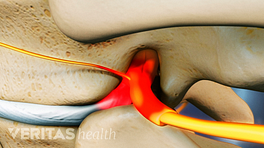
The first step in diagnosing a thoracic herniated disc always includes a good patient medical history and physical examination. The spine physician will begin by getting a better understanding of the patient’s symptoms, including the:
- Location of the pain
- Severity of the pain
- Type of pain (numbness, weakness, burning, etc.).
The physician will often follow up by learning if any injuries occurred prior to the thoracic back pain or if any other problems (weight loss, fevers, illnesses, difficulty urinating) were recently present before the upper back pain. The physician will then perform a physical examination.
This combination of the patient’s description of how the pain feels, where it occurs, when it occurs, etc., as well as the spine physician’s physical examination, should yield clues to help localize the lesion to the thoracic spine.
In This Article:
Thoracic Herniated Disc Diagnostic Tests
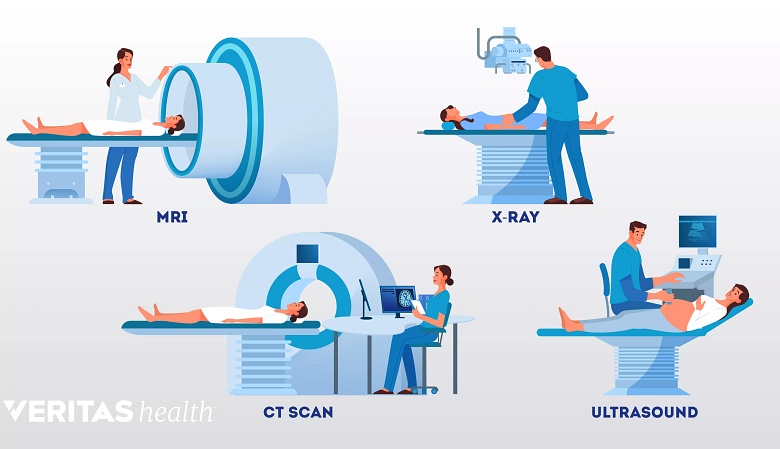
Several imaging techniques may be used to diagnose thoracic herniated disc.
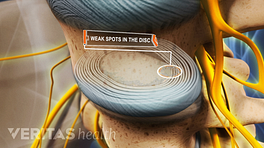
If a thoracic herniated disc is suspected as the underlying cause of the pain, there are several diagnostic tests that can confirm the diagnosis and provide additional information, including
- X-rays – While plain x-rays will not show a thoracic herniated disc, they may be used to help localize injuries in cases of trauma as well as aid in identifying spinal instability.
- Magnetic Resonance Imaging (MRI) – An MRI utilizes a powerful magnet attached to a computer to produce images of the spine. A painless and often accurate test, an MRI scan is the most useful imaging tool to identify disc pathology.
In some cases, a physician may seek even more detailed information beyond an MRI and order the following tests:
- Computed Tomography (CT) – A CT scan involves the use of a computer that constructs a cross-dimensional, three-dimensional image of the spine after processing data from an X-ray beam rotated around the spine.
- Myelogram – A myelogram involves the injection of a special dye into the spinal column, with an X-ray taken to examine any pressure on the spine and any problems with the discs or vertebrae.
In cases where an MRI scan is contraindicated, a post-myelogram CT can help identify an area of external compression, but it will not yield information about injury within the substance of the cord (myelomalacia).