, Sayed D. Basivertebral Nerve Ablation. [Updated 2023 May 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK572127/ , 7 Koreckij T, Kreiner S, Khalil JG, et al. Prospective, randomized, multicenter study of intraosseous basivertebral nerve ablation for the treatment of chronic low back pain: 24-Month treatment arm results. N Am Spine Soc J. 2021;8:100089. Published 2021 Oct 26. doi:10.1016/j.xnsj.2021.100089 :
- Premedication. An intravenous line is started, and patients are given a relaxing medication to produce moderate sedation. Patients are sometimes placed under general anesthesia, which requires additional monitoring and breathing support. A single dose of an antibiotic medication is also administered through this IV line to prevent surgical site infections.
- Positioning and preparation. The patient lies face-down on the procedure table, and imaging guidance called fluoroscopy is used to pinpoint the location for the ablation procedure. A local anesthetic is injected into the skin to numb the tissue in the targeted area.
- Creating the channel for the probe. A small incision (approximately 0.5 cm, or less than the length of one staple) is made in the lower back, and a thin instrument called an introducer cannula is inserted through the pedicle and into the vertebra.
- Radiofrequency probe placement. The radiofrequency probe is then inserted through the cannula to the precise area in the vertebral body where the basivertebral nerve is located.
- Ablation. The tip of the radiofrequency probe is heated and applied to the nerve for 7 to 15 minutes (depending on multiple factors) to create a heat lesion.
- Closing. The instruments are then removed, and the incision is closed using dissolvable stitches or surgical glue.
X-ray fluoroscopic guidance is used throughout the procedure to ensure the accuracy of probe placement. 2 Tieppo Francio V, Sayed D. Basivertebral Nerve Ablation. [Updated 2023 May 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK572127/ , 7 Koreckij T, Kreiner S, Khalil JG, et al. Prospective, randomized, multicenter study of intraosseous basivertebral nerve ablation for the treatment of chronic low back pain: 24-Month treatment arm results. N Am Spine Soc J. 2021;8:100089. Published 2021 Oct 26. doi:10.1016/j.xnsj.2021.100089
The entire BVN ablation procedure usually takes approximately 1 to 1 and ½ hours to perform.
Step 4: Following the Procedure
When the procedure is complete, patients are monitored until the effects of the medication dissipate, and it is considered safe for the patient to stand and walk. 2 Tieppo Francio V, Sayed D. Basivertebral Nerve Ablation. [Updated 2023 May 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK572127/
The patient can usually return home within a few hours of the procedure's completion.
Rest is advised on the day of a basivertebral nerve ablation, and limited physical activity is recommended for 48 hours following ablation. Patients are instructed to avoid 2 Tieppo Francio V, Sayed D. Basivertebral Nerve Ablation. [Updated 2023 May 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK572127/ :
- Lifting objects greater than 15 pounds
- Twisting and bending the spine
- Submerging in water (eg, bath, pool, or hot tub)
Patients are not allowed to drive for at least 24 hours after the procedure due to the use of sedating medication. If general anesthesia was administered, additional restrictions – such as operating machinery and drinking alcohol – for the first 24 to 48 hours after the procedure are recommended.
Most patients can resume light activities within 24 hours, and most can resume all regular activities after 48-hours. 2 Tieppo Francio V, Sayed D. Basivertebral Nerve Ablation. [Updated 2023 May 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK572127/
The incision site on the lower back should be monitored for signs of infection and kept clean and dry as it heals, which usually takes several days. 2 Tieppo Francio V, Sayed D. Basivertebral Nerve Ablation. [Updated 2023 May 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK572127/
Potential Side Effects
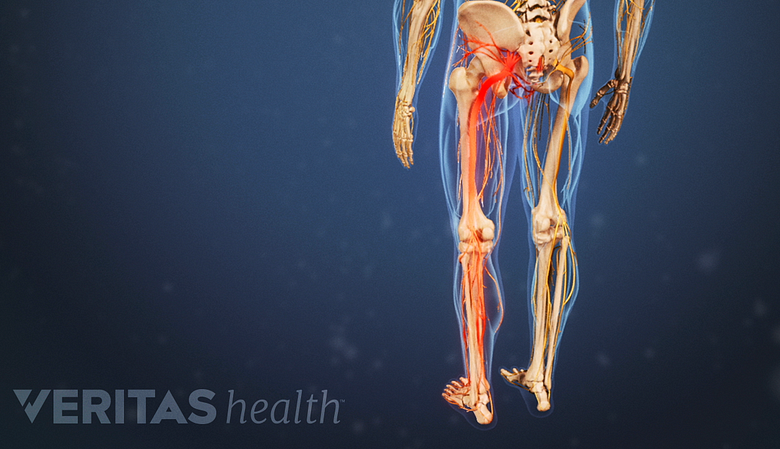
Radiating pain, numbness, and/or weakness in one or both legs is a potential side effect of BVN ablation.
