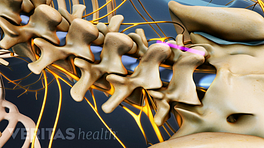
The XLIF (extreme lateral interbody fusion) surgery treats lower back disorders by fusing the affected spinal segments and eliminating motion in those segments. The surgical approach is taken from the side of the lower spine, and up to two adjacent spinal segments may be treated using this procedure.
A single-level XLIF procedure takes approximately an hour to perform from the time of incision to the time that the surgeon closes the lateral incision with sutures (stitches). Additional time will be required if screws and rods are placed from the back in a separate procedure.
In This Article:
- XLIF: Lumbar Spinal Fusion
- Description of XLIF Surgery
Step-by-Step XLIF Procedure
Prior to any form of lumbar spine fusion, medical clearance is obtained and patients who smoke are required to stop. Patients may donate their own blood, if they choose, to be used at the time of surgery.
More specifically, a step-by-step approach to the XLIF surgical procedure involves:
- Preparing the patient. After receiving general anesthesia, the patient is positioned lying on his or her side. Fluoroscopy images (or live x-rays) are taken to locate the disc that will be removed. The surgeon marks the skin directly above the disc.
- Accessing the spine. A small incision (cut) is made in the flank (low back region of the trunk). The surgeon uses his or her finger to push away the peritoneum (sac covering the abdominal organs) from the abdominal wall. A tube-like instrument called a dilator is inserted into the peritoneum and advanced near the disc. Fluoroscopy images are taken to ensure that the dilator is in a suitable position above the disc. A probe (blunt tool) is inserted through the psoas, a large muscle, which runs along the front part of the lower spine, wraps around the pelvic area, and attaches to the hip. The probe helps avoid interrupting the nerves.
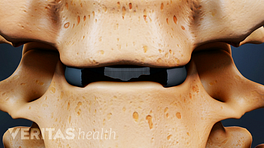
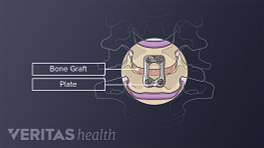
- Replacing the disc with an interbody cage. A complete discectomy is performed to remove the damaged disc. An interbody cage is inserted through the same incision from the side. The cage helps hold the vertebrae in their proper position to preserve the disc height (space between adjacent vertebral bodies) and maintain spinal alignment. Some cages are also filled with bone grafts to facilitate bone growth and fusion. X-rays are taken to ensure that the implant is in the right position.
- Closing the wound. Sutures (stitches) are used to close the incision.
- Using posterior fixation. In most cases, pedicle screws are placed from the back, fixated above and below the disc level, and connected by rods.
-
Patients are closely monitored for a few hours until the effect of general anesthesia wears off and they regain consciousness.
Nerve monitoring during XLIF
Several nerves exiting the spinal column are close to the psoas muscle in the front part of the lower spine and can even run right over its surface. During an XLIF procedure, it is critical that the surgeon monitors real-time information about the position of these nerves relative to his or her surgical instruments.
Recovery After XLIF
Recovery after an XLIF surgery depends on several factors such as the number of vertebral levels that were fused, severity of the lower back problem, and the patient's age and overall health.
In general, XLIF surgical recovery may include:
- Pain and bruising at the incision sites after surgery, which can be controlled with oral pain medication and eventually resolve after a few weeks
- Soreness in the front part of the thigh, which lasts for a few days to weeks and eventually resolves
- Improvement of presurgical symptoms (such as leg pain) immediately or gradually after surgery
Patients are usually able to get up and walk around a few hours after surgery because the XLIF approach splits the muscle fibers in the psoas rather than completely cutting them (which may prolong the recovery). Most patients who undergo an XLIF procedure will return home the same day or the day after the surgery; others may require staying for a few days or a week in the hospital. Patients are discharged once the pain is under control and they can safely walk.
See Hospital Care After Spinal Fusion Surgery (2 to 4 Days)
Return to daily activities
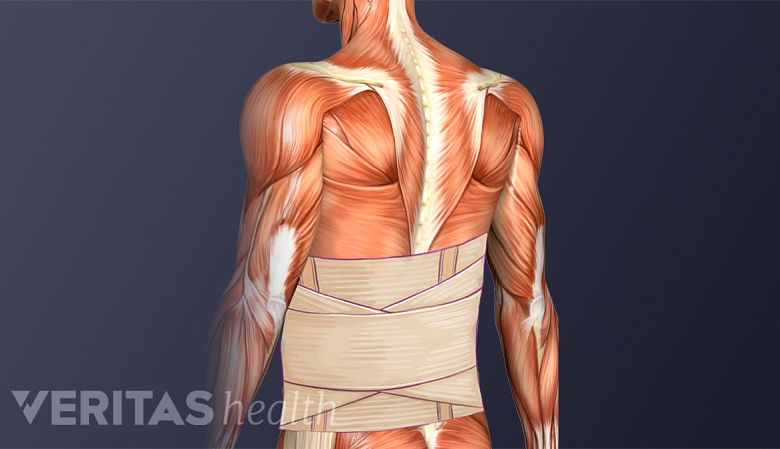
A lumbar brace stabilizes the spine and assists in the recovery process.
A back brace may be recommended for the first few weeks after surgery to help stabilize the spine and assist in the fusion process. Walking is usually recommended the next day after surgery. More vigorous activities, such as an elliptical trainer, may be safe around 2 weeks after surgery; running may be safe about 6 weeks after surgery. Most patients can typically return to their normal activities within a few months of surgery. The presence of other spinal conditions and the general health and well-being of the patient plays an important role in defining the time taken to return to all routine activities.
Post-surgical visits are typically scheduled every few weeks or months. During these visits, the surgeon typically checks for signs of healing or infection and addresses any possible concerns regarding activity or pain management. The visits may occur more often or less often and are typically tailored to the needs of the patient.
See Spinal Fusion Surgery Recovery: 1 to 4 Weeks After
A guided physical therapy program may be recommended for the initial few weeks to help regain strength and assist with routine physical activities.
Read more about Postoperative Care for Spinal Fusion Surgery