Certain side effects occur in approximately 10% of patients, which include but are not limited to 3 Conger A, Schuster NM, Cheng DS, et al. The Effectiveness of Intraosseous Basivertebral Nerve Radiofrequency Neurotomy for the Treatment of Chronic Low Back Pain in Patients with Modic Changes: A Systematic Review. Pain Med. 2021;22(5):1039-1054. doi:10.1093/pm/pnab040 :
- Pain or soreness at the injection site
- Pain in the lower back and/or leg
- Numbness or tingling in the leg, back, and/or buttocks
In most cases, these side effects resolve within 2 to 3 months. 3 Conger A, Schuster NM, Cheng DS, et al. The Effectiveness of Intraosseous Basivertebral Nerve Radiofrequency Neurotomy for the Treatment of Chronic Low Back Pain in Patients with Modic Changes: A Systematic Review. Pain Med. 2021;22(5):1039-1054. doi:10.1093/pm/pnab040
It is possible for patients to experience increased pain initially after the procedure due to the insertion of the cannula and probe into an area already inflamed and in pain. This pain should be transient and resolve in a few days or weeks.
Over-the-counter and/or prescription pain medications, ice packs, or heat are helpful in managing the side effects of pain. 2 Tieppo Francio V, Sayed D. Basivertebral Nerve Ablation. [Updated 2023 May 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK572127/ For increased pain or any concerning symptoms, patients are advised to consult with their treating physician.
Potential Risks and Complications
As with any medical procedure, there is a risk of failure and continued pain.
Serious adverse events are reported in less than 1% of patients and include 3 Conger A, Schuster NM, Cheng DS, et al. The Effectiveness of Intraosseous Basivertebral Nerve Radiofrequency Neurotomy for the Treatment of Chronic Low Back Pain in Patients with Modic Changes: A Systematic Review. Pain Med. 2021;22(5):1039-1054. doi:10.1093/pm/pnab040 , 7 Koreckij T, Kreiner S, Khalil JG, et al. Prospective, randomized, multicenter study of intraosseous basivertebral nerve ablation for the treatment of chronic low back pain: 24-Month treatment arm results. N Am Spine Soc J. 2021;8:100089. Published 2021 Oct 26. doi:10.1016/j.xnsj.2021.100089 :
- Nerve root irritation and sciatica pain (lumbar radiculopathy)
- Bleeding into the abdominal space (retroperitoneal hemorrhage)
- Vertebral compression fracture
- Urinary retention
As this procedure is relatively new, additional research is needed to characterize the duration of pain relief, when and if the procedure can be repeated if pain returns and the potential risks and long-term safety profile.
It is advisable to discuss the risks, benefits, complications, and alternative treatments with a specialist who performs the procedure before considering vertebral endplate injections.
- 1 Sayed D, Naidu RK, Kiran Klaus Patel, et al. Best Practice Guidelines on the Diagnosis and Treatment of Vertebrogenic Pain with Basivertebral Nerve Ablation from the American Society of Pain and Neuroscience. 2022;Volume 15:2801-2819. doi:10.2147/jpr.s378544
- 2 Tieppo Francio V, Sayed D. Basivertebral Nerve Ablation. [Updated 2023 May 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK572127/
- 3 Conger A, Schuster NM, Cheng DS, et al. The Effectiveness of Intraosseous Basivertebral Nerve Radiofrequency Neurotomy for the Treatment of Chronic Low Back Pain in Patients with Modic Changes: A Systematic Review. Pain Med. 2021;22(5):1039-1054. doi:10.1093/pm/pnab040
- 4 Smith CC, Schneider B, McCormick ZL, et al. Risks and Benefits of Ceasing or Continuing Anticoagulant Medication for Image-Guided Procedures for Spine Pain: A Systematic Review. Pain Med. 2018;19(3):438-448. doi:10.1093/pm/pnx152
- 5 American Society of Anesthesiologists. Practice Guidelines for Preoperative Fasting and the Use of Pharmacologic Agents to Reduce the Risk of Pulmonary Aspiration: Application to Healthy Patients Undergoing Elective Procedures: An Updated Report by the American Society of Anesthesiologists Task Force on Preoperative Fasting and the Use of Pharmacologic Agents to Reduce the Risk of Pulmonary Aspiration. Anesthesiology. 2017;126(3):376-393. doi:10.1097/ALN.0000000000001452
- 6 An D, Ayob F, Rajaleelan W, Chung F, Wong J. Preoperative smoking cessation as part of surgical prehabilitation. Can J Anaesth. 2019;66(4):476-479. doi:10.1007/s12630-018-01283-7
- 7 Koreckij T, Kreiner S, Khalil JG, et al. Prospective, randomized, multicenter study of intraosseous basivertebral nerve ablation for the treatment of chronic low back pain: 24-Month treatment arm results. N Am Spine Soc J. 2021;8:100089. Published 2021 Oct 26. doi:10.1016/j.xnsj.2021.100